Chapter 5
Protecting the Immune System
In This Chapter
 Taking a look at the immune system
Taking a look at the immune system
 Exploring the role of vitamin D
Exploring the role of vitamin D
 Battling infections
Battling infections
 Looking at multiple sclerosis, rheumatoid arthritis, and lupus
Looking at multiple sclerosis, rheumatoid arthritis, and lupus
The body’s immune system protects against foreign invaders such as bacteria and viruses. Unfortunately, that same system sometimes mistakes native body cells for invaders. When that happens, the body reacts against them and kills normal healthy cells your body needs. This is called autoimmunity, a reaction that causes diseases such as type 1 diabetes mellitus, hypothyroidism and hyperthyroidism, multiple sclerosis, rheumatoid arthritis, and Crohn’s disease.
Evidence that vitamin D may be important for a healthy immune system has been accumulating since 1982, when scientists first discovered that human white blood cells contained receptors for calcitriol (the active form of vitamin D). White blood cells are circu-lating cells that are critical for our response against the microbes that cause disease. Soon afterward, scientists discovered that specific types of white blood cells could turn 25-hydroxyvitamin D into calcitriol. Still later, researchers showed that calcitriol caused other white blood cells to make a protein that kills invasive organisms. This all shows that calcitriol is needed for your immune system but doesn’t answer the question of how much vitamin D you need in your body to get this protection.
This chapter explains how the normal immune system functions and how it can go awry without active vitamin D.
Describing the Immune System
The immune system is made up of many different tissues and processes that protect the body against invaders and kill them when they get in. There are multiple lines of protection that make up the immune system:
 The skin, lungs, sinuses, and intestine are physical barriers to invasion.
The skin, lungs, sinuses, and intestine are physical barriers to invasion.
 Cells that come to the site of damage or infection engulf the invaders and digest them (called phagocytes).
Cells that come to the site of damage or infection engulf the invaders and digest them (called phagocytes).
 Cells that are recruited to the site of infection by phagocytes and produce chemicals that work against the invaders.
Cells that are recruited to the site of infection by phagocytes and produce chemicals that work against the invaders.
 Cells that retain a memory of past invaders so that the body can mount an attack in the future (called acquired immunity that is the basis for why vaccines work).
Cells that retain a memory of past invaders so that the body can mount an attack in the future (called acquired immunity that is the basis for why vaccines work).
 Organs like the liver, spleen, and lymph glands, which sweep up invaders and destroy them.
Organs like the liver, spleen, and lymph glands, which sweep up invaders and destroy them.
In the following sections, I describe the two divisions of the immune system and the cells that help keep you healthy.
Separating the innate from the adaptive immune system
The immune system is divided into the innate immune system and the adaptive immune system. All of the cells that make up these two parts of the immune system are broadly called white blood cells; however, there are many different types of white blood cells, and each of them has a specific function.
The innate immune system is made up of white blood cells that attack organisms and foreign materials that get past the body’s barriers. Because the innate immune system hasn’t previously encountered the invader, it doesn’t have specific weapons to destroy it; instead, it uses a variety of nonspecific tools:
 Phagocytosis: This is the process whereby cells engulf and kill invaders by “eating” them.
Phagocytosis: This is the process whereby cells engulf and kill invaders by “eating” them.
 Inflammation: White blood cells are attracted to the invaders and release chemicals called cytokines in an attempt to destroy them. Some of these cytokines are toxic to the invader, some cause your body to have a fever to make the body a less pleasant place for invaders, and some send messages to other types of white blood cells to come and join the attack. Altogether this causes the typical redness and swelling at the site of an infection.
Inflammation: White blood cells are attracted to the invaders and release chemicals called cytokines in an attempt to destroy them. Some of these cytokines are toxic to the invader, some cause your body to have a fever to make the body a less pleasant place for invaders, and some send messages to other types of white blood cells to come and join the attack. Altogether this causes the typical redness and swelling at the site of an infection.
The adaptive immune system is the system that has the ability to remember invaders from the past so that it can start a specific response to an invader the next time it enters the body. Its tools include the following:
 B and T lymphocytes (described in the next section)
B and T lymphocytes (described in the next section)
 Antibodies, the proteins that B lymphocytes produce that circulate looking for a specific invader or protein from an invader
Antibodies, the proteins that B lymphocytes produce that circulate looking for a specific invader or protein from an invader
Calling on B and T cells for protection
B and T cells are white blood cells that play an important role in immunity. Both types originate in the bone marrow, but B cells mature in the spleen and T cells mature in the thymus. Phagocytes, B cells, and T cells all work together to protect your body from invaders.
B cells are part of the system that uses proteins to destroy the invader. B cells have the ability to recognize the proteins on the invader’s surface. The B cell then makes a new protein that recognizes the invader protein — the B cell protein is called an antibody. The protein on the invader is called an antigen. When an antibody binds to an antigen, the two proteins enter the B cell and the antigen is broken down to pieces of proteins called peptides. These peptides are then brought back to the surface of the B cell. Mature T cells attach to the antigen peptide fragments on the surface and cause the B cell to divide and produce millions of copies of the antibody that recognizes the foreign antigen. The antibodies circulate in the blood, attaching to the foreign invaders and marking them for destruction in the liver or spleen.
