Chapter 4
Facilitating Bone Growth and Strength
In This Chapter
 Building strong bones with vitamin D
Building strong bones with vitamin D
 Dealing with rickets and osteomalacia
Dealing with rickets and osteomalacia
 Combating osteoporosis
Combating osteoporosis
 Keeping your teeth strong
Keeping your teeth strong
Between the years 1645 and 1982, experts thought vitamin D’s only role was to enhance calcium absorption and facilitate bone growth and strength. Since 1982, however, vitamin D has been given much more credit, but if vitamin D did nothing more than manage calcium and improve bone, that would truly be enough.
In this chapter, you discover how vitamin D deficiency prevents the normal production of bone. You also find out how osteoporosis and your teeth tie into vitamin D. Finally, you discover how to check and treat your child for vitamin D deficiency.
Recognizing the Importance of Bone
Bone isn’t an inert organ. It has critical functions in the body, which can be broken down (no pun intended) into three main categories: mechanical, synthetic, and metabolic.
Mechanical functions of bone
Bone provides four major mechanical functions:
 Movement: Bone, along with its ligaments, tendons, and joints, allows the body to move through space.
Movement: Bone, along with its ligaments, tendons, and joints, allows the body to move through space.
 Protection: Bone protects major organs from damage, particularly the brain and the heart and lungs.
Protection: Bone protects major organs from damage, particularly the brain and the heart and lungs.
 Shape: The facial bones, teeth, skull, rib cage, and other bones give shape to the body.
Shape: The facial bones, teeth, skull, rib cage, and other bones give shape to the body.
 Sound transmission: Bones in the inner ear transmit sound.
Sound transmission: Bones in the inner ear transmit sound.
Synthetic function of bone
All the blood cells of the body are produced within the cavities of bone in tissue called marrow. The major blood cells include the following:
 Red blood cells
Red blood cells
 White blood cells
White blood cells
 Platelets
Platelets
Bone also produces other kinds of cells, including mesenchymal stem cells, which can become bone cells and muscle cells.
Metabolic functions of bone
Bone serves a number of metabolic functions that are essential for normal functioning of the body. Without these functions, living organisms couldn’t exist. Consider these key functions:
 Mineral storage: Bone is the major storage site for calcium, phosphorus, and magnesium.
Mineral storage: Bone is the major storage site for calcium, phosphorus, and magnesium.
 Acid-base balance: The blood must be at a pH that is slightly alkaline. Bone helps maintain the blood pH by releasing or absorbing alkaline chemicals (mostly phosphate).
Acid-base balance: The blood must be at a pH that is slightly alkaline. Bone helps maintain the blood pH by releasing or absorbing alkaline chemicals (mostly phosphate).
 Detoxification: Bone can accumulate toxic substances, to keep them from having a negative effect on the body.
Detoxification: Bone can accumulate toxic substances, to keep them from having a negative effect on the body.
 Endocrine organ function: Bone releases several hormones that regulate the way the body uses calcium and phosphorus.
Endocrine organ function: Bone releases several hormones that regulate the way the body uses calcium and phosphorus.
Building Strong Bones with Vitamin D
Even before we knew what vitamin D was, we’ve understood that it is important for bone. In the industrial age, when the skies of many cities were dark from soot, the number of rickets cases exploded. Doctors learned that cod liver oil could reverse and prevent rickets. Now we know that the soot stopped the UV rays of the sun and prevented the skin from producing vitamin D. We also know that vitamin D was the active chemical in cod liver oil that prevented rickets.
In the following sections, I explain how your body creates bone tissue, describe how your bones grow, and cover the minerals your body needs for bone growth.
What is bone?
Bones are very strong but relatively lightweight (despite the claims of some “large-boned” people). To make good bone you need a protein scaffold; then you need to harden the scaffold with crystals of calcium and phosphorus.
There are two different types of bone (see Figure 4-1):
 Cortical, or compact, bone: This is the hard, dense bone that makes up the tube part of the long bones such as the femur that is in your thigh. It also makes up your skull and the outer part of the ribs and vertebrae. The marrow lives in the center of the long bones and ribs and is protected by cortical bone.
Cortical, or compact, bone: This is the hard, dense bone that makes up the tube part of the long bones such as the femur that is in your thigh. It also makes up your skull and the outer part of the ribs and vertebrae. The marrow lives in the center of the long bones and ribs and is protected by cortical bone.
 Cancellous, or trabecular, bone: This type of bone is more porous than cortical bone. It’s found at the end of long bones and inside the vertebrae. This woven structure works like a shock absorber. The marrow can be mixed within the pores of trabecular bone.
Cancellous, or trabecular, bone: This type of bone is more porous than cortical bone. It’s found at the end of long bones and inside the vertebrae. This woven structure works like a shock absorber. The marrow can be mixed within the pores of trabecular bone.
Good, strong bone is produced in two different ways. When you’re growing, the ends of your bones grow because of the action of cells called chondrocytes. These cells live in the part of the long bones called the “growth plate,” a structure at the end of the long bones. The other way new bone is made is by another bone-forming cell called osteoblasts. These cells live on the surface of bone. Both osteoblasts and chondrocytes make proteins that serve as the scaffold for bone.
