Chapter 6
Preventing Cancer
In This Chapter
 Understanding how vitamin D helps prevent the big C
Understanding how vitamin D helps prevent the big C
 Protecting against prostate cancer
Protecting against prostate cancer
 Derailing breast cancer
Derailing breast cancer
 Deflating lung cancer
Deflating lung cancer
 Avoiding ovarian cancer
Avoiding ovarian cancer
 Preventing pancreatic cancer
Preventing pancreatic cancer
 Curbing colon cancer
Curbing colon cancer
Cancer is a troublesome disease in the United States today. It’s scary when we hear that one of our loved ones or friends has cancer. But you may be surprised that as much as 70 percent of the cancers that occur each year may be preventable by things you can control. Some of these lifestyle decisions are pretty obvious — for example, don’t smoke and you dramatically reduce your risk of lung cancer.
Over the last 30 years, more and more evidence has accumulated that shows higher vitamin D status intake or higher 25-hydroxyvitamin D levels may prevent cancer. In 1980, Drs. Frank and Cedric Garland first proposed higher vitamin D status as the link that explains why people in the southern part of the United States have lower rates of colon cancer. They proposed that this was because the skin makes more vitamin D in the sunny south. Since then, 16 different cancers have been associated with low vitamin D!
In this chapter, I discuss the evidence for six cancers where vitamin D may play a preventive role. I think you’ll see that the evidence is compelling. Beyond these six, all of the following cancers have been linked in some way to reduced vitamin D:
 Bladder
Bladder
 Breast
Breast
 Colon
Colon
 Esophagus
Esophagus
 Gallbladder
Gallbladder
 Hodgkin’s lymphoma
Hodgkin’s lymphoma
 Kidney
Kidney
 Lung
Lung
 Non-Hodgkin’s lymphoma
Non-Hodgkin’s lymphoma
 Ovary
Ovary
 Pancreas
Pancreas
 Prostate
Prostate
 Rectum
Rectum
 Stomach
Stomach
 Uterus
Uterus
 Vulva
Vulva
The story on vitamin D and cancer is still ongoing. Most of the work done so far is either from cancer cells using calcitriol (active vitamin D) or from associations drawn between estimated sun-light exposure, vitamin D intake, or serum 25-hydroxyvitamin D levels and cancer risk in groups of people. There are still a lot of gaps in our understanding; however, assuming that low vitamin D causes cancer, some researchers estimate that more than 50,000 premature deaths from cancer could be prevented each year in the United States if people maintained sufficient levels of 25-hydroxyvitamin D in their blood.
Explaining How Cancer Develops
Cancer is a very complicated subject. It’s not really a single disease, but rather many related diseases. This is because each tissue forms a cancer in its own way and progresses according to its own plan. Some cancers develop quickly whereas others take a lifetime to develop. A prostate cancer can develop over decades before it is known whereas certain pancreatic and lung tumors can have very rapid growths. This means that diagnosis, treatment, and even prevention strategies can be different from one cancer to the next. In general, cancers go through a number of different steps:
 Uncontrolled cell growth: This leads to masses of cells that could be cancer or benign — like a polyp in the colon.
Uncontrolled cell growth: This leads to masses of cells that could be cancer or benign — like a polyp in the colon.
 Development of a new blood supply to the tumor: When this happens, the tumor can grow big.
Development of a new blood supply to the tumor: When this happens, the tumor can grow big.
 Invasion of tissues surrounding the cancer: This can damage the normal healthy tissue and make treatment more difficult.
Invasion of tissues surrounding the cancer: This can damage the normal healthy tissue and make treatment more difficult.
 Spread to distant tissues in the body: This process is called metastasis. When this happens, new tumors can grow all around the body. This is very hard to treat.
Spread to distant tissues in the body: This process is called metastasis. When this happens, new tumors can grow all around the body. This is very hard to treat.
In the following sections, I give you some general points about cancer that apply to most but certainly not all cancers.
Understanding how cell growth gets out of control
Cells normally have a strong system that limits them from growing or multiplying except when necessary. Like good plants, normal cells respect their boundaries, don’t crowd neighboring cells, and grow only when and where they’re supposed to. For example, your skin cells grow and divide slowly, except after you get a cut and you need to replace the injured skin. Occasionally, the genes that regulate this system acquire one or more defects called mutations. These gene mutations can be caused by environmental factors like cigarette smoke, UV rays of the sun, radiation from X-rays, pollutants, and other cancer-causing substances. Mutations can alter the function of many genes, but in cancer the most common mutations activate genes that cause cells to multiply, or they suppress genes that stop cells from multiplying. When several mutations are in the same cell, especially if both activating and suppressing genes are affected, a mass of cells grow and become a tumor.
Checking out the different types of tumors
Cancers are classified by the types of cells that make up the tumor. The various types are
 Carcinoma: A malignant tumor derived from the tissue that lines the cavities and surfaces of tissues throughout the body. These are the most common tumors and include breast cancer, colon cancer, lung cancer, and prostate cancer.
Carcinoma: A malignant tumor derived from the tissue that lines the cavities and surfaces of tissues throughout the body. These are the most common tumors and include breast cancer, colon cancer, lung cancer, and prostate cancer.
 Germ cell tumor: A malignant tumor derived from cells that can form any type of tissue, usually in the testicles and ovaries.
Germ cell tumor: A malignant tumor derived from cells that can form any type of tissue, usually in the testicles and ovaries.
 Lymphomas and leukemias: Malignant tumors derived from blood-forming cells.
Lymphomas and leukemias: Malignant tumors derived from blood-forming cells.
 Sarcomas: Malignant tumors derived from connective tissue, which provides structure and support in the body like cartilage, bone, and fat.
Sarcomas: Malignant tumors derived from connective tissue, which provides structure and support in the body like cartilage, bone, and fat.
Moving through the stages of cancer
The progression of cancer is broken into stages to provide general information about the prognosis of the cancer and the extent of treatment that is necessary or appropriate. In general, there are five stages of cancer:
 Stage 0: Only a few cells are involved and the cancer is just beginning.
Stage 0: Only a few cells are involved and the cancer is just beginning.
 Stage 1: The cancer is small and localized to the organ in which it originated.
Stage 1: The cancer is small and localized to the organ in which it originated.
 Stage 2: The tumor is larger and beginning to spread to surrounding tissues.
Stage 2: The tumor is larger and beginning to spread to surrounding tissues.