There are many different types of T cells:
 Helper T cells are the T cells that help manage the immune response by regulating what B cells and phagocytes do. For example, as described earlier in this chapter, they stimulate the B cell to make antibodies that are needed to clear invaders from the body. Helper T cells can also bind to the surface of phagocytes. This causes the helper T cell to produce chemicals that recruit more phagocytes and more T cells. There are many different types of helper T cells; it’s the balance among all the various types of helper T cells that defines how the immune system fights a specific infection.
Helper T cells are the T cells that help manage the immune response by regulating what B cells and phagocytes do. For example, as described earlier in this chapter, they stimulate the B cell to make antibodies that are needed to clear invaders from the body. Helper T cells can also bind to the surface of phagocytes. This causes the helper T cell to produce chemicals that recruit more phagocytes and more T cells. There are many different types of helper T cells; it’s the balance among all the various types of helper T cells that defines how the immune system fights a specific infection.
 The natural killer T cell kills cells that are infected with viruses or that are damaged. Each natural killer T cell looks for a specific viral antigen sitting on a cell that has been infected. When it finds that antigen, the natural killer T cell releases chemicals that kill the infected cell.
The natural killer T cell kills cells that are infected with viruses or that are damaged. Each natural killer T cell looks for a specific viral antigen sitting on a cell that has been infected. When it finds that antigen, the natural killer T cell releases chemicals that kill the infected cell.
Consider the example of influenza to illustrate the function of these B and T cells. When an influenza virus enters the body, usually by being inhaled, B cells produce antibodies that latch on to the influenza virus. The B cells remember that influenza virus, so a future attack by that same virus quickly results in an outpouring of antibodies to keep the virus from causing disease. When the virus is covered by antibodies, certain types of T cells come along and destroy the antibody-covered virus.
Immunity can be passive or active. When a baby is in the mother’s uterus, the mother passes her antibodies through the placenta (the connection between mother and child) so that the baby is born with the ability to fight some infections even before its own immune system develops. This is called passive immunity. During breastfeeding, the mother sends antibodies into the baby’s stomach to protect against invaders there (again, passive immunity). Within several months of birth, the baby can make his or her own antibodies (active immunity).
Realizing the Role of Vitamin D
There has been a lot of interesting research that points to an important role for calcitriol in the immune system. Most of this research has been done in cultured cells (cells isolated from the body and grown in special solutions of nutrients) and in animals with either severe vitamin D deficiency or whose genes have been altered to “knock out” proteins that control vitamin D metabolism or active vitamin D action. These types of studies are essential proof of principle that vitamin D is important for the immune system. On top of this, there are a lot of studies that draw associations between either estimated UV light exposure (for example, season or latitude) or serum 25-hydroxyitamin D and certain types of infections or conditions.
Because of these studies scientists are pretty sure that vitamin D (or, more specifically, calcitriol) is important for strengthening the immune system. What we don’t know yet is how much vitamin D you need so there is enough calcitriol to maximize the way your immune system works. Research to figure that out is ongoing.
Certain B cells and T cells have vitamin D receptors and can respond to calcitriol whereas some phagocytes can convert 25-hydroxyvitamin D into calcitriol. This suggests that phagocytes may communicate with T and B cells through calcitriol.
Research studies on the cells of the immune system show that when calcitriol is present it blocks the features of the adaptive immune system that would lead to autoimmunity. Animal studies show that when calcitriol is absent, the cells of the immune system are more likely to attack the healthy cells of the body (autoimmunity). It’s important to remember that lack of vitamin D isn’t the only or even the primary cause for autoimmunity — it’s just not good for the immune system when vitamin D is low. Unfortunately, it’s not clear yet how much vitamin D you need in your body to lessen the impact of autoimmunity on health. However, later in this chapter I discuss specific examples where researchers think vitamin D can help prevent various infectious diseases and specific immune diseases.
Vitamin D, as calcitriol, influences the immune system in two ways:
 Calcitriol avoids triggering and arming the T cells during autoimmunity. T cells play a major role in autoimmunity. Calcitriol helps diminish that role and blocks the increased production of the specific helper T cells needed for autoimmunity. Blocking the production of those cells decreases the ability of T cells to recognize the native protein as foreign, so fewer killer T cells are produced. In other words, the presence of adequate levels of vitamin D and calcitriol keeps the T cells from attacking the body’s own tissues.
Calcitriol avoids triggering and arming the T cells during autoimmunity. T cells play a major role in autoimmunity. Calcitriol helps diminish that role and blocks the increased production of the specific helper T cells needed for autoimmunity. Blocking the production of those cells decreases the ability of T cells to recognize the native protein as foreign, so fewer killer T cells are produced. In other words, the presence of adequate levels of vitamin D and calcitriol keeps the T cells from attacking the body’s own tissues.
 Calcitriol blocks chemicals that kill native tissue. As it decreases the number of T cells, calcitriol also diminishes the role of B cells in producing chemicals to destroy native tissue. The antibody response to the body’s own tissue is decreased and the reaction is blocked. For example, diminished destruction of the beta cells of the pancreas, the cause of type 1 diabetes, are proposed to result when adequate levels of vitamin D and calcitriol are present.