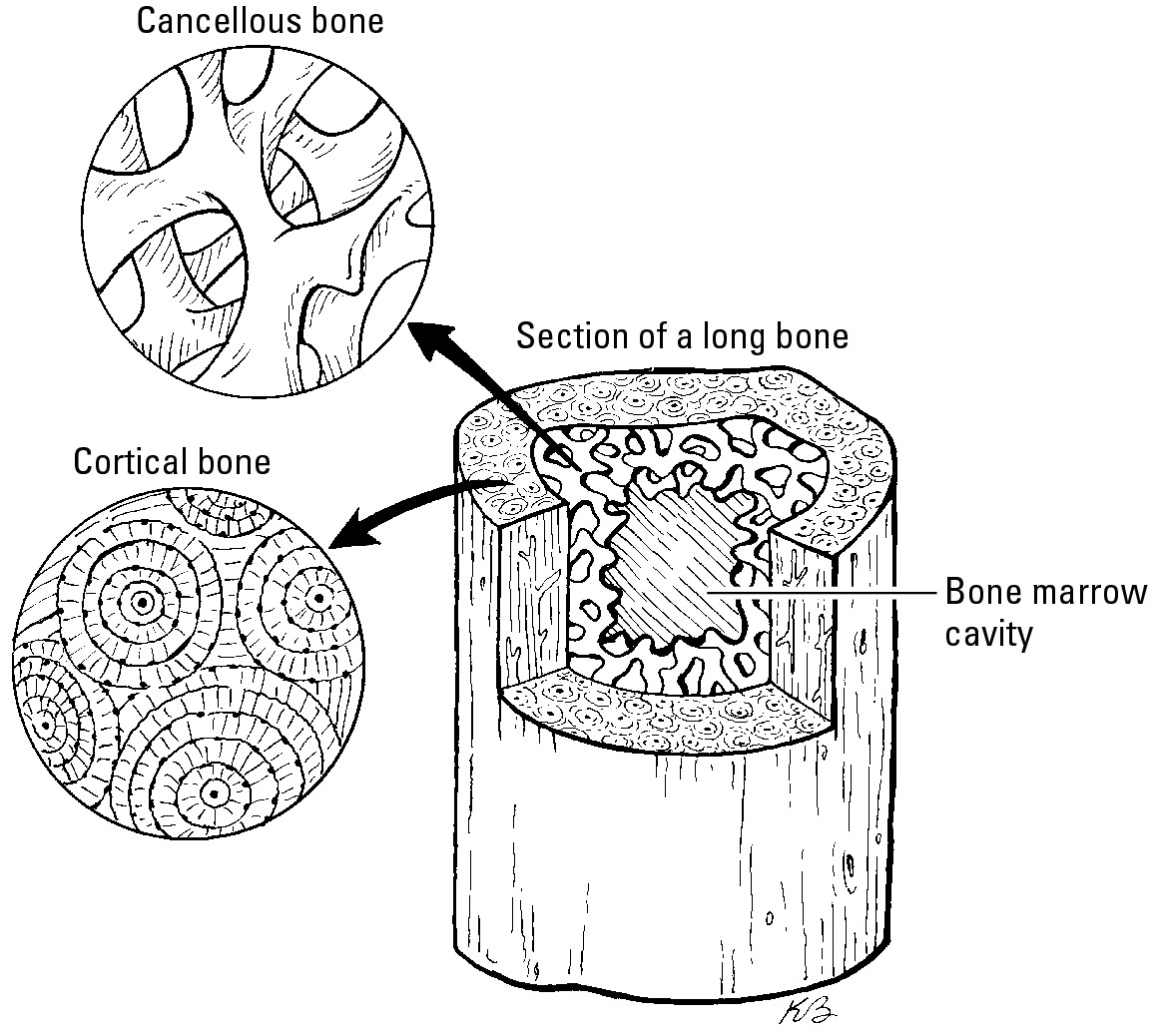
Figure 4-1: Cortical and cancellous bone.
Another interesting fact about osteoblasts is that as the bone mineralizes, the osteoblast can get embedded in the newly formed bone. When this happens they change and become osteocytes. Osteocytes are like sensors within the bone that detect when the mineralized bone has tiny stress fractures. This leads the osteocytes to send signals to a cell type called osteoclasts, whose function is to dissolve bone. These cells reabsorb the bone either when bone needs repairing or when the body needs calcium or phosphorus. After they do their job, the lost bone is replaced by osteoblasts (the bone forming cells). As this process occurs, the bone retains its shape. The entire process is called bone remodeling.
 It provides a source of calcium to keep the blood calcium stable.
It provides a source of calcium to keep the blood calcium stable.
 It maintains the strength of the bone as a structural material.
It maintains the strength of the bone as a structural material.
Vitamin D brings in the calcium and promotes bone growth
Without enough vitamin D in the body, the bones are in trouble. This is because calcitriol (active vitamin D or 1,25(OH)2 vitamin D) has a number of roles in the control of how your body uses calcium as well as in the production of healthy bone:
 In the intestine, calcitriol induces the production of proteins that cause calcium to be absorbed from food into the bloodstream. Much of the calcium absorbed ends up being taken up by the protein scaffold that osteoblasts make.
In the intestine, calcitriol induces the production of proteins that cause calcium to be absorbed from food into the bloodstream. Much of the calcium absorbed ends up being taken up by the protein scaffold that osteoblasts make.
 In the parathyroid gland, calcitriol suppresses the production of more parathyroid hormone. Remember, parathyroid hormone is a signal to break down bone and free up calcium. When your vitamin D status is too low, your body can’t make calcitriol and parathyroid hormone levels go up.
In the parathyroid gland, calcitriol suppresses the production of more parathyroid hormone. Remember, parathyroid hormone is a signal to break down bone and free up calcium. When your vitamin D status is too low, your body can’t make calcitriol and parathyroid hormone levels go up.
 In the kidneys, calcitriol induces the production of proteins that keep calcium from being excreted in the urine. By keeping more calcium (but not too much!) in the body, you protect your bones.
In the kidneys, calcitriol induces the production of proteins that keep calcium from being excreted in the urine. By keeping more calcium (but not too much!) in the body, you protect your bones.
 In the bone, vitamin D causes the osteoblasts to produce more of the protein scaffold that is then mineralized to make mature bone.
In the bone, vitamin D causes the osteoblasts to produce more of the protein scaffold that is then mineralized to make mature bone.
Reckoning with Rickets and Osteomalacia
Rickets is a condition resulting from inadequate mineralization of all the bones. It leads to weak, flexible bones. In the long bones of the leg, this means they can’t support the weight of the body so that they curve abnormally. Soft, rachitic bones don’t properly protect the body, either, as with an abnormally soft skull and the brain. Hereditary rickets can be caused by genetic reasons or by a poor diet. When either vitamin D or calcium is deficient in growing children, they may develop nutritional rickets. Figure 4-2 shows the spine and legs of a child with rickets.