 Stage 3: Cancer cells are found in the lymph tissue (the tissue that contains immune cells and drains away infections) around the tumor.
Stage 3: Cancer cells are found in the lymph tissue (the tissue that contains immune cells and drains away infections) around the tumor.
 Stage 4: Cancer has spread to other areas of the body.
Stage 4: Cancer has spread to other areas of the body.
Another method of staging, which is often used in combination with the above stages, is the TNM staging. This stands for tumor size (T), lymph node involvement (N), and metastases (M, spread to other organs).
How Vitamin D Helps Prevent the Big C
Studies in cultured cells done with calcitriol show that it may affect cancer in numerous ways. This is different from the way many drugs work to affect biology. Drugs are designed to stop a specific part of how a cell works but calcitriol appears to influence more than just one type of process in a cell. Some of the most important capabilities of calcitriol seem to include the following:
 Suppressing the proliferation of cells; cancer arises from abnormal cell proliferation
Suppressing the proliferation of cells; cancer arises from abnormal cell proliferation
 Promoting the death of abnormal cells that may become cancerous
Promoting the death of abnormal cells that may become cancerous
 Preventing blood vessels from forming in a developing tumor, which keeps nutrients from the tumor and prevents it from getting bigger
Preventing blood vessels from forming in a developing tumor, which keeps nutrients from the tumor and prevents it from getting bigger
 Stopping cancer cells from spreading to other parts of the body, thereby preventing metastases, the spread of cancer to healthy organs
Stopping cancer cells from spreading to other parts of the body, thereby preventing metastases, the spread of cancer to healthy organs
Doctors are not yet at the point where they can recommend a specific level of 25-hydroxyvitamin D in the blood that can prevent or help to treat any specific cancer. Hopefully, future editions of this book will be able to answer that question.
Promoting normal cell growth
When vitamin D is converted to calcitriol (see Chapter 1 for details), it can decrease cell division and increase normal maturation of cells. Both of these events should slow the development of cancer. Calcitriol may do this in a number of ways:
 Stimulates the production of proteins, such as p21 and p27, which stop cells from multiplying.
Stimulates the production of proteins, such as p21 and p27, which stop cells from multiplying.
 Stimulates the production of E-cadherin, a protein that binds cells together. When E-cadherin is lost, cancer can leave the tumor and spread.
Stimulates the production of E-cadherin, a protein that binds cells together. When E-cadherin is lost, cancer can leave the tumor and spread.
 Inhibits the function of beta catenin, a protein that regulates genes that cause cells to multiply. Increased activity of beta catenin is involved in a number of cancers, including skin cancer, colorectal cancer, and ovarian cancer.
Inhibits the function of beta catenin, a protein that regulates genes that cause cells to multiply. Increased activity of beta catenin is involved in a number of cancers, including skin cancer, colorectal cancer, and ovarian cancer.
 Blocks the production and action of prostaglandins, fatty substances that promote the construction of blood vessels and stimulate cell growth.
Blocks the production and action of prostaglandins, fatty substances that promote the construction of blood vessels and stimulate cell growth.
Encouraging the death of abnormal cells
Calcitriol not only protects against the development and growth of cancer cells, but also destroys cells that may turn into cancer. It causes apoptosis (death) of cells that have acquired changes that could make them cancerous or malignant.
Calcitriol may cause cell death in two ways. First, it may stimulate apoptosis by prompting the release of calcium from special storage spots inside cells. In cancer cells, calcitriol can also block the production of proteins that prevent cell death while enhancing the production of proteins that cause cell death.
As a result, calcitriol may also sensitize cancer cells to cancer treatments like radiation therapy and chemotherapy, which further enhances the death of cancer cells.
Protecting cells from things that cause cancer
Scientists have been using new and sophisticated tools to examine all the ways that calcitriol might influence normal or cancerous cells. From these studies we’ve learned that calcitriol affects more than just controlling how cells multiply or die. Some of these new roles include:
 Induces the production of proteins that repair damage to the genes caused by factors like UV light from sunlight. DNA damage to genes is what causes mutations, and these mutations can affect the function of a gene thereby starting the process of cancer.
Induces the production of proteins that repair damage to the genes caused by factors like UV light from sunlight. DNA damage to genes is what causes mutations, and these mutations can affect the function of a gene thereby starting the process of cancer.
 Regulates the ability of cells to control molecules that can damage DNA or proteins. These molecules are called reactive oxygen species (ROS).
Regulates the ability of cells to control molecules that can damage DNA or proteins. These molecules are called reactive oxygen species (ROS).
 Suppresses the production of chemicals that cause inflammation. Inflammation is a process that can make cancer develop more quickly or aggressively.
Suppresses the production of chemicals that cause inflammation. Inflammation is a process that can make cancer develop more quickly or aggressively.
Taking steps if you already have cancer: Vitamin D’s effect
The current thinking is that vitamin D, as calcitriol, may help your body ward off cancer before it forms or that it slows and kills cancer cells at the earliest stages (soon after they’ve formed) so that it never develops into a disease that needs treatment by a doctor.
The reason for this is that cancer is a creative disease. It figures out ways to get around all of the protections your body has to fight it. For example, whereas your immune system normally recognizes abnormal cells and kills them, tumors have developed ways to shut down this protection. The same thing also seems to be happening with vitamin D. There is evidence that as a cancer moves through the stages to become more advanced, the cancer makes it harder for vitamin D to work. In some cancers the level or function of the vitamin D receptor is reduced; in others, enzymes that break down calcitriol are increased; and in others, the production of calcitriol is shut down in the cancer tissue.
However, doctors have seen all the good things that calcitriol appears to do to cancer cells in cell cultures, so they have also been trying to use calcitriol or drugs based on its structure as a way to treat established cancer. Calcitriol has been used alone and in combination with anti-cancer drugs. In general calcitriol has shown some promise of prolonging the length of a remission, but it doesn’t lead to a cure. One major problem is that calcitriol is so potent at controlling calcium metabolism that the levels needed to treat established cancer cause hypercalcemia (excessively high blood levels of calcium). Hypercalcemia, in any patient, can cause nausea, vomiting dehydration, weight loss, muscle weakness, confusion, and even coma and death. Consequently, calcitriol has been largely abandoned as a potential cancer treatment. Instead, researchers are looking at drugs with similar structures to calcitriol but which have less of an effect on serum calcium. None of these drugs have been proven in clinical studies to treat cancer and so none have yet become an approved treatment for cancer.