Calcitriol blocks chemicals that kill native tissue. As it decreases the number of T cells, calcitriol also diminishes the role of B cells in producing chemicals to destroy native tissue. The antibody response to the body’s own tissue is decreased and the reaction is blocked. For example, diminished destruction of the beta cells of the pancreas, the cause of type 1 diabetes, are proposed to result when adequate levels of vitamin D and calcitriol are present.
Boosting the Immune System to Fight Infections
Infectious diseases are diseases caused by viruses, bacteria, and other tiny organisms that enter the body through the lungs, the skin, or the intestines.
Books have been written about the positive effect of sunlight on infectious diseases. In fact, an early Nobel Prize in medicine was given to Neils Ryberg Finsen for his work on how sunlight could be used in the treatment of tuberculosis of the skin. A prime example of sunlight in medicine is presented in the book The Magic Mountain (Everyman’s Library), by Thomas Mann. It’s a story about a visit to a sanitarium high in the Alps in Davos, Switzerland where people went to seek a cure for tuberculosis in the decade before World War I. Although they weren’t exactly sure what it was doing, doctors and patients felt that the sun had healing properties. Today we believe that the increased vitamin D produced by the sun at higher altitudes through conversion into calcitriol, could be the reason for the sanitarium’s success.
In the following sections, I explain how vitamin D may help your body fight off nasty infections such as the flu and tuberculosis.
Healing tuberculosis
Some scientists think that vitamin D could play a major role in managing tuberculosis, a disease of the lungs. Tuberculosis (TB) is a common infection caused by the bacteria Mycobacterium tuberculosis in humans. About one-third of the world’s population has been infected with TB, but most infections don’t cause disease; they just remain quietly in the body.
Vaccinations may prevent tuberculosis, and TB is usually treated with antibiotics. This treatment approach has been effective, but tuberculosis continues to be a major problem for two reasons. First, antibiotic-resistant strains of the organism have developed and are difficult to treat. Second, immune diseases such as HIV/AIDS allow the disease-causing organism to spread throughout the body.
In 75 percent of patients TB starts in the lungs. Other areas that are affected after spreading from the lungs:
 The pleura, the tissue that surrounds the lungs
The pleura, the tissue that surrounds the lungs
 The central nervous system, with tuberculous meningitis
The central nervous system, with tuberculous meningitis
 The neck, with involvement of lymph nodes leading to a condition called scrofula
The neck, with involvement of lymph nodes leading to a condition called scrofula
 The genitourinary system, with involvement of the kidneys
The genitourinary system, with involvement of the kidneys
 The bones and joints, leading to Pott’s disease of the spine
The bones and joints, leading to Pott’s disease of the spine
Signs and symptoms of TB
Pulmonary tuberculosis involves the following symptoms:
 Chest pain
Chest pain
 Cough, often producing blood
Cough, often producing blood
 Fatigue
Fatigue
 Fever
Fever
 Night sweats
Night sweats
 Weight loss
Weight loss
Doctors can identify the disease by taking a sputum (stuff you cough up from your lungs) sample and examining it under a microscope. The presence of Mycobacterium tuberculosis, an organism that is bright-red and elongated, confirms the diagnosis.
The role of vitamin D and calcitriol in TB
The first suggestion that vitamin D might be beneficial for TB was from anecdotal reports from doctors and their patients in the days before antibiotics were available as a treatment. They swore that both sunlight and cod liver oil were cures for the disease. Other people noticed that TB rates were higher in African Americans (45 percent of U.S.-born citizens who contract TB are black). What do these things have in common? Vitamin D! Unfortunately, these types of findings aren’t strong enough proof to stop doctors from using antibiotics and start using vitamin D supplements to treat TB.
Interestingly, people who have TB are more likely to have low serum 25-hydroxyvitamin D levels than healthy people. The problem is we don’t know if this is the cause of the TB or an effect that results from the infection.
Strong proof of principle that calcitriol protects against TB comes from cell studies.
When tuberculosis organisms enter the body, they stimulate the innate immune system to trigger an antituberculosis response in white blood cells from the innate immune system called monocytes. In the presence of calcitriol, these monocytes produce several specific antimicrobial peptides that kill viruses, bacteria, and fungi — and also modify the way other cells of the innate and adaptive immune system work. These antimicrobial peptides are like broad spectrum antibiotics. Cathelicidin is one that kills the tuberculosis organisms after they’ve been engulfed by the monocytes. Defensin is another that pokes holes in the invaders, allowing entry of compounds that kill them. Both cathelocidin and defensin levels are increased in monocytes treated with active vitamin D, and these block the TB infection.
When they’re activated by the TB microbe, the monocytes also increase the numbers of receptors for calcitriol and they convert 25-hydroxyvitamin D into calcitriol. This all suggests that if you have an adequate vitamin D status, your body can battle tuberculosis much more effectively.
Fending off flu and other viruses
New cell-based research from the last couple of years shows that calcitriol enhances innate immunity by prompting cells to produce a large numbers of antimicrobial peptides that are like broad spectrum antibiotics. These are substances that kill viruses, bacteria, and fungi — and they also modify the way other cells of the innate and adaptive immune system work. This may explain how calcitriol could protect you against the influenza virus.