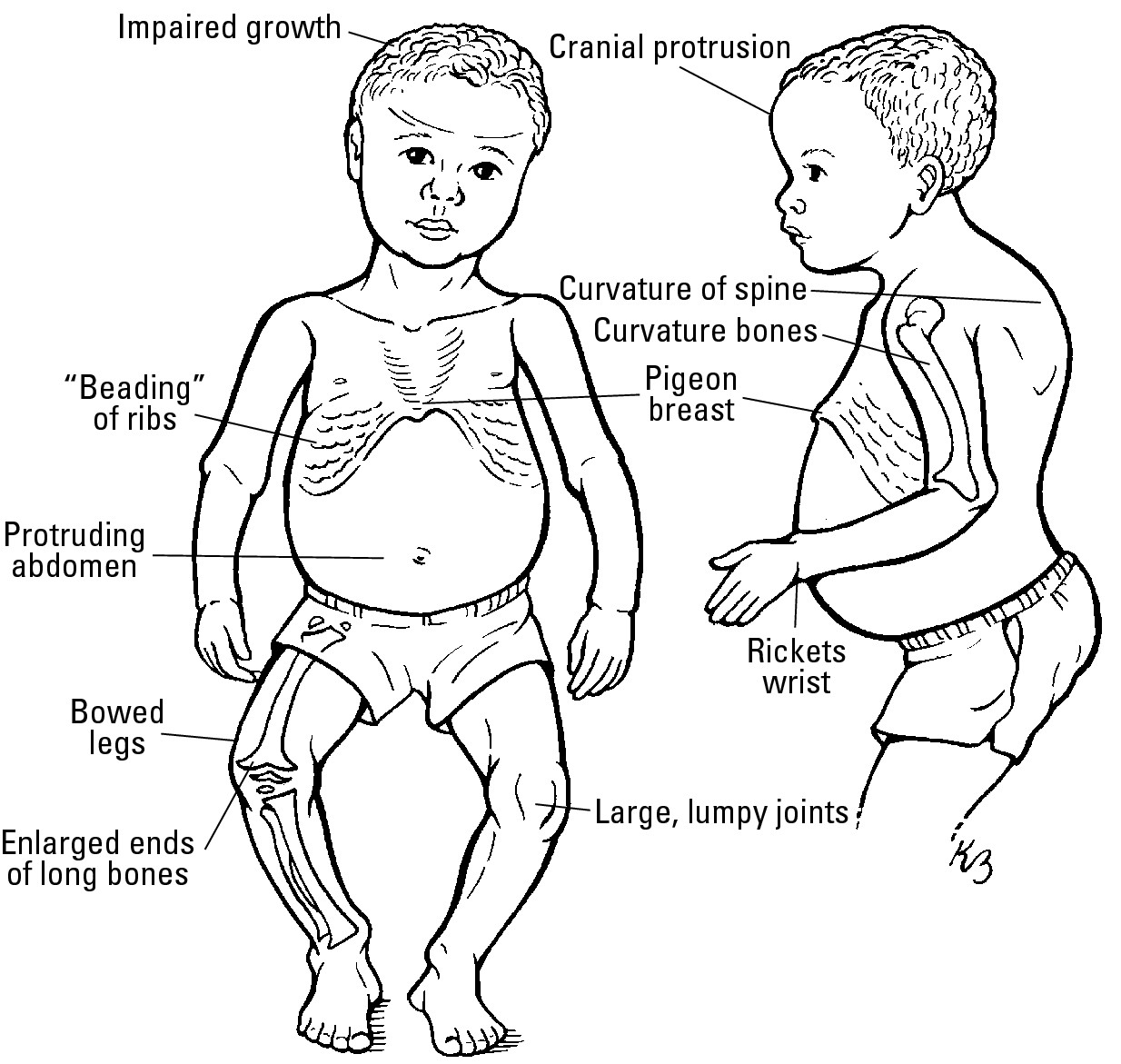
Figure 4-2: Spine and legs of a child with rickets.
Although rickets is common throughout the world, it remains rare in the United States. In the last decade, however, rickets has become more common among certain segments of the American population. Rickets typically occurs in the United States in children who:
 Are African American (because this group typically makes little vitamin D even when exposed to the sun)
Are African American (because this group typically makes little vitamin D even when exposed to the sun)
 Are breastfed exclusively
Are breastfed exclusively
 Are kept out of the sun
Are kept out of the sun
 Have mothers who are severely deficient in vitamin D while they are pregnant and during breastfeeding
Have mothers who are severely deficient in vitamin D while they are pregnant and during breastfeeding
Deficient vitamin D levels result in reduced calcium absorption, to only 10 to 15 percent of dietary calcium, and less than 50 percent absorption of dietary phosphorus. See Chapter 3 for more on the place of phosphorus in bone development. This lower level of calcium and phosphorus absorption isn’t enough to keep serum calcium and phosphorus levels normal. As a result, the protein scaffold made by osteoblasts can’t be mineralized.
Studies in children and animals with nutritional or genetic forms of rickets show that the role of vitamin D in preventing rickets is simply to promote intestinal calcium absorption. It is actually the lack of calcium that is to blame for the weak bones, and vitamin D’s job is to make sure we absorb enough calcium from the diet to protect bone. In fact, the role of vitamin D for bone can be almost completely bypassed by giving calcium as an intravenous infusion directly into the blood or by giving very high calcium diets or calcium supplements to children or animals. These calcium treatments will let the bones mineralize, but they don’t straighten the bones if they’ve already curved.
Although rickets is suspected when the child has the characteristic shape shown in Figure 4-2, doctors can confirm the diagnosis with a blood test that shows low serum calcium and bone X-rays that show poor mineralization and the characteristic bowing shape.
If severe vitamin D deficiency develops after the bones have been formed (in adults), the condition is called osteomalacia. This condition also occurs when the protein scaffold in bone isn’t mineralized. The difference is that only the new scaffold produced during bone remodeling isn’t mineralized, so the condition takes longer to develop.
Describing signs and symptoms
Children from age six months to three years are especially at risk of rickets because their bones are growing very fast. The condition rarely appears in newborns.
Signs and symptoms of rickets include the following:
 Abnormal growth of long bones with short stature
Abnormal growth of long bones with short stature
 Bone pain involving the arms, legs, pelvis, and spine
Bone pain involving the arms, legs, pelvis, and spine
 Dental abnormalities, including delayed formation of teeth, increased cavities, and holes in the enamel (see the section “Helping Your Teeth Grow,” later in this chapter)
Dental abnormalities, including delayed formation of teeth, increased cavities, and holes in the enamel (see the section “Helping Your Teeth Grow,” later in this chapter)
 Enlargement of the ends of bones
Enlargement of the ends of bones
 Muscle cramps
Muscle cramps
 Weak muscles especially at the hips and shoulders (limb girdle muscles)
Weak muscles especially at the hips and shoulders (limb girdle muscles)
 Skeletal abnormalities, including
Skeletal abnormalities, including
• Abnormal shape of the skull
• Bowlegs
• Pigeon chest
• Abnormal spine curvature
 Uncontrolled muscle spasms due to low calcium
Uncontrolled muscle spasms due to low calcium
Osteomalacia tends to have milder symptoms than rickets. Signs and symptoms of osteomalacia include the following:
 Bone bending
Bone bending
 Bone pain
Bone pain
 Bone tenderness
Bone tenderness
 Compressed vertebrae
Compressed vertebrae
 Easy fracturing
Easy fracturing
 Muscle weakness
Muscle weakness
The bones are less rigid in osteomalacia. Patients are weak and can’t climb stairs or get out of a chair without using their arms because their serum calcium levels are low and their muscles are weak. Some patients complain only of chronic fatigue, which makes diagnosis difficult. As in rickets, blood tests in osteomalacia for calcium and phosphate are low. This finding, along with low levels of serum 25-hydroxyvitamin D, help confirm the diagnosis.