Blocking Colon Cancer
Of all the cancers proposed to have a relationship to vitamin D, perhaps colon cancer has the strongest connection. More properly called colorectal cancer because the disease may involve any part of the large intestine, including the rectum, colorectal cancer can be picked up in early and curable stages with proper screening.
Excluding skin cancer, colorectal cancer is the third most common cancer diagnosed in the United States, with about 140,000 new cases each year. The incidence is evenly split between men and women. About 51,000 people died of colorectal cancer in the United States in 2010.
Reviewing colorectal cancer
More than 80 percent of colorectal cancers are spontaneous and not related to family history. The cancers that form in the first part of the colon (proximal), last part of the colon (distal), and the rectum can form for different reasons. However, I’ll tell you some general features common to all of the forms. Colorectal cancer usually develops in mushroom-shaped growths called polyps that extend from the inner lining of the colon or rectum into the lumen. Most polyps aren’t malignant, but some develop into cancer.
Although most cases of colorectal cancer occur for unknown reasons, a number of factors increase the risk of developing colorectal cancer:
 African American background
African American background
 Alcoholism
Alcoholism
 Diet high in red meats, especially processed meats like luncheon meats
Diet high in red meats, especially processed meats like luncheon meats
 Family history of colorectal cancer
Family history of colorectal cancer
 History of colorectal polyps
History of colorectal polyps
 History of inflammatory bowel disease, including ulcerative colitis and Crohn’s disease
History of inflammatory bowel disease, including ulcerative colitis and Crohn’s disease
 Obesity
Obesity
 Older age (much more common after 50)
Older age (much more common after 50)
 Physical inactivity
Physical inactivity
 Smoking
Smoking
 Certain inherited conditions in which polyps are made
Certain inherited conditions in which polyps are made
Colorectal cancer has many signs and symptoms after it has enlarged or spread. The major ones include the following:
 Bowel obstruction when the tumor blocks the colon and prevents stool from moving through the intestine. This is uncomfortable and can lead to vomiting and life-threatening infection of the abdomen if the colon tears due to the strain (perforation).
Bowel obstruction when the tumor blocks the colon and prevents stool from moving through the intestine. This is uncomfortable and can lead to vomiting and life-threatening infection of the abdomen if the colon tears due to the strain (perforation).
 Change in bowel habits (constipation or diarrhea)
Change in bowel habits (constipation or diarrhea)
 Constitutional symptoms like weakness due to anemia, weight loss, and fever
Constitutional symptoms like weakness due to anemia, weight loss, and fever
 Dark stools from breakdown of blood in the colon
Dark stools from breakdown of blood in the colon
 Jaundice if the tumor spreads to the liver
Jaundice if the tumor spreads to the liver
 Rectal bleeding
Rectal bleeding
Excellent screening methods are available to detect colorectal cancer or polyps. Most screening turns up polyps or pre-cancerous growths. These are removed as a precautionary measure but don’t specifically predict that a person will get a colon tumor later. Colorectal screening methods include these major forms:
 Colonoscopy, visual examination with a long, flexible video camera that can be used to see most of the colon. If everyone over the age of 50 did this once every five years colonoscopy may reduce the death rate from colorectal cancer by 80 percent.
Colonoscopy, visual examination with a long, flexible video camera that can be used to see most of the colon. If everyone over the age of 50 did this once every five years colonoscopy may reduce the death rate from colorectal cancer by 80 percent.
 Examination of the rectum by the doctor’s gloved finger. Many tumors can be felt if they’re in the rectal area.
Examination of the rectum by the doctor’s gloved finger. Many tumors can be felt if they’re in the rectal area.
 Identification of carcinoembyronic antigen, a protein that the body produces when colorectal cancer is present. Details about the antigen can provide doctors with information about the size of the tumor.
Identification of carcinoembyronic antigen, a protein that the body produces when colorectal cancer is present. Details about the antigen can provide doctors with information about the size of the tumor.
 Sigmoidoscopy, direct visual examination with a short, stiff tube inserted into the rectum. This is like a colonoscopy but doesn’t look as far into the colon.
Sigmoidoscopy, direct visual examination with a short, stiff tube inserted into the rectum. This is like a colonoscopy but doesn’t look as far into the colon.
 Testing of the stools for blood.
Testing of the stools for blood.
 Virtual colonoscopy, using X-rays to see inside the colon. This form still requires visualization with a sigmoidoscope or colonoscope to do a biopsy, if necessary.
Virtual colonoscopy, using X-rays to see inside the colon. This form still requires visualization with a sigmoidoscope or colonoscope to do a biopsy, if necessary.
Colorectal cancer is staged to define the severity of the cancer and provide a basis for a person’s treatment and prognosis.
Treatment of colorectal cancer begins with surgery for the original cancer and for any spread that has occurred, if possible. After surgery, the patient undergoes chemotherapy in an effort to kill any remaining cancer cells and to prevent future spread of the disease. Many drugs and numerous regimens of treatment are used. Radiation therapy is done for rectal cancers but not for colon cancers.
Follow-up exams are done every three to six months after treatment for colon cancer. These can reduce the death rate from colon cancer by a substantial amount.
Understanding vitamin D’s possible role
As I told you earlier in this chapter, colorectal cancer was one of the first cancers proposed to be associated with low vitamin D status. These first studies showed:
 The incidence of colorectal cancer is higher the farther north people live, where they’re less able to make vitamin D in the skin during long winters.
The incidence of colorectal cancer is higher the farther north people live, where they’re less able to make vitamin D in the skin during long winters.
 Mortality (death) rates from colorectal cancer in the United States are highest in populations exposed to the least amount of natural sunlight. When the amount of sunlight that a population gets is divided into four parts, from least sunlight to more sunlight, to even more sunlight, to most sunlight, the death rate from colorectal cancer is exactly opposite.
Mortality (death) rates from colorectal cancer in the United States are highest in populations exposed to the least amount of natural sunlight. When the amount of sunlight that a population gets is divided into four parts, from least sunlight to more sunlight, to even more sunlight, to most sunlight, the death rate from colorectal cancer is exactly opposite.