So what’s the direct evidence that more vitamin D is good for preventing infections like the flu or other upper respiratory tract (URT) infections? The first line of evidence is the same as for TB — monocytes treated with calcitriol make antimicrobial peptides that kill viruses. There are even a few clinical studies that support the idea that a supplement with vitamin D would reduce the number of URT infections or flu. The problem is that those studies aren’t big or weren’t done quite right, and none of them can define a vitamin D level for protection. For example, a small study out of Japan in 2010 was widely covered in the media for its claim that vitamin D use in schoolchildren reduced the cases of influenza A. One problem with that study is that almost 25 percent of subjects dropped out; whenever the dropouts exceed 5 to 10 percent, a study’s results become skewed and questionable. But more importantly, the number of cases of influenza B increased by almost the same amount that the cases of influenza A decreased. So the study actually showed no net change in influenza cases, and it was too small of a study to conclude anything with certainty. So, even though it looks like vitamin D may be useful for stopping infections, we need more proof for this relationship as well as more information about how much vitamin D is required to prevent the flu.
Examining Autoimmune Diseases
There’s some promising but inconsistent evidence that the farther you live from the equator, the greater your chance to develop an autoimmune disease (in which the body attacks itself). These observations have led to major new investigations of the role of the sun and its product, vitamin D, in protecting against these diseases.
In this section, I describe some of the better-established connections between vitamin D and autoimmune diseases. (For more on how vitamin D affects autoimmune responses, see the section “Describing the Immune System,” earlier in this chapter.)
Autoimmune diseases occur for a number of reasons with genetics (heredity) and ethnicity playing a large role in determining whether you’re at risk for them or not. Other factors such as stress, infections, environment, and possibly low vitamin D status may act as triggers for the autoimmune attack to begin in a susceptible person. When it happens it’s because the adaptive immune system has gone awry, so it’s the role of calcitriol on T and B cells that’s important here. Remember, cell studies show that calcitriol suppresses the adaptive immune system so that it doesn’t kill cells that are part of your body.
Multiple sclerosis
Multiple sclerosis (MS) is an autoimmune disease that attacks a person’s own nervous system. In MS, the myelin sheaths that surround the nerves in the brain and spinal cord are damaged. Just like the wires in your house can’t transmit properly if they’ve lost their surrounding insulation, so too the nerves can’t conduct an electrical signal without their myelin sheaths, and the function of that nerve is lost. The body tries to restore the myelin but can’t completely do it. The resultant signs and symptoms depend on which areas are most damaged.
When the nerve tissue of a person affected by MS is examined, damage by T cells, a major player in the adaptive immune system, is evident. Ordinarily, T cells don’t get through the blood-brain barrier to enter the brain, but they do in MS. T cells treat the myelin like a foreign protein, leading to signals that bring other cells into the brain and also cause the production of cytokines that kill cells and cause inflammation.
The disease usually begins in young adults and occurs more in females than males. MS comes and goes in multiple cycles called relapses and remissions. Sometimes after a relapse there aren’t any signs of the disease. Unfortunately, after some relapses, abnormalities remain. These abnormalities continue to accumulate with additional relapse/remission cycles so that the severity of MS gets worse over time.
Signs and symptoms of MS
Signs and symptoms of multiple sclerosis vary widely and include any or all of the following, all of which may be intermittent:
 Acute or chronic pain
Acute or chronic pain
 Difficulty with speech and vision
Difficulty with speech and vision
 Fatigue
Fatigue
 Loss of balance
Loss of balance
 Loss of bladder and/or bowel control
Loss of bladder and/or bowel control
 Loss of sensation
Loss of sensation
 Muscle spasms
Muscle spasms
 Weakness
Weakness
Multiple sclerosis is diagnosed in the following way:
 MRI scan of the brain and spine show areas consistent with lost myelin covering the nerves.
MRI scan of the brain and spine show areas consistent with lost myelin covering the nerves.
 Cerebrospinal fluid obtained by inserting a needle into the lumbar spine shows chronic inflammation with white blood cells and certain types of proteins.
Cerebrospinal fluid obtained by inserting a needle into the lumbar spine shows chronic inflammation with white blood cells and certain types of proteins.
 When certain nerves are stimulated, they respond more slowly than normal.
When certain nerves are stimulated, they respond more slowly than normal.
Relapses are unpredictable but usually happen no more than once or twice a year. They may be brought on by viral infections or stress. The lifespan of a person with MS is five to ten years less than someone who isn’t affected.
Doctors use a variety of drugs to treat MS, but none have been completely successful. (For more information on MS, check out Multiple Sclerosis For Dummies, by Rosalind Kalb, PhD.)
The role of vitamin D in MS
There are a number of different lines of indirect evidence that suggest higher intakes of vitamin D or circulating 25-hydroxyvitamin D levels may delay the onset of MS or improve the disease course. Consider some of the evidence:
 Many MS patients have low circulating levels of 25-hydroxyvitamin D, especially during relapses. The problem with this observation is that many people develop lower vitamin D levels during times of illness because they are indoors and not eating well.
Many MS patients have low circulating levels of 25-hydroxyvitamin D, especially during relapses. The problem with this observation is that many people develop lower vitamin D levels during times of illness because they are indoors and not eating well.
 Low serum 25-hydroxyvitamin D levels are associated with the relapse rate of MS. Consistent with this, one clinical study found that increasing vitamin D intake might reduce the relapse rate, but there weren’t enough people studied to be certain.