Exploring the causes
As I said earlier in this chapter, nutritional rickets can be caused either by a diet very low in calcium or due to low vitamin D status. Sometimes both occur together. At other times, as in some Asian countries, high intake of a chemical found in some plants and grains called phytate prevents what would otherwise be a reasonable dietary intake of calcium from being absorbed. Phytate is a phosphate-rich chemical that binds calcium and other minerals and this limits the ability of the minerals from crossing the intestine. When vitamin D levels are inadequate, insufficient uptake of calcium occurs and the bones aren’t mineralized sufficiently. Parathyroid hormone also increases in an effort to maintain normal serum calcium, and so the bones become further stripped of calcium and weakened.
Although lack of vitamin D is the most common reason for developing rickets or osteomalacia in the United States, other causes exist and are seen in the United States and in developing countries:
 Lack of dietary calcium: Without sufficient calcium, the bones don’t mineralize properly. Rickets caused by calcium deficiency happens in developing countries where the diet is generally low in calcium, high in phytate, and where kids don’t have access to dairy foods.
Lack of dietary calcium: Without sufficient calcium, the bones don’t mineralize properly. Rickets caused by calcium deficiency happens in developing countries where the diet is generally low in calcium, high in phytate, and where kids don’t have access to dairy foods.
 Lack of dietary phosphorus: The mineral that’s added to bone is calcium phosphate, so a lack of phosphorus prevents mineralization.
Lack of dietary phosphorus: The mineral that’s added to bone is calcium phosphate, so a lack of phosphorus prevents mineralization.
 Hereditary rickets: There are several genetic forms of rickets that affect vitamin D metabolism or action. Type IA or “Pseudovitamin D deficiency” genetic rickets is caused by a defect in the gene that makes calcitriol in the kidneys. Type IB genetic rickets is caused by a defect in the gene that makes 25-hydroxyvitamin D, the precursor for calcitriol. Type II genetic rickets is caused by a defect in the gene for the protein (vitamin D receptor) that binds calcitriol to regulate how it works at the molecular level. The end result of both conditions is that the body thinks it is vitamin D deficient. Fortunately, both of these conditions are rare. And as mentioned, both can be treated with calcium alone, either orally or intravenously.
Hereditary rickets: There are several genetic forms of rickets that affect vitamin D metabolism or action. Type IA or “Pseudovitamin D deficiency” genetic rickets is caused by a defect in the gene that makes calcitriol in the kidneys. Type IB genetic rickets is caused by a defect in the gene that makes 25-hydroxyvitamin D, the precursor for calcitriol. Type II genetic rickets is caused by a defect in the gene for the protein (vitamin D receptor) that binds calcitriol to regulate how it works at the molecular level. The end result of both conditions is that the body thinks it is vitamin D deficient. Fortunately, both of these conditions are rare. And as mentioned, both can be treated with calcium alone, either orally or intravenously.
 Renal tubular acidosis: In this disease, the kidneys fail to rid the body of acid. The blood becomes more acidic, which dissolves the calcium phosphate crystals in bone and makes it so more calcium is lost in the urine. As a result, the minerals in bone are lost and they become less dense and weaker.
Renal tubular acidosis: In this disease, the kidneys fail to rid the body of acid. The blood becomes more acidic, which dissolves the calcium phosphate crystals in bone and makes it so more calcium is lost in the urine. As a result, the minerals in bone are lost and they become less dense and weaker.
 Inability to absorb fats from the intestine: Vitamin D is a compound that dissolves in fat. As a result, it is absorbed from the diet along with fat. If you can’t absorb fat, this leads to vitamin D deficiency and rickets. This can occur because of diseases such as Crohn’s and bowel resections.
Inability to absorb fats from the intestine: Vitamin D is a compound that dissolves in fat. As a result, it is absorbed from the diet along with fat. If you can’t absorb fat, this leads to vitamin D deficiency and rickets. This can occur because of diseases such as Crohn’s and bowel resections.
Treating the condition
Treatment depends on the source of the condition. If a patient lacks vitamin D, doctors can rapidly correct the condition with a supplement. For example, doctors can give vitamin D as a 50,000 IU dose each week for four to six weeks. This will correct the low vitamin D status and allow the body to make calcitriol again. In addition, doctors will give 500 mg of calcium and 200 mg of phosphorus daily until blood levels of these minerals return to normal.
Doctors treat renal tubular acidosis by giving bicarbonate to counteract the acidity of the blood to bring the pH to a more normal level. This helps protect bone by keeping calcium from being lost in the urine.
If fats can’t be absorbed from the intestine, the patient can receive vitamin D by injection on a monthly or quarterly basis (this preparation is no longer available in Canada, though). Sometimes very high doses of vitamin D (for example, 50,000 IU daily) can be used to achieve adequate 25-hydroxyvitamin D levels in patients with short bowel or severe malabsorption, or the patient can be treated with UV (either through sunlight exposure or UV lamps under the guidance of a dermatologist).
If a kidney defect prevents synthesis of active vitamin D, physicians can give calcitriol by direct injection. Another form of vitamin D, 1-alpha-cholecalciferol, can be given which becomes activated by the liver without requiring the kidneys.
Managing Osteoporosis
Osteoporosis is a brittle bone disease in which both the structure of the bone and its mineralization are reduced. As a result, people with this disease are more likely to experience a bone fracture sometime in their life. Osteoporosis is the most common bone disease, occurring in one of every three women over age 50. Even men aren’t immune to osteoporosis; 1 in 12 men over 50 suffer from the disease.
Still, osteoporosis has its greatest impact on women. At menopause, which usually happens around the midcentury mark, women begin to lose bone at an accelerated rate. If they don’t start menopause with plenty of bone, they may lose so much bone that they develop osteoporosis. Ultimately, there are many causes for osteoporosis; some of the disease is caused by poor nutrition. Some women who didn’t start menopause with plenty of bone may have lacked vitamin D during the many years of their life.
Osteoporosis generally doesn’t produce symptoms until a fracture occurs. If a vertebra in the spine collapses from lack of strength, the person may experience sudden pain in the back. If several vertebra collapse, dowager’s hump, a forward bending of the spine that’s also known as kyphosis, may develop. (Figure 4-3a shows a normal spine, and Figure 4-3b shows a dowager’s hump.) The other common fracture is a hip fracture.