Although it seemed logical that these relationships could be due to the lack of vitamin D production in the skin, these types of studies can be very misleading, so more research was needed. In the last two decades the evidence that vitamin D deficiency plays a role in colorectal cancer has greatly increased. Some major discoveries confirm this role:
 Calcitriol and synthetic drugs similar to it suppress the growth of colon cancer cells in cell culture experiments by reducing the production of new cancer cells, preventing colon cells from becoming abnormal, causing the death of cancer cells (apoptosis), and preventing blood vessels from feeding cancer tumors.
Calcitriol and synthetic drugs similar to it suppress the growth of colon cancer cells in cell culture experiments by reducing the production of new cancer cells, preventing colon cells from becoming abnormal, causing the death of cancer cells (apoptosis), and preventing blood vessels from feeding cancer tumors.
 Drugs designed to function like calcitriol reduce development of colon cancer caused by chemicals in mice and rats.
Drugs designed to function like calcitriol reduce development of colon cancer caused by chemicals in mice and rats.
 Diets deficient in vitamin D cause mice to develop colon tumors and for tumors to grow more quickly.
Diets deficient in vitamin D cause mice to develop colon tumors and for tumors to grow more quickly.
 In mice that don’t have the gene for the vitamin D receptor needed for the action of calcitriol, the cells of the colon multiply faster and acquire DNA damage that could lead to cancer-causing gene mutations.
In mice that don’t have the gene for the vitamin D receptor needed for the action of calcitriol, the cells of the colon multiply faster and acquire DNA damage that could lead to cancer-causing gene mutations.
 Vitamin D intakes less than 150 IU a day are associated with developing more colon cancer compared to intakes more than 500 IU per day.
Vitamin D intakes less than 150 IU a day are associated with developing more colon cancer compared to intakes more than 500 IU per day.
 Whether measurements of serum 25OH vitamin D are looked at directly or indirectly, an inverse relationship exists between vitamin D status and both occurrence and severity of colon cancer.
Whether measurements of serum 25OH vitamin D are looked at directly or indirectly, an inverse relationship exists between vitamin D status and both occurrence and severity of colon cancer.
This all suggests that one secret to preventing colon cancer is to avoid vitamin D deficiency; however, we don’t yet have strong, consistent evidence that higher serum 25-hydroxyvitamin D levels (more than 30 ng/ml [75 nmol/L]) caused by high levels of vitamin D intake (more than 1,500 IU per day) are better than the currently recommended blood level of 20 ng/ml [50 nmol/L] or intake of 600 IU per day). The question should be settled definitively within the next five years or so because a large clinical study called VITAL is randomizing 20,000 people to take higher doses of vitamin D versus placebo and looking to see if colorectal and other cancers are decreased.
Stopping Breast Cancer
Breast cancer is the most commonly diagnosed cancer in women in the United States after skin cancer. About 250,000 new cases of breast cancer were diagnosed in 2009, and about 40,000 deaths resulted from breast cancer. (For more information about this type of cancer, grab a copy of Breast Cancer For Dummies, by Ronit Elk, PhD, and Monica Morrow, MD [Wiley].)
Reviewing breast cancer
Breast cancer usually arises in the ducts of the breast that carry the milk to the nipple. Less often, it begins in the lobules of the breast where milk is formed.
A number of risk factors can contribute to breast cancer, beyond gender:
 Obesity
Obesity
 Lack of exercise
Lack of exercise
 Increased consumption of alcohol
Increased consumption of alcohol
 Estrogen supplementation in postmenopausal women
Estrogen supplementation in postmenopausal women
 Age (it occurs more in older women)
Age (it occurs more in older women)
 Personal or family history of breast cancer
Personal or family history of breast cancer
 Absence of pregnancies and lack of breastfeeding
Absence of pregnancies and lack of breastfeeding
 Abnormalities of two major breast cancer susceptibility genes, BRCA 1 and 2 (these abnormalities run in families)
Abnormalities of two major breast cancer susceptibility genes, BRCA 1 and 2 (these abnormalities run in families)
Like most cancers, breast cancer in its early stages does not have any symptoms. As the cancer enlarges, the following symptoms and signs occur:
 A painless lump in the breast or armpit that is hard and uneven
A painless lump in the breast or armpit that is hard and uneven
 Redness, dimpling, or puckering of the skin of the breast
Redness, dimpling, or puckering of the skin of the breast
 Discharge from the nipple that can be bloody
Discharge from the nipple that can be bloody
The diagnosis of breast cancer is usually made with a fine needle biopsy of the suspicious lump. Then the cancer is staged. This means classifying the cancer as follows:
 Stage 0 is premalignant. Cancer cells are present in the duct but don’t invade surrounding tissue.
Stage 0 is premalignant. Cancer cells are present in the duct but don’t invade surrounding tissue.
 Stage 1 cancer has cancerous cells invading nearby normal tissue.
Stage 1 cancer has cancerous cells invading nearby normal tissue.
 Stage 2 cancer has invaded lymph nodes or is no larger than 5 centimeters.
Stage 2 cancer has invaded lymph nodes or is no larger than 5 centimeters.
 Stage 3 cancer has spread beyond the lymph nodes under the arm.
Stage 3 cancer has spread beyond the lymph nodes under the arm.
 Stage 4 has spread to other organs, most often lungs, liver, bone, or brain. Only stage 4 is considered incurable.
Stage 4 has spread to other organs, most often lungs, liver, bone, or brain. Only stage 4 is considered incurable.
Treatment usually starts with surgery and depends on the size and spread of the cancer (that is, the stage of the cancer). After surgery, the patient generally undergoes radiation therapy and/or chemotherapy to kill any cancer cells that may have been left after removing the lump. Some cancers grow in response to estrogen; when that’s the case, agents that block estrogen action are given.
The prognosis for breast cancer recovery isn’t as good for younger women because the cancers they develop tend to be more aggressive. As a group, black women are more likely to die from breast cancer than white women. This is linked to lower incomes and reduced likelihood of insurance coverage, which reduces breast cancer screening and causes less intensive care after diagnosis.
Understanding vitamin D’s role
A number of studies exist from cells and animals that show calcitriol affects the cells of the breast and limits the growth of cancer cells. There are also some interesting associations between vitamin D intake or serum 25-hydroxyvitamin D and breast health. Consider some of the more important findings:
 Calcitriol decreases the proliferation of abnormal breast cells in cell cultures and blocks the actions of estrogen that tend to produce cancer cells.