Low serum 25-hydroxyvitamin D levels are associated with the relapse rate of MS. Consistent with this, one clinical study found that increasing vitamin D intake might reduce the relapse rate, but there weren’t enough people studied to be certain.
 Higher serum 25-hydroxyvitamin D levels have been associated with improved T cell function in MS patients.
Higher serum 25-hydroxyvitamin D levels have been associated with improved T cell function in MS patients.
 There is a widely held belief that as latitude moves away from the equator, the population experiences a progressive increase in the incidence of MS. In fact, people who have lived in the tropics up to age 15 rarely develop the disease, even if they later move to temperate areas. However, a careful review of the evidence found that there is an effect of latitude only in Australia and New Zealand, but not in North America or Europe.
There is a widely held belief that as latitude moves away from the equator, the population experiences a progressive increase in the incidence of MS. In fact, people who have lived in the tropics up to age 15 rarely develop the disease, even if they later move to temperate areas. However, a careful review of the evidence found that there is an effect of latitude only in Australia and New Zealand, but not in North America or Europe.
 In Sweden, more people affected with MS were born during the months when the mother was low in vitamin D than during the months when the mother had adequate vitamin D. This is interesting because it suggests low vitamin D status during pregnancy might program a person to have a higher risk of MS as an adult.
In Sweden, more people affected with MS were born during the months when the mother was low in vitamin D than during the months when the mother had adequate vitamin D. This is interesting because it suggests low vitamin D status during pregnancy might program a person to have a higher risk of MS as an adult.
 Calcitriol and drugs designed to look like it inhibit experimental autoimmune encephalitis, an animal model of MS.
Calcitriol and drugs designed to look like it inhibit experimental autoimmune encephalitis, an animal model of MS.
These facts suggest that lack of vitamin D may be playing a role in the onset and progression of MS; however, no one has yet shown that vitamin D supplements prevent the development of MS, slow the rate of relapse of the MS, or reduce the symptoms associated with an outbreak of the disease. Ongoing clinical trials should give the final answer about this relationship and also determine the level of vitamin D intake or serum 25-hydroxyvitamin D needed to prevent or lessen the impact of MS.
Rheumatoid arthritis
Rheumatoid arthritis (RA) is an autoimmune disease that affects the synovial joints between bones. The synovial joints are surrounded by a joint capsule. The inner lining of the joint capsule is made of tissue called synovium, which secretes synovial fluid into the synovial cavity to provide smooth movement of the joint. Figure 5-1 shows a typical synovial joint.
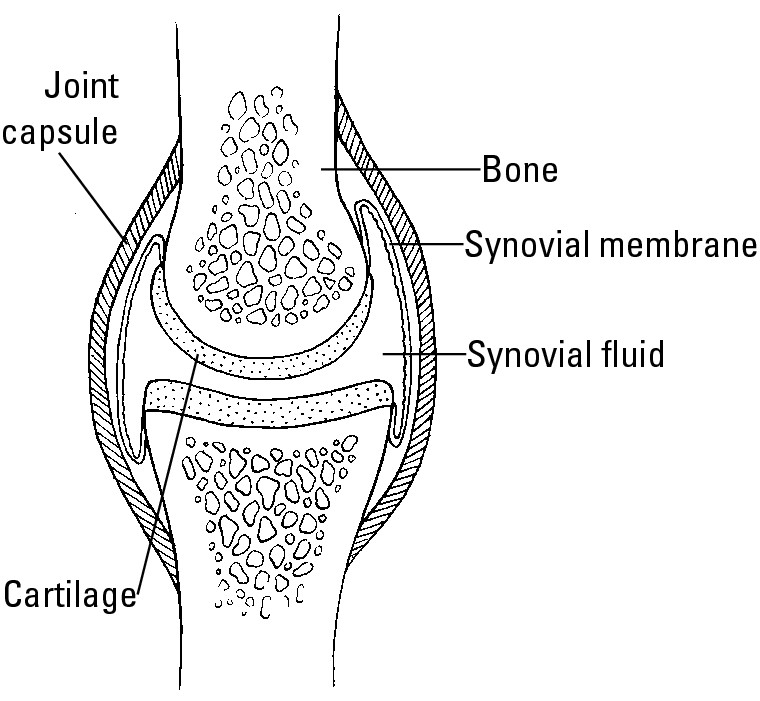
Figure 5-1: A healthy synovial joint.
RA can affect the main synovial joints of the body:
 Elbow joints
Elbow joints
 Finger and toe joints
Finger and toe joints
 Hip joints
Hip joints
 Knee joints
Knee joints
 Shoulder joints
Shoulder joints
 Wrist joints
Wrist joints
Like all autoimmune diseases, RA is caused by the adaptive immune system. Because calcitriol modulates the adaptive immune system, intake of vitamin D may modulate RA.
In RA, the immune system attacks the synovial tissue, which stops producing the synovial fluid. Without synovial fluid the joints don’t move smoothly. It’s like removing the oil from the engine of a car — you get a lot of friction without the oil. In RA, the joints heat up, swell, and become tender. Over time they also become stiff and don’t move well. As the disease worsens, the joints lose their motion and become deformed.
Figure 5-2 shows a synovial joint affected by rheumatoid arthritis.