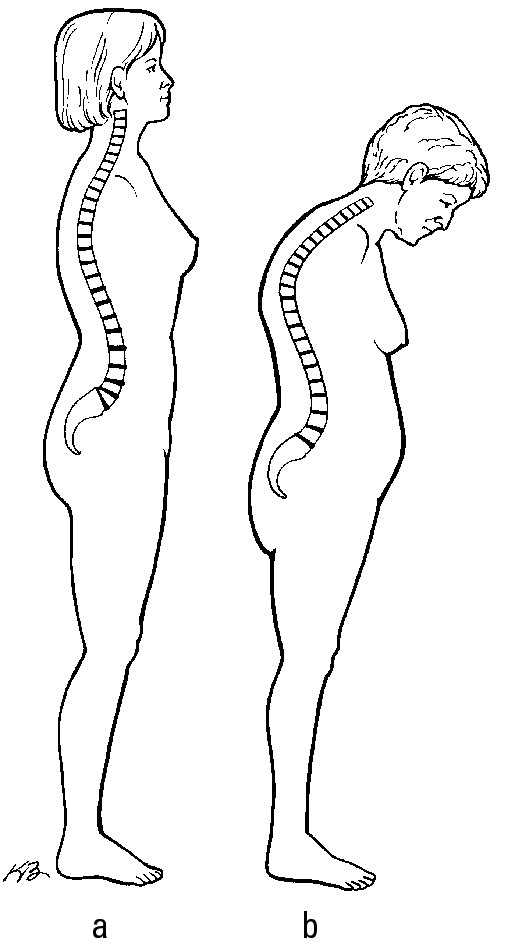
Figure 4-3: A normal spine and a dowager’s hump.
Osteoporosis is a disease of the elderly. One patient waited so long in the doctor’s waiting room that she told the doctor when she was finally seen, “It’s a shame you couldn’t have seen my disease in its early stages.”
For more information about osteoporosis, pick up a copy of Osteoporosis For Dummies (Wiley), by Carolyn Riester O’Connor, MD, and Sharon Perkins, RN.
Looking at the risk factors
Risk factors of an osteoporotic fracture are divided into those that you can modify and those that you can’t. Nonmodifiable risk factors include the following:
 Age
Age
 European or Asian ancestry
European or Asian ancestry
 Family history of osteoporosis
Family history of osteoporosis
 Female
Female
 Loss of testosterone in men
Loss of testosterone in men
 Menopause
Menopause
 Previous fracture
Previous fracture
Modifiable risk factors include the following:
 Alcohol: Limit your drinking to ten glasses of wine or its equivalent per week if you’re male and five glasses per week if you’re female. Alcohol has direct effects on bone and also affects coordination leading to more falls.
Alcohol: Limit your drinking to ten glasses of wine or its equivalent per week if you’re male and five glasses per week if you’re female. Alcohol has direct effects on bone and also affects coordination leading to more falls.
 Anticoagulant use: If you have a condition that requires prevention of blood clotting, check with your doctor if you must continue anticoagulation long term.
Anticoagulant use: If you have a condition that requires prevention of blood clotting, check with your doctor if you must continue anticoagulation long term.
 Falls: You can prevent falls by
Falls: You can prevent falls by
• Avoiding sedating medications, including alcohol
• Avoiding walking on ice without help
• Removing household hazards such as loose carpeting, toys or pets underfoot
• Using bars in the bathtub
 High-protein diet: This one can be confusing. Most elderly don’t eat well and aren’t getting enough protein in the diet. It’s good for your bones if you correct this; however, some people think if a little is good, a lot is better. That’s simply not so. Too much protein may cause you to lose bone. Limit your protein intake to less than 50 grams a day.
High-protein diet: This one can be confusing. Most elderly don’t eat well and aren’t getting enough protein in the diet. It’s good for your bones if you correct this; however, some people think if a little is good, a lot is better. That’s simply not so. Too much protein may cause you to lose bone. Limit your protein intake to less than 50 grams a day.
 Inactivity: Do some weight-bearing exercise for 45 minutes at least three to four times weekly.
Inactivity: Do some weight-bearing exercise for 45 minutes at least three to four times weekly.
 Malnutrition: A diet that is insufficient in vitamin D and calcium should be corrected.
Malnutrition: A diet that is insufficient in vitamin D and calcium should be corrected.
 Glucocorticoids: If you must take glucocorticoids (for example, prednisone), use the lowest dose possible.
Glucocorticoids: If you must take glucocorticoids (for example, prednisone), use the lowest dose possible.
 Thiazolidinedione drugs used in diabetes: Use a different drug for diabetes if you have osteoporosis.
Thiazolidinedione drugs used in diabetes: Use a different drug for diabetes if you have osteoporosis.
 Thyroid excess: See your doctor to get your thyroid under control.
Thyroid excess: See your doctor to get your thyroid under control.
 Tobacco use: Don’t smoke.
Tobacco use: Don’t smoke.
 Vitamin D deficiency: Follow the recommendations in this book to get adequate amounts of vitamin D.
Vitamin D deficiency: Follow the recommendations in this book to get adequate amounts of vitamin D.
Diagnosing osteoporosis
Doctors diagnose osteoporosis by performing a bone densitometry test, which measures the amount of mineral per square centimeter of bone. The test typically takes about ten minutes to complete. Figure 4-4a shows dense, healthy bones, and Figure 4-4b shows bones weakened by osteoporosis.
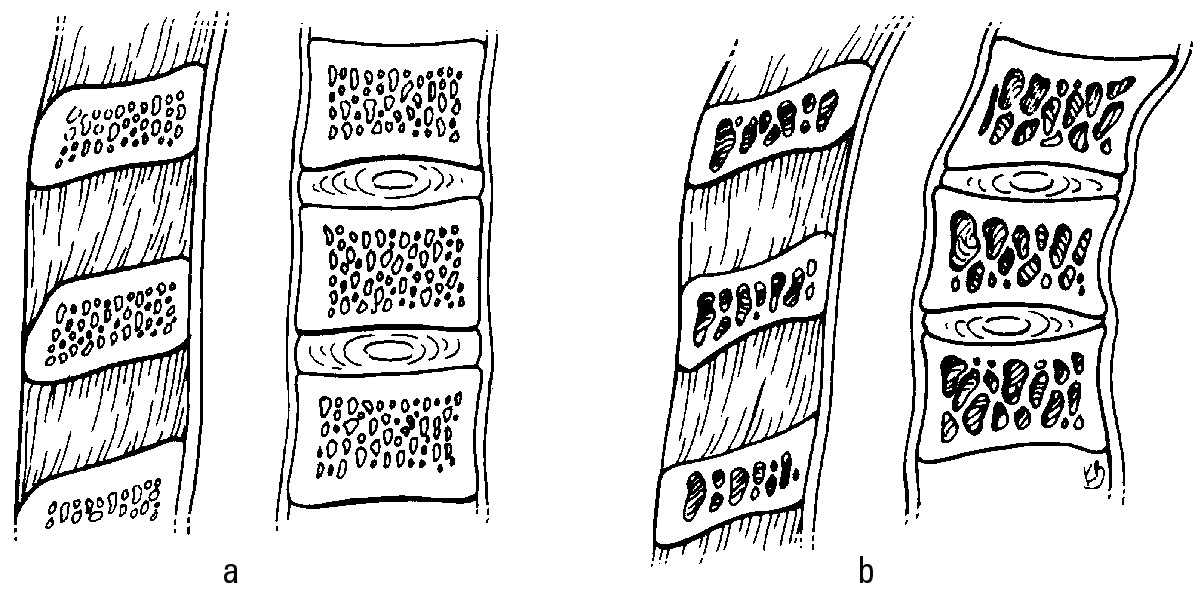
Figure 4-4: Healthy bones are denser than bones affected by osteoporosis.