Calcitriol decreases the proliferation of abnormal breast cells in cell cultures and blocks the actions of estrogen that tend to produce cancer cells.
 Mice without the vitamin D receptor gene have abnormal development of the breast and develop more severe breast cancer.
Mice without the vitamin D receptor gene have abnormal development of the breast and develop more severe breast cancer.
 Drugs developed to function like calcitriol can reduce the development of breast cancer in animal models by slowing the growth of tumor cells and by blocking their ability to spread.
Drugs developed to function like calcitriol can reduce the development of breast cancer in animal models by slowing the growth of tumor cells and by blocking their ability to spread.
 Breast cancer occurs less frequently in areas with more sunlight.
Breast cancer occurs less frequently in areas with more sunlight.
 Women with very low vitamin D intake (less than 200 IU per day) are more likely to have mammograms that indicate increased breast cancer risk.
Women with very low vitamin D intake (less than 200 IU per day) are more likely to have mammograms that indicate increased breast cancer risk.
 Several studies suggest that women with high blood 25(OH) vitamin D levels are less likely to develop breast cancer.
Several studies suggest that women with high blood 25(OH) vitamin D levels are less likely to develop breast cancer.
 High vitamin D intake reduces the pain associated with treatment of breast cancer by a class of drugs called aromatase inhibitors.
High vitamin D intake reduces the pain associated with treatment of breast cancer by a class of drugs called aromatase inhibitors.
Although proof is lacking that suggests taking higher amounts of vitamin D will prevent breast cancer, these studies point to a clear benefit of avoiding vitamin D deficiency if you want to limit your risk of breast cancer. For women, this makes two good reasons to get enough vitamin D — better bones, and less risk of breast cancer.
Looking at Prostate Cancer
Prostate cancer is the most common cancer in men in the United States, and it generally occurs in men over the age of 50; however, prostate cancer is slow growing in most men and takes a lifetime to develop. When doctors looked at the prostates of car accident victims, they were surprised to find that even men in their early twenties have the earliest stages of prostate cancer.
Because of this, prostate cancer is diagnosed frequently but kills much less often. For example, in 2008, 186,000 new cases emerged, but just 28,600 deaths resulted from prostate cancer.
Prostate cancer has been found in the prostate gland of more than 80 percent of men over the age of 70 who died from an entirely unrelated disease. Some doctors are concerned that the major test for detecting prostate cancer, the prostate specific antigen or PSA test, is overused. Its major weakness is that it not only picks up prostate cancer, but it also detects another prostate condition that isn’t cancer called benign prostatic hypertrophy (BPH). Unfortunately, when men get a positive PSA test, many of them may have had radical prostatectomy (surgical removal of the prostate) and then suffered from problems with erections and urinary incontinence. (For more information about this disease, check out Prostate Cancer For Dummies, by Paul H. Lange, MD, and Christine Adamec [Wiley].)
Reviewing prostate cancer
Prostate cancer occurs in the prostate gland, a tiny gland that surrounds the urethra, the tube that carries urine and semen through the penis out of the body. The prostate is only 20 grams in size, and its function is to make seminal fluid to carry sperm from the testicles. Figure 6-1 shows the location of the prostate gland.
Prostate cancer is linked to many risk factors beyond gender, including the following:
 Age: The older you are, the more likely you are to be diagnosed with prostate cancer.
Age: The older you are, the more likely you are to be diagnosed with prostate cancer.
 Race: African Americans are 60 percent more likely to develop prostate cancer than Caucasians.
Race: African Americans are 60 percent more likely to develop prostate cancer than Caucasians.
 Family history: Men whose fathers or brothers develop prostate cancer are more likely to develop it.
Family history: Men whose fathers or brothers develop prostate cancer are more likely to develop it.
 Smoking: This bad habit is probably a risk factor for more aggressive prostate cancer.
Smoking: This bad habit is probably a risk factor for more aggressive prostate cancer.
Most prostate cancers cause no symptoms, but when they’ve grown to become clinically important, they may cause these issues:
 Pain in the pelvic area
Pain in the pelvic area
 Difficulty urinating (this is also seen in the non-cancer condition BPH)
Difficulty urinating (this is also seen in the non-cancer condition BPH)
 Difficulty having an erection
Difficulty having an erection
 Bone pain if the cancer has spread to bone
Bone pain if the cancer has spread to bone
Prostate cancer is diagnosed with a biopsy of the prostate gland.
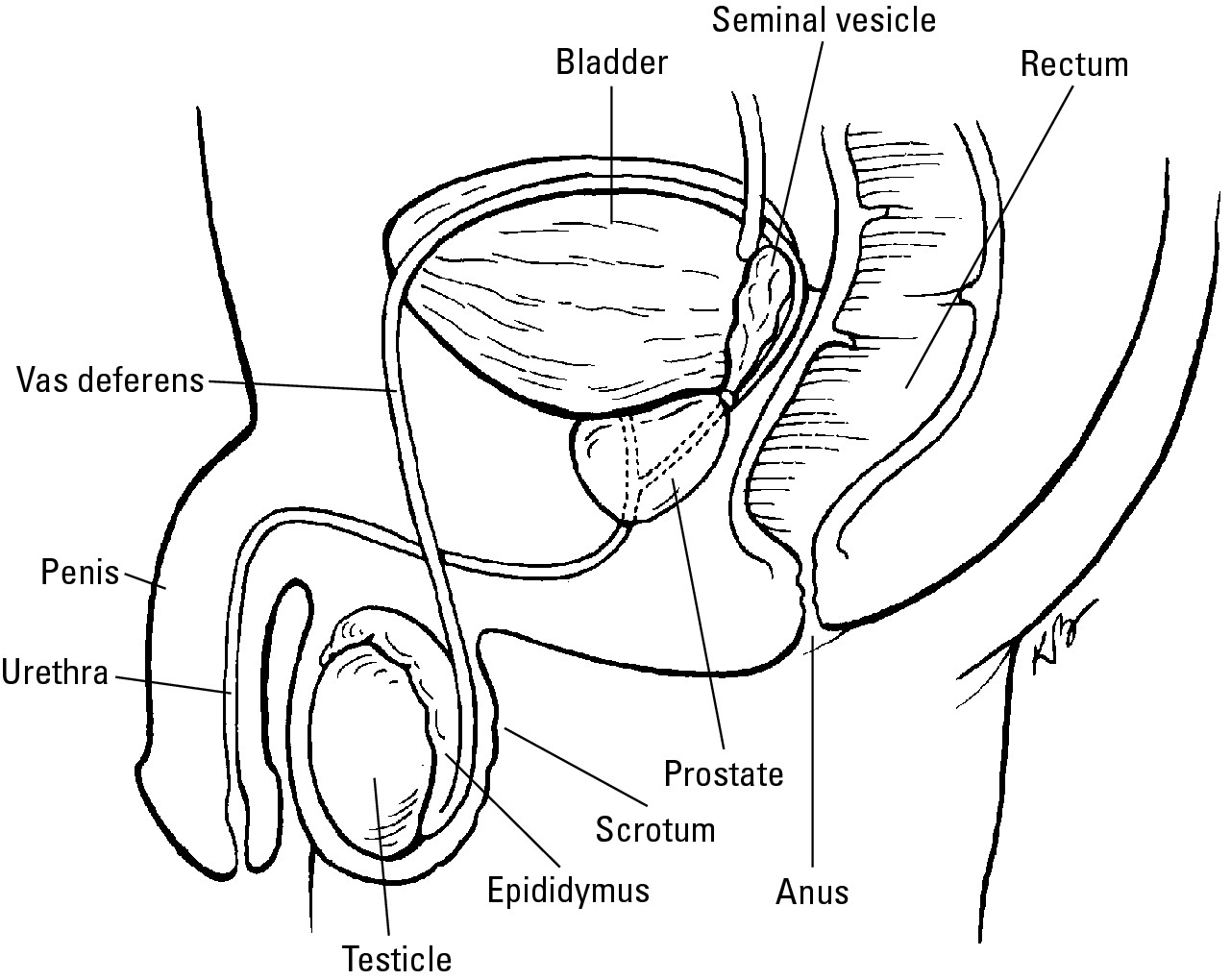
Figure 6-1: The location of the prostate and other male reproductive organs.