RA usually progresses to loss of joint function and movement after ten years. RA also reduces a person’s lifespan by about ten years.
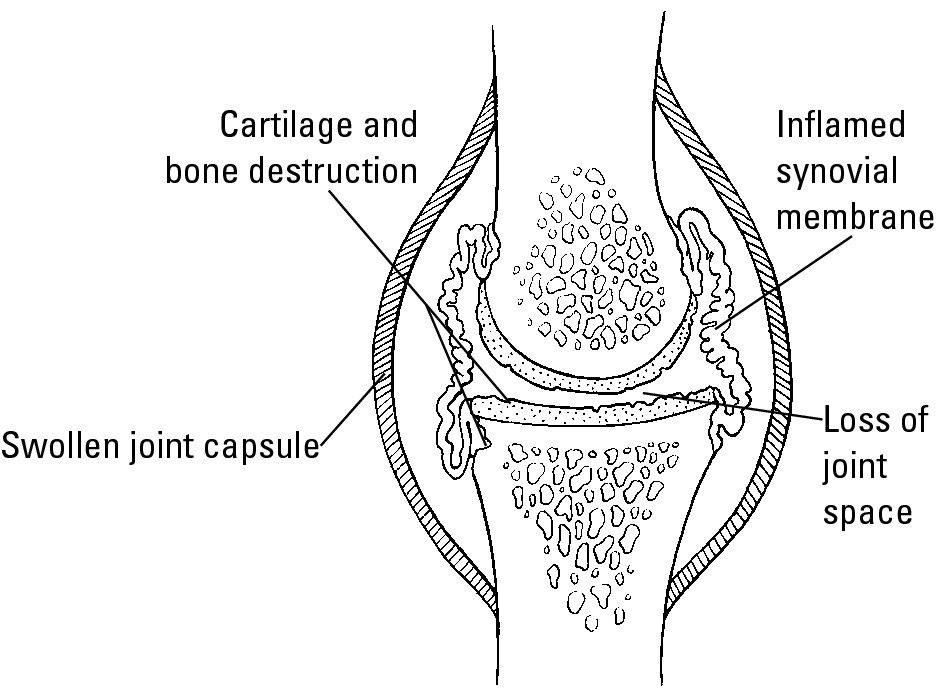
Figure 5-2: A synovial joint with inflammation in the synovial membrane.
Signs and symptoms of rheumatoid arthritis
RA affects women at a rate three to five times higher than men. It mainly affects the joints but also has signs and symptoms that affect the entire body. The major signs and symptoms include the following:
 Inflammation of the joints caused by cytokines produced by T cells with swelling, heat, and tenderness that’s usually (but not necessarily) symmetric
Inflammation of the joints caused by cytokines produced by T cells with swelling, heat, and tenderness that’s usually (but not necessarily) symmetric
 Inflammation of the lungs, the tissue surrounding the heart (called the pericardium), the tissue surrounding the lungs (called the pleura), and the white part of the eye (called the sclera)
Inflammation of the lungs, the tissue surrounding the heart (called the pericardium), the tissue surrounding the lungs (called the pleura), and the white part of the eye (called the sclera)
 Destruction of the cartilage, the smooth surfaces that permit unhindered movement of the joint, leading to joint deformity and loss of joint mobility
Destruction of the cartilage, the smooth surfaces that permit unhindered movement of the joint, leading to joint deformity and loss of joint mobility
 Nodular lesions under the skin, called rheumatoid nodules
Nodular lesions under the skin, called rheumatoid nodules
 Increased susceptibility to heart attacks and strokes
Increased susceptibility to heart attacks and strokes
 Loss of bone near the inflamed joint (cytokines stimulate bone loss by activating osteoclasts)
Loss of bone near the inflamed joint (cytokines stimulate bone loss by activating osteoclasts)
Constitutional symptoms, including the following:
 Fatigue
Fatigue
 Loss of appetite
Loss of appetite
 Loss of weight
Loss of weight
 Low-grade fever
Low-grade fever
 Morning stiffness
Morning stiffness
Diagnosis involves a blood test for a protein called the rheumatoid factor. This test isn’t flawless — 15 percent of patients who have the disease might not have rheumatoid factor in their blood whereas 10 percent of the normal population might have it there. Newer tests are being developed that are more specific for RA, but they aren’t perfect either. These new tests are for anticitrullinated protein antibodies or antimutated citrullinated vimentin.
Doctors use a multitude of anti-inflammatory and other drugs for RA, with variable results. (For more information about this autoimmune disease, check out Arthritis For Dummies, by Barry Fox.)
The role of vitamin D in RA
A number of findings have linked vitamin D to RA. Among the most important findings are the following:
 RA patients with serum 25-hydroxyvitamin D levels less than 20 ng/ml [50 nmol/L] have more tender joints and more evidence of inflammation compared to people with higher serum levels.
RA patients with serum 25-hydroxyvitamin D levels less than 20 ng/ml [50 nmol/L] have more tender joints and more evidence of inflammation compared to people with higher serum levels.
 Among 29,368 women who were followed for 11 years, those who took more than 400 IU of vitamin D as a supplement each day had a lower risk of developing RA.
Among 29,368 women who were followed for 11 years, those who took more than 400 IU of vitamin D as a supplement each day had a lower risk of developing RA.