The areas studied in a bone densitometry study are usually the lumbar spine and the upper part of the hip. The bone density correlates fairly well with the tendency of a bone to fracture. Measurements at the hip and spine can predict fractures at other sites.
Dual-energy X-ray absorptiometry (DXA) is the most common method for studying the density of your bones. In this study, you lie on a table; then two X-ray beams — one of high energy and one of low energy — are aimed at your bones. The amount of radiation that passes through the bone is measured for each beam. This amount is determined by the thickness of the bone. The bone density is measured by a formula using the difference between the two beams. This procedure is painless and safe; the amount of radiation is very small — about one-tenth the amount a patient receives during a routine chest X-ray.
The test is limited by differences in testing methods and technicians. Results are also affected by curvature of the spine, calcium in the abdominal aorta and blood vessels, arthritic changes in the spine, and multiple previous fractures. The test doesn’t identify the cause of low bone density.
 Women age 65 or older
Women age 65 or older
 Men age 70 or older
Men age 70 or older
 Women age 60 to 64 if they’re at increased risk — mainly low in weight, but also smokers and heavy drinkers (more than five drinks a week)
Women age 60 to 64 if they’re at increased risk — mainly low in weight, but also smokers and heavy drinkers (more than five drinks a week)
 Men between ages 50 and 70 who haven’t had sufficient testosterone
Men between ages 50 and 70 who haven’t had sufficient testosterone
 Anyone older than 50 who’s had a broken bone
Anyone older than 50 who’s had a broken bone
Osteoporosis is different from osteomalacia in several ways. First, in osteoporosis a person has normal blood levels of calcium, phosphorus, and vitamin D. The calcium content of the bone is normal; it’s just that there’s less bone present than normal (in contrast, in osteomalacia the bone contains less calcium than normal and that is why it is soft). Also, in osteoporosis, a person has both low bone density and starts losing the structure of the trabecular bone at the ends of bones and in the spine. (For more on osteomalacia, see the earlier section “Reckoning with Rickets and Osteomalacia.”) Osteoporosis also causes no pain unless fractures occur.
Preventing osteoporosis
You can prevent osteoporosis through lifestyle changes. Among the most important are the following:
 Exercise, which includes these components:
Exercise, which includes these components:
• Weight-bearing activities, such as walking, jogging, and dancing
• Resistance exercises, such as free weights and machines
• Balance exercises, such as tai chi and yoga
• Cycling on a stationary bike (for aerobic fitness without the risk of falling)
 Stop excessive drinking.
Stop excessive drinking.
 Stop smoking.
Stop smoking.
 Take vitamin D, calcium, and phosphorus supplements, if any are low in the blood. Chapters 3 and 14 offer recommendations on amounts.
Take vitamin D, calcium, and phosphorus supplements, if any are low in the blood. Chapters 3 and 14 offer recommendations on amounts.
Treating osteoporosis
When osteoporosis is in full swing, a person will need medical help in the form of drugs. Several drugs treat osteoporosis by slowing or stopping the bone loss. They don’t affect vitamin D. The current drugs of choice are the bisphosphonate class of drugs. These drugs work by binding to calcium in bone, thereby blocking the ability of osteoclasts to break down any more bone. They’re also taken up by osteoclasts. This destroys them so that they don’t break down any more bone.
The most popular bisphosphonates currently are
 Alendronate (Fosamax), taken once a day
Alendronate (Fosamax), taken once a day
 Risedronate (Actonel), taken once a week
Risedronate (Actonel), taken once a week
 Ibandronate (Boniva), taken once a month
Ibandronate (Boniva), taken once a month
 Zoledronic Acid (Reclast or Aclasta), taken intravenously once yearly
Zoledronic Acid (Reclast or Aclasta), taken intravenously once yearly
 Atrial fibrillation: The atria of the heart lose their regular motion and develop rapid disorganized movement.
Atrial fibrillation: The atria of the heart lose their regular motion and develop rapid disorganized movement.
 Inflammation of the stomach and erosion of the esophagus: The patient needs to be able to stand or sit upright for at least 30 minutes after taking a bisphosphonate. Because all bisphosphonates are poorly absorbed, the patient must avoid food, drink, and all medications for 30 minutes. (Some bisphosphonates can be administered intravenously, and this doesn’t happen with that route of delivery.)
Inflammation of the stomach and erosion of the esophagus: The patient needs to be able to stand or sit upright for at least 30 minutes after taking a bisphosphonate. Because all bisphosphonates are poorly absorbed, the patient must avoid food, drink, and all medications for 30 minutes. (Some bisphosphonates can be administered intravenously, and this doesn’t happen with that route of delivery.)
 Osteonecrosis of the jaw: In osteonecrosis, one of the jaw bones is exposed through the gums, and infection and pain occurs. This condition generally occurs after a dental extraction in patients treated with the intravenous forms (ibandronate and zoledronic acid).
Osteonecrosis of the jaw: In osteonecrosis, one of the jaw bones is exposed through the gums, and infection and pain occurs. This condition generally occurs after a dental extraction in patients treated with the intravenous forms (ibandronate and zoledronic acid).
 Severe pain: The pain occurs in bones, joints, or muscles.
Severe pain: The pain occurs in bones, joints, or muscles.
Physicians monitor the effect of the bisphosphonates by repeating the bone densitometry study every year or two. If the bone densitometry remains stable or improves, the patient may stop the bisphosphonates after five years. Doctors continue to monitor bone density.