Treatment of prostate cancer follows several paths:
 Active surveillance (sometimes called watchful waiting), in which the patient is monitored for symptoms or growth of the tumor but no treatment is performed until clear evidence of danger arises, such as rapid growth or obvious symptoms (the PSA test is useful during this time because it’s already understood that the person has cancer)
Active surveillance (sometimes called watchful waiting), in which the patient is monitored for symptoms or growth of the tumor but no treatment is performed until clear evidence of danger arises, such as rapid growth or obvious symptoms (the PSA test is useful during this time because it’s already understood that the person has cancer)
 Surgery, in which the prostate is entirely removed
Surgery, in which the prostate is entirely removed
 Radiation therapy
Radiation therapy
 Cryosurgery (freezing of the tissue, which leads to death of the prostate tissue, including the cancer)
Cryosurgery (freezing of the tissue, which leads to death of the prostate tissue, including the cancer)
 Chemotherapy with drugs that kill the cancer
Chemotherapy with drugs that kill the cancer
 Hormone therapy to block the effect of testosterone to stimulate growth of normal and cancerous prostate cells
Hormone therapy to block the effect of testosterone to stimulate growth of normal and cancerous prostate cells
 Some combination of these treatments
Some combination of these treatments
Understanding vitamin D’s role
Although scientists think vitamin D affects prostate cancer, there are more gaps in the evidence. Here is evidence that makes scientists think vitamin D may be protective:
 The risk of prostate cancer appears to be higher in people who live in places where sunlight is limiting. Interestingly, if you have high sunlight exposure when you’re young, you may be protected from prostate cancer throughout your life, even if you move more north.
The risk of prostate cancer appears to be higher in people who live in places where sunlight is limiting. Interestingly, if you have high sunlight exposure when you’re young, you may be protected from prostate cancer throughout your life, even if you move more north.
 African American men have the lowest levels of vitamin D in their blood and the highest levels of both prostate cancer and death from prostate cancer in the United States.
African American men have the lowest levels of vitamin D in their blood and the highest levels of both prostate cancer and death from prostate cancer in the United States.
 In men with prostate cancer, PSA levels rise more slowly in the spring and summer, when vitamin D production in skin is normally highest.
In men with prostate cancer, PSA levels rise more slowly in the spring and summer, when vitamin D production in skin is normally highest.
 Calcitriol and drugs designed to function like it reduce the growth of prostate cancer cells and slow the growth of prostate tumors in animal models.
Calcitriol and drugs designed to function like it reduce the growth of prostate cancer cells and slow the growth of prostate tumors in animal models.
 Prostate cells can make active vitamin D from 25-hydroxy-vitamin D.
Prostate cells can make active vitamin D from 25-hydroxy-vitamin D.
These studies suggest that higher intakes of vitamin D could protect men from prostate cancer. Unfortunately, when researchers have looked for a relationship between serum 25-hydroxyvitamin D and the risk of prostate cancer, the results have been confusing. Some studies show that near deficient levels of vitamin D status increase prostate cancer risk, some show that serum 25-hydroxy-vitamin D levels don’t relate at all to prostate cancer risk, and still others show that high serum 25-hydroxyvitamin D levels may lead to higher levels of prostate cancer. I think that this confusion is because prostate cancer is so slow growing — what we really need to know is whether a lifetime of high vitamin D status is protective, but we can’t measure that. This is why it is crucial for researchers to test these ideas in animal models and translate them to humans with clinical intervention studies.
Vitamin D and Other Cancers
The three cancers I just described are the ones where researchers have the best evidence to support the idea that higher vitamin D intakes or 25-hydroxyvitamin D levels may be protective. Even with these cancers we have some gaps that make it hard to give specific recommendations about how much vitamin D you need — but we’re getting close.
As scientists have seen these studies, they’ve expanded their view and started asking if vitamin D might be involved in other cancers. So far their studies have been very promising. The following are other cancers that may respond to vitamin D.
Halting lung cancer
Lung cancer is the most common deadly cancer among both men and women. In the United States in 2009, about 220,000 new cases of lung cancer were diagnosed. That same year, about 153,000 people died of lung cancer. People over age 65 are mostly affected.
It’s no secret that long-term exposure to smoke from cigarettes causes lung cancer. Of the 15 percent of lung cancer patients who haven’t been exposed to smoke, other factors, like exposure to radon gas, asbestos, and air pollution, are responsible.