 Vitamin D insufficiency (serum 25OH D of less than 15 ng/ml [37.5 nmol/L]) is common in African Americans with recent-onset RA.
Vitamin D insufficiency (serum 25OH D of less than 15 ng/ml [37.5 nmol/L]) is common in African Americans with recent-onset RA.
 Treating with a drug similar to calcitriol reduced joint inflammation and reduced RA in rats.
Treating with a drug similar to calcitriol reduced joint inflammation and reduced RA in rats.
None of the studies so far are randomized controlled trials, but those types of studies are getting underway. As a result, no consensus exists on the vitamin D dosage that may protect a person from RA or that may lessen the effects of the disease in an already affected patient. However, based on what we know so far, getting the blood level up to 20 ng/ml [50 nmol/L] simply makes sense in protecting against this disease.
Systemic lupus erythematosis
Systemic lupus erythematosis, often shortened to just lupus, is an autoimmune disease of the connective tissues that support and protect organs. It can affect every organ in the body because connective tissue surrounds all organs.
In lupus, antibodies form against the connective tissues in various parts of the body. Immune cells then destroy these tissues. The resultant signs and symptoms depend on which tissues are most affected.
Signs and symptoms of lupus
Lupus is nine times more common in women than men. Because lupus affects any organ in the body, signs and symptoms vary widely. Depending on where lupus starts, it may mimic other diseases, like rheumatoid arthritis.
The following are the most common signs and symptoms of lupus. Just remember the disease isn’t the same in everyone, so not all of the signs and symptoms are present in every person:
 Blood disorders, especially anemia.
Blood disorders, especially anemia.
 Brain and nervous system disorders, especially headaches and psychiatric problems, such as anxiety and psychosis.
Brain and nervous system disorders, especially headaches and psychiatric problems, such as anxiety and psychosis.
 General body problems, such as fever and fatigue.
General body problems, such as fever and fatigue.
 Heart problems due to inflammation in the tissue surrounding the heart (the pericardium), the heart muscle itself (the myocardium), and the inner lining of the heart (the endocardium).
Heart problems due to inflammation in the tissue surrounding the heart (the pericardium), the heart muscle itself (the myocardium), and the inner lining of the heart (the endocardium).
 Joint disorders, especially pain and inflammation, that aren’t as severe and destructive as rheumatoid arthritis.
Joint disorders, especially pain and inflammation, that aren’t as severe and destructive as rheumatoid arthritis.
 Kidney problems, such as blood in the urine, leading to kidney failure.
Kidney problems, such as blood in the urine, leading to kidney failure.
 Lung problems from inflammation of the tissue around the lungs (the pleura), as well as pneumonia.
Lung problems from inflammation of the tissue around the lungs (the pleura), as well as pneumonia.
 Skin disorders, especially a rash involving the nose and the face on either side of the nose, called a butterfly rash because of its appearance. Sunlight may bring on the rash.
Skin disorders, especially a rash involving the nose and the face on either side of the nose, called a butterfly rash because of its appearance. Sunlight may bring on the rash.
Doctors use a blood test called the antinuclear antibody test to diagnose lupus. However, this test is positive in other connective tissue diseases and in normal people as well, so a diagnosis of lupus is made only if some of the preceding symptoms are seen in addition to a positive blood test.
Although lupus can be a serious disease, the course of lupus is much less severe now than in the past. Many patients can live without symptoms, and many effective medications can control symptoms and prevent complications that lead to death.
The role of vitamin D in lupus
Association studies support the idea that vitamin D deficiency plays a role in the development and progression of lupus. These show that patients with lupus who have the most active disease have the lowest serum levels of 25-hydroxyvitamin D. Also, lower serum levels of 25-hydroxyvitamin D correlate with higher levels of autoantibodies in lupus.
There’s not a lot of evidence for vitamin D and lupus yet. But given the role that vitamin D plays in the adaptive immune response, scientists are continuing to look for how vitamin D might be used to help those affected by lupus.
Graves’ disease
Graves’ disease is an autoimmune disease in which the body’s metabolism speeds up. Graves’ disease is caused by an antibody that makes the thyroid gland produce too much thyroid hormone — the antibody activates the thyroid stimulating hormone (TSH) receptor. Graves’ disease is often accompanied by eye disease and skin disease.
Under normal circumstances, the pituitary gland in the brain makes TSH, which goes through the bloodstream to stimulate the thyroid gland (located in the neck) to make thyroid hormone. Thyroid hormone regulates metabolism in the body. Normally, if the thyroid isn’t making enough hormone, the pituitary secretes more TSH. If the thyroid makes too much, TSH is suppressed. In Graves’ disease the antibody mimics the effect of too much TSH even though the real level of TSH is very low.
Signs and symptoms
Graves’ disease is ten times more common in women than men. It usually begins between ages 30 and 60. It’s hereditary, passing from mother to daughter, but sometimes skips a generation. What is inherited is the tendency for autoimmune attack on the thyroid to occur, but a trigger to initiate the autoimmune attack is still needed. Known triggers for Graves’ disease include stress, illness, pregnancy, and other factors. Oddly enough, the risk of hypothyroidism is also increased in the same families that are at high risk for Graves’ disease.