Five other drugs are used to treat osteoporosis:
 Intermittent Parathyroid Hormone (Forteo) is one that probably surprises you because we already told you that parathyroid hormone breaks down bone. It turns out this hormone can both increase and decrease bone mass, depending how you use it. In the body, when serum calcium falls, parathyroid hormone is increased, and its level stays up for a long time. When used as a treatment for osteoporosis, parathyroid hormone is given in small daily doses and the serum level of this hormone is increased for just a short time. This actually increases osteoblast activity and builds new bone.
Intermittent Parathyroid Hormone (Forteo) is one that probably surprises you because we already told you that parathyroid hormone breaks down bone. It turns out this hormone can both increase and decrease bone mass, depending how you use it. In the body, when serum calcium falls, parathyroid hormone is increased, and its level stays up for a long time. When used as a treatment for osteoporosis, parathyroid hormone is given in small daily doses and the serum level of this hormone is increased for just a short time. This actually increases osteoblast activity and builds new bone.
 Denosumab (Prolia) is an antibody to a chemical signal that tells osteoclasts to tear down bone. Given every six months as a subcutaneous injection, it is more effective than bisphosphonates in turning off bone resorption and it is very effective at preventing fractures.
Denosumab (Prolia) is an antibody to a chemical signal that tells osteoclasts to tear down bone. Given every six months as a subcutaneous injection, it is more effective than bisphosphonates in turning off bone resorption and it is very effective at preventing fractures.
 Strontium ranelate (Protelos) is an element similar to calcium. Binding strontiuim to ranelate increases its absorption in the intestine. Strontium ranelate reduces bone breakdown and also seems to stimulate bone formation modestly. It prevents spine and hip fractures. It is not approved in the United States or Canada but has become the most popular osteoporosis medication in Europe. Beware that strontium citrate, available in health food stores in North America, is poorly absorbed and has not been shown to benefit the skeleton.
Strontium ranelate (Protelos) is an element similar to calcium. Binding strontiuim to ranelate increases its absorption in the intestine. Strontium ranelate reduces bone breakdown and also seems to stimulate bone formation modestly. It prevents spine and hip fractures. It is not approved in the United States or Canada but has become the most popular osteoporosis medication in Europe. Beware that strontium citrate, available in health food stores in North America, is poorly absorbed and has not been shown to benefit the skeleton.
 Calcitonin is a hormone normally produced in the thyroid gland that suppresses osteoclast activity, so the bone isn’t reabsorbed.
Calcitonin is a hormone normally produced in the thyroid gland that suppresses osteoclast activity, so the bone isn’t reabsorbed.
 Raloxifene is a drug similar to the female hormone estrogen that was designed to give the good effects of estrogen on bone without the bad effects on other organs like the heart or the uterus. It’s one of a class of drugs called selective estrogen receptor modulators, or SERMs. SERMs and estrogen stimulate osteoblast activity to build bone or suppress osteoclast activity that reabsorbs bone. Raloxifene is especially protective of the vertebral spine, reducing the risk of fractures by 55 percent.
Raloxifene is a drug similar to the female hormone estrogen that was designed to give the good effects of estrogen on bone without the bad effects on other organs like the heart or the uterus. It’s one of a class of drugs called selective estrogen receptor modulators, or SERMs. SERMs and estrogen stimulate osteoblast activity to build bone or suppress osteoclast activity that reabsorbs bone. Raloxifene is especially protective of the vertebral spine, reducing the risk of fractures by 55 percent.
Examining the connection between vitamin D and bone health in seniors
In November 2010 an expert committee gathered together by the Institute of Medicine of the U.S. National Academy of Science released its new recommendations for vitamin D intake (see Chapter 2). Their recommendations for older people are similar to ones released in April 2010 by the International Osteoporosis Foundation (IOF). Both of these recommendations are based on a type of research called randomized clinical trials. In these studies scientists follow two similar groups — one that gets a treatment (like vitamin D) and one that gets a placebo or a pill that’s not supposed to do anything. Neither the people in the study nor the scientists know who is getting what treatment until the end of the study (that’s called a “double blind” study). For the scientists to say that a treatment works, it has to help the people on the treatment significantly more than any effect seen in the placebo group.
The IOF and the Institute of Medicine committee agreed on several points:
 Vitamin D acts on muscle tissue and improves grip strength and muscle mass.
Vitamin D acts on muscle tissue and improves grip strength and muscle mass.
 Supplementing with vitamin D may improve lower extremity performance and reduce the risk of falling.
Supplementing with vitamin D may improve lower extremity performance and reduce the risk of falling.
 Supplementing with a dose of at least 600 IU daily was needed to see a detectable effect on falls.
Supplementing with a dose of at least 600 IU daily was needed to see a detectable effect on falls.
 Vitamin D affects fracture risk through its effect on bone metabolism and risk of falling.
Vitamin D affects fracture risk through its effect on bone metabolism and risk of falling.
 Vitamin D reduces rates of bone loss in older women.
Vitamin D reduces rates of bone loss in older women.
 Supplementing with a dose of at least 600 IU daily was needed to see an effect on nonvertebral and hip fractures.
Supplementing with a dose of at least 600 IU daily was needed to see an effect on nonvertebral and hip fractures.
Making the case for more vitamin D
Based on the results of the randomized clinical trials, both the IOF and the Institute of Medicine committee recommended that people take more vitamin D. The IOF argued that women need 800 to 1,000 IU of vitamin D daily whereas the Institute of Medicine committee thought that 700 to 800 IU was enough.
The two groups also pointed out that the amount of dietary vitamin D a person needs varies depending on the starting level of 25-hydroxyvitamin D, how much body fat a person has, the amount of sun exposure, and other factors.
The Institute of Medicine committee set their requirement with the assumption that someone gets no vitamin D from sunlight. It’s also critical to realize that these requirements are set for normal, healthy people not people with specific diseases. However, the Institute of Medicine report did make a point to explain that the vitamin D dose may need to be adjusted upward when people have trouble absorbing fat or for people who are obese. The IOF recommended that physicians may need to adjust vitamin D intake upward in some special groups (to as high as 2,000 IU each day). But someone who has fat malabsorption may need even larger doses of vitamin D to achieve target 25-hydroxyvitamin D levels.
The IOF also noted that because uncertainty exists about whether vitamin D3 is more effective than vitamin D2 at raising the 25(OH) vitamin D, physicians should use vitamin D3 when available.
There was a big disagreement between the two groups on the level of serum 25-hydroxyvitamin D that people should reach to help their bones and prevent osteoporotic fractures. The IOF felt that 30 ng/ml [75 nmol/L] is the appropriate target level for serum 25-hydroxyvitamin D, but the Institute of Medicine committee showed that this estimate was based on a flawed study. As a result, the Institute of Medicine committee recommended 20 ng/ml [50 nmol/L] as the target level.