Reviewing lung cancer
Lung cancer is classified according to the type of cell involved. Two major types make up 97 percent of all lung cancers. Most lung cancers (80 percent) are non-small-cell lung cancers. The other 17 percent are small-cell lung cancers, which, despite being made up of small cells, produce a large tumor. The small-cell cancers contain hormones that can cause abnormalities like high calcium from production of a hormone that mimics parathyroid hormone. Another hormone produced inappropriately by small-cell cancers is antidiuretic hormone that results in low blood sodium and fluid overload.
Lung cancer has the following signs and symptoms:
 Constant cough
Constant cough
 Cough that produces blood
Cough that produces blood
 Difficulty swallowing
Difficulty swallowing
 Hoarse voice
Hoarse voice
 Pain in the chest or abdomen
Pain in the chest or abdomen
 Pneumonia
Pneumonia
 Shortness of breath
Shortness of breath
 Spread to the brain, bones, liver, and kidney
Spread to the brain, bones, liver, and kidney
 Weight loss and loss of appetite
Weight loss and loss of appetite
A chest X-ray is the first study done to look for lung cancer. It may show the tumor and/or widening of the structures in the middle of the chest from the cancer’s spread to the lymph nodes there. The tumor then is biopsied to make a definitive diagnosis.
Treatment depends on the type of cell, the amount of spread, and the physical fitness of the patient. The treatments include surgical removal (if possible), chemotherapy, and radiation therapy. Surgery can involve anything from removing part of the lobe of the lung in which the tumor is found, to removing an entire lung. As with other cancers, the tumor is staged based on how much spread has occurred at the time of diagnosis.
Prognosis for either type of lung cancer is poor. By the time the diagnosis is made, the cancer is usually advanced. It makes good sense to try to prevent lung cancer instead of treating it after it has occurred.
The single best lung cancer prevention advice is to reduce or stop smoking. Smoking has been reduced in the United States and throughout the world by laws prohibiting smoking in public places. If a person stops smoking before age 45, he is at low risk of developing cancer.
Understanding vitamin D’s role
Several discoveries seem to point to a relationship between normal levels of vitamin D and the prevention of lung cancer. Some of the more significant include the following:
 Normal lung tissue, premalignant lung tissue, and malignant lung tissue all have the vitamin D receptor. For calcitriol to perform its anti-cancer work, it has to be able to bind to the appropriate tissue.
Normal lung tissue, premalignant lung tissue, and malignant lung tissue all have the vitamin D receptor. For calcitriol to perform its anti-cancer work, it has to be able to bind to the appropriate tissue.
 There is an inverse association between the amount of exposure to ultraviolet B rays (the rays of sun that are responsible for triggering vitamin D production in your body; see Chapter 1) and the occurrence of lung cancer. The more exposure, the less common the cancer.
There is an inverse association between the amount of exposure to ultraviolet B rays (the rays of sun that are responsible for triggering vitamin D production in your body; see Chapter 1) and the occurrence of lung cancer. The more exposure, the less common the cancer.
 Patients who have surgery for lung cancer during the summer, when ultraviolet B is at its height, have a better prognosis than those who have surgery in the winter.
Patients who have surgery for lung cancer during the summer, when ultraviolet B is at its height, have a better prognosis than those who have surgery in the winter.
What we’re missing to complete this story are studies that show lung cells or lung cancer cells are influenced by calcitriol; that high serum levels of 25-hydroxyvitamin D are associated with low lung cancer risk; and that giving vitamin D supplements to people with low vitamin D status help them avoid lung cancer.
Deterring ovarian cancer
The ovaries are oval organs found in pairs in the female reproductive system. Figure 6-2 shows the location of the ovaries. Within the ovaries, eggs are produced, along with estrogen and progesterone.
Ovarian cancer may arise in the ovaries. In 2009, about 21,550 cases were diagnosed and 14,600 women died of ovarian cancer in the United States. Ovarian cancer is usually a cancer of women older than age 60 and is more common in White than Black women.
Reviewing ovarian cancer
Several factors increase the risk for ovarian cancer:
 Infertility
Infertility
 Endometriosis, in which cells of the uterus are found outside the uterus, such as on the ovaries, causing pain and bleeding, especially during menstruation
Endometriosis, in which cells of the uterus are found outside the uterus, such as on the ovaries, causing pain and bleeding, especially during menstruation
 Postmenopausal estrogen supplementation
Postmenopausal estrogen supplementation
Factors that decrease the risk for ovarian cancer include use of combined estrogen/progesterone oral contraceptives and contraception by tubal ligation (tying off the fallopian tubes).
Ovarian cancer is associated with a number of signs and symptoms, but none that are specific to ovarian cancer. Consider the most important:

Figure 6-2: Location of the ovaries and other female reproductive organs.
 Back pain
Back pain
 Bloating
Bloating
 Digestive symptoms, including constipation and lack of appetite
Digestive symptoms, including constipation and lack of appetite
 A feeling of being full early
A feeling of being full early
 Irregular menstrual cycles
Irregular menstrual cycles
 Pain in the pelvis or abdomen
Pain in the pelvis or abdomen
 Swollen abdomen
Swollen abdomen
 Vaginal bleeding
Vaginal bleeding
 Vague lower abdominal pain
Vague lower abdominal pain
Ovarian cancer isn’t usually diagnosed in its early stages because it tends to cause symptoms that aren’t specific to the disease. When ovarian cancer is suspected, a pelvic examination and CT scan can diagnose it. A definitive diagnosis requires a biopsy of the mass in the ovary.
Treatment of ovarian cancer starts by surgically removing the ovary and fallopian tube. If the cancer has spread, chemotherapy is added to the treatment. Radiation therapy isn’t usually used because the ovaries are located near other vital organs.
The prognosis for ovarian cancer is poor because the diagnosis is generally made so late in the disease. Complications that may occur include fluid in the abdomen, intestinal obstruction, and spread to other organs. The five-year survival is 45 percent.
Understanding vitamin D’s role
The evidence that a lack of vitamin D plays a role in the occurrence of ovarian cancer is interesting; however, this relationship isn’t secure yet.
Evidence that vitamin D plays a role in preventing and treating ovarian carcinoma includes the following:
 Calcitriol slows the growth and increases apoptosis (death) of cultured ovarian cancer cells.
Calcitriol slows the growth and increases apoptosis (death) of cultured ovarian cancer cells.
 Drugs designed to act like calcitriol inhibit the growth of ovarian cancer in animal models.