The signs and symptoms of Graves’ disease include the following:
 Swollen knees with a waxy appearance
Swollen knees with a waxy appearance
 Bulging eyes with the whites showing above and below the pupil
Bulging eyes with the whites showing above and below the pupil
 Persistently high body temperature
Persistently high body temperature
 Weight loss resulting from muscle loss
Weight loss resulting from muscle loss
 Moist, warm skin from increased sweating
Moist, warm skin from increased sweating
 Rapid pulse felt as palpitations of the heart
Rapid pulse felt as palpitations of the heart
 Fine tremor of the fingers
Fine tremor of the fingers
 Weakness
Weakness
 Miscarriage of a pregnancy if uncontrolled
Miscarriage of a pregnancy if uncontrolled
 Increased bowel movements and sometimes diarrhea
Increased bowel movements and sometimes diarrhea
 Increased appetite, but weight loss because of the increased metabolism
Increased appetite, but weight loss because of the increased metabolism
 Loss of bone from increased breakdown, with increased fracture rate
Loss of bone from increased breakdown, with increased fracture rate
 Increased urination and thirst
Increased urination and thirst
 Increased reflexes
Increased reflexes
 Changes in hair (thinner, falling out) and nails (breaking easily, separating from nail bed)
Changes in hair (thinner, falling out) and nails (breaking easily, separating from nail bed)
Doctors diagnose Graves’ disease by measuring the amount of free (active) thyroid hormone and the amount of TSH in the blood. In Graves’ disease, active thyroid hormone is elevated, TSH is suppressed, and a thyroid scan shows the gland to be enlarged. Levels of antibodies against the TSH receptor can also be measured and will be elevated, but this test is usually done in exceptional circumstances such as pregnancy (because the antibody can cause Graves’ disease in the fetus).There are other causes of hyperthyroidism apart from Graves’ disease, including toxic nodules, multinodular goiters, and autoimmune thyroiditis.
Treating Graves’ disease
Doctors use three major forms of treatment for Graves’ disease:
 Antithyroid pills, either methimazole or propylthiouracil: These drugs suppress the thyroid’s ability to make thyroid hormone and return the blood levels to normal. During the time that the thyroid is suppressed, in some patients the autoimmune attack lets up and the patient is effectively cured (it doesn’t seem to be a direct effect of the drug, though). But in others the condition relapses weeks to years after the medication is stopped, and the patient needs to be retreated for a longer interval or indefinitely. I prefer this treatment because it’s the only one that can potentially cure the disease.
Antithyroid pills, either methimazole or propylthiouracil: These drugs suppress the thyroid’s ability to make thyroid hormone and return the blood levels to normal. During the time that the thyroid is suppressed, in some patients the autoimmune attack lets up and the patient is effectively cured (it doesn’t seem to be a direct effect of the drug, though). But in others the condition relapses weeks to years after the medication is stopped, and the patient needs to be retreated for a longer interval or indefinitely. I prefer this treatment because it’s the only one that can potentially cure the disease.
 Radioactive iodine: Thyroid hormone is made out of iodine, and the thyroid avidly takes up most of the iodine in the diet. When a radioactive form of iodine goes into the thyroid, it kills thyroid cells and cures the overactive thyroid that way. Most patients end up with low thyroid function and have to take thyroid hormone in the form of a pill for life.
Radioactive iodine: Thyroid hormone is made out of iodine, and the thyroid avidly takes up most of the iodine in the diet. When a radioactive form of iodine goes into the thyroid, it kills thyroid cells and cures the overactive thyroid that way. Most patients end up with low thyroid function and have to take thyroid hormone in the form of a pill for life.
 Surgical removal of the thyroid: This treatment usually results in low thyroid function because removing just enough thyroid to control Graves’ disease is difficult. It’s rarely done to treat Graves’ disease except in unusual circumstances, such as for a pregnant woman and those unable to tolerate the antithyroid medication (radioactive iodine cannot be safely used because it may destroy the fetal thyroid).
Surgical removal of the thyroid: This treatment usually results in low thyroid function because removing just enough thyroid to control Graves’ disease is difficult. It’s rarely done to treat Graves’ disease except in unusual circumstances, such as for a pregnant woman and those unable to tolerate the antithyroid medication (radioactive iodine cannot be safely used because it may destroy the fetal thyroid).
The role of vitamin D in Graves’ disease
There’s not a whole lot of evidence linking vitamin D to Graves’ disease; still, there’s enough that it’s worth considering. All of the following may link vitamin D and Graves’ disease:
 Vitamin D deficiency has been seen among female Graves’ disease patients from Japan.
Vitamin D deficiency has been seen among female Graves’ disease patients from Japan.
 Variations in the genes responsible for calcitriol signaling or calcitriol action (see Chapter 1) have been associated with a high incidence of Graves’ disease in some studies. This suggests that when calcitriol can’t work well in cells, a person might be more likely to get Graves’ disease. However, no one has tested to see if treating with vitamin D will prevent the onset of Graves’ disease or reduce its severity after it has occurred.
Variations in the genes responsible for calcitriol signaling or calcitriol action (see Chapter 1) have been associated with a high incidence of Graves’ disease in some studies. This suggests that when calcitriol can’t work well in cells, a person might be more likely to get Graves’ disease. However, no one has tested to see if treating with vitamin D will prevent the onset of Graves’ disease or reduce its severity after it has occurred.