How calcium factors in
Calcium isn’t as well absorbed from the intestine in older women compared to young women. Also, the daily intake of calcium by every age group of American women is less than the daily recommended intakes, sometimes by as much as 500 mg a day. This means older women are doubly cursed — they don’t get enough calcium in their diet, and they don’t absorb the calcium they do get very well.
Many elderly women don’t like dairy products because they develop lactose intolerance and dairy upsets their stomach. For that reason, doctors recommend that most women take a daily supplement of 1,000 mg to reach their recommended levels.
Helping Your Teeth Grow
Teeth aren’t exactly bones, but they’re made up of similar tissues and are subject to the same problems bones may have. Because of this, rickets and osteomalacia also can affect teeth. In this section, I discuss the normal development of teeth and the effects of these conditions on them.
Exploring the normal development of teeth
Humans develop two different sets of teeth. The baby, or primary, teeth begin to erupt from the gums at six months of age, which any parent knows is a painful time called teething. Primary teeth begin to develop between the sixth and eighth weeks of pregnancy. Permanent teeth form in the twentieth week of pregnancy. These times are critical, and the teeth may not develop if they don’t start by then. If a mom’s vitamin D and calcium levels are deficient when this development is taking place, the teeth don’t form normally.
A tooth consists of a top part called a crown, made of enamel. Enamel is made up of calcium phosphate and is the hardest substance in the body. Under the crown is supporting dentin, which is mineralized tissue that isn’t as hard as the enamel. Within the dentin is the pulp of the tooth, which contains the nerves and blood vessels for the tooth.
The tooth continues down into its bony support of the jaw and skull as one or more roots, which are covered by cementum. Cementum is another mineralized tissue that is softer than dentin or enamel. Cementum permits the tooth to attach strongly to the bone.
Where the crown of the tooth meets its supporting bone, it’s surrounded by soft tissue called gingiva, or gums. Figure 4-5 shows the various parts of a tooth.
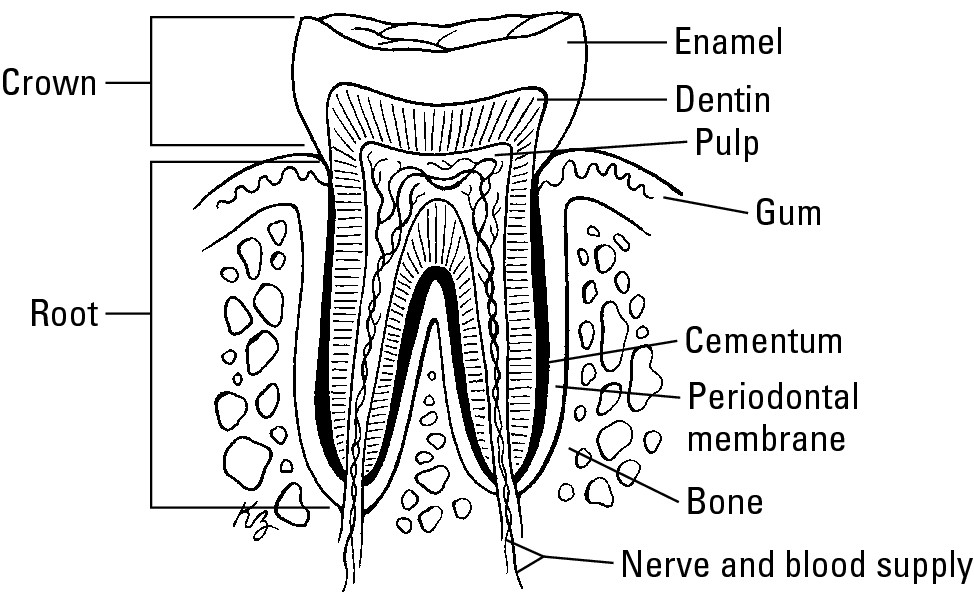
Figure 4-5: Parts of a tooth.
Knowing how rickets affects teeth
Rickets can have a negative effect at every stage of the development of teeth. The primary effects of rickets include the following:
 Delayed formation: The baby teeth may not erupt until after one year. When they erupt, they may be smaller than normal.
Delayed formation: The baby teeth may not erupt until after one year. When they erupt, they may be smaller than normal.
 Periodontal disease: Periodontal disease can affect many different parts of the tooth, the bone, the cementum, or the gingiva. All of these weaken the anchoring of the teeth into bone. In the absence of sufficient vitamin D, the bone that forms in the jaw or skull isn’t sufficiently mineralized. Periodontal disease is also commonly caused by infection of the gums. When a gum infection occurs and the gingiva become inflamed, normal chewing or pressure on the gums makes them bleed easily. This condition is called gingivitis.
Periodontal disease: Periodontal disease can affect many different parts of the tooth, the bone, the cementum, or the gingiva. All of these weaken the anchoring of the teeth into bone. In the absence of sufficient vitamin D, the bone that forms in the jaw or skull isn’t sufficiently mineralized. Periodontal disease is also commonly caused by infection of the gums. When a gum infection occurs and the gingiva become inflamed, normal chewing or pressure on the gums makes them bleed easily. This condition is called gingivitis.
Calcitriol helps regulate the immune system and protect against inflammation (see Chapter 5) so some have suggested that low vitamin D status increases periodontal disease by increasing gingivitis. Regardless of the cause, when the teeth become loose in the mouth they may fall out.
 Dental caries: Dental caries, or cavities, are holes in the enamel of the tooth and can also result from inadequate vitamin D status. Because the teeth don’t mineralize sufficiently in rickets caused by low vitamin D status, this may increase a person’s chances of getting cavities. In the absence of vitamin D, infection is established on the tooth, leading to further loss of enamel and cavitation (holes in the teeth).
Dental caries: Dental caries, or cavities, are holes in the enamel of the tooth and can also result from inadequate vitamin D status. Because the teeth don’t mineralize sufficiently in rickets caused by low vitamin D status, this may increase a person’s chances of getting cavities. In the absence of vitamin D, infection is established on the tooth, leading to further loss of enamel and cavitation (holes in the teeth).
Symptoms of dental caries include the following:
• Bad breath
• Chills
• Fever
• Foul taste
• Increasing infection
• Pain
• Tooth loss
The caries can involve the enamel, the dentin, or the cementum. Pain occurs when the cavity reaches the dentin, which is connected to the nerves in the root of the tooth.
Osteomalacia can result in all these abnormalities as well. The teeth are painful, deformed, and subject to increased cavities and periodontal disease. They may be lost early. (For more on osteomalacia, see the section “Reckoning with Rickets and Osteomalacia” earlier in this chapter.)