Drugs designed to act like calcitriol inhibit the growth of ovarian cancer in animal models.
 Results from several smaller studies suggest that higher 25-hydroxyvitamin D levels might be protective against ovarian cancer; however, a recent study that combines several smaller studies shows this may be limited to overweight women.
Results from several smaller studies suggest that higher 25-hydroxyvitamin D levels might be protective against ovarian cancer; however, a recent study that combines several smaller studies shows this may be limited to overweight women.
Fending off pancreatic cancer
Pancreatic cancer is another cancer that’s hard to treat at an early stage and generally has a poor prognosis because of its location in relation to other critical organs (see Figure 6-3). The pancreas has two major functions: producing hormones, insulin, glucagon, and somatostatin to control the glucose (sugar) in the body, and producing enzymes that go into the small intestine and help to break down food into particles that the body can absorb.
Most of the pancreas lies behind the stomach. Any tumors that grow can’t be felt until they’re so large that the cancer is very advanced. For this reason, pancreatic cancer has a high mortality rate. About 42,500 new cases occur in the United States every year, and 35,250 deaths occur from pancreatic cancer.
Reviewing pancreatic cancer
Pancreatic cancers usually arise from the tissue that makes the enzymes for the small intestine rather than the tissue that makes the hormones. This cancer is called a “silent killer” because of a lack of early symptoms and nonspecific later symptoms. Other pancreatic cancers arise from the hormone-producing cells of the pancreas, called the islets. These cancers can be silent or they may cause low blood sugar (hypoglycemia) due to an insulin-producing tumor (insulinoma).

Figure 6-3: The location of the pancreas.
Pancreatic cancer has many risk factors, some of which can be avoided and others that can’t. The most important are listed here:
 African American background
African American background
 Diabetes mellitus
Diabetes mellitus
 Excessive red meat in the diet
Excessive red meat in the diet
 Lack of vegetables and fruits in the diet
Lack of vegetables and fruits in the diet
 Family history of pancreatic cancer
Family history of pancreatic cancer
 Male sex
Male sex
 Obesity
Obesity
 Older age (older than 60)
Older age (older than 60)
 Smoking (responsible for 30 percent of pancreatic cancers)
Smoking (responsible for 30 percent of pancreatic cancers)
The most common signs and symptoms include the following:
 Diabetes (see Chapter 8), as the tumor replaces the tissue that produces insulin
Diabetes (see Chapter 8), as the tumor replaces the tissue that produces insulin
 Dark urine from jaundice
Dark urine from jaundice
 Loss of appetite, with nausea and vomiting
Loss of appetite, with nausea and vomiting
 Loss of weight
Loss of weight
 Pain in the upper abdomen and back
Pain in the upper abdomen and back
 Painless jaundice (yellow eyes and skin)
Painless jaundice (yellow eyes and skin)
The diagnosis of pancreatic cancer is usually made at a late stage, when a patient complains of pain in the abdomen, has experienced weight loss, and has jaundice. The patient then usually has a computed tomography (CT) scan to find the location of the cancer.
If the tumor is still localized to the pancreas, the first line of treatment is surgical removal of the tumor. Next, chemotherapy is given, but this is usually just to give the patient a few more months to live.
Because pancreatic cancer is usually diagnosed late and the recovery from the disease is rare, some think that prevention is more feasible than treatment. Up to 30 percent of pancreatic cancer may be prevented by stopping smoking.
Understanding vitamin D’s role
Some evidence suggests that vitamin D may play an important role in pancreatic cancer. Consider these points:
 The amount of ultraviolet B irradiation from sun is inversely associated with the occurrence of pancreatic cancer worldwide.
The amount of ultraviolet B irradiation from sun is inversely associated with the occurrence of pancreatic cancer worldwide.
 Calcitriol and drugs designed to act like calcitriol can slow the growth of pancreatic cancer cells in culture and in animal models.
Calcitriol and drugs designed to act like calcitriol can slow the growth of pancreatic cancer cells in culture and in animal models.
 Pancreatic cancer risk was higher in both the Nurses Health Study and the Health Professionals Follow-Up Study when vitamin D intake was lower than 150 IU per day. Protection due to vitamin D was maximized when intake was over 300 IU per day.
Pancreatic cancer risk was higher in both the Nurses Health Study and the Health Professionals Follow-Up Study when vitamin D intake was lower than 150 IU per day. Protection due to vitamin D was maximized when intake was over 300 IU per day.
It’s studies like these that make some vitamin D experts cautious about blanket recommendations to raise vitamin D intake to high levels. If the cancer-preventing effects of calcitriol are real, it may be that the doses currently recommended for bone health are all that’s needed to achieve them.
The evidence for pancreatic cancer is consistent with other studies that show it’s important to avoid becoming vitamin D deficient (serum 25-hydroxyvitamin D levels less than 10 ng/ml [25 nmol/L]). The current recommendations from the Institute of Medicine expert panel will get you there.
A Caveat about Vitamin D and Cancer
The evidence that vitamin D prevents many cancers seems overwhelming to some; however, the studies done in cell cultures with calcitriol don’t tell us what intake of vitamin D or blood level of 25-hydroxyvitamin D is needed to achieve that effect in humans. In addition, all the studies that connect vitamin D to cancer in human populations so far are epidemiologic. That is, they show inverse associations between interventions that lead to more skin synthesis of vitamin D (such as UVB light) or higher serum levels of 25-hydroxyvitamin D and the likelihood that a person will develop cancer (for example, high vitamin D status = low cancer risk). The problem is that these types of studies don’t directly prove that vitamin D is preventing cancer. These association studies could be affected by other things.
For example, factors other than vitamin D correlate with sun exposure. In this case, higher serum 25-hydroxyvitamin D might be a marker for the fact that you do a lot of outdoor exercise. Because exercise has been shown to prevent many cancers, a study that relates vitamin D to cancer through UV exposure of geography could really be showing you that exercise prevents cancer. Similarly, high vitamin D status might just indicate that you’re health conscious. A person who’s health conscious is more likely to exercise and follow a healthy diet rich in fruits and vegetables with little meat, especially processed meats (hot dogs and luncheon meats). In this case, high vitamin D status is just a marker of other lifestyle factors that protect you from cancer.
If this sounds far-fetched, then beware that we’ve been through this before and fooled several times. Lower intakes of vitamin E and beta carotene were associated with cancers, heart disease, and other adverse health outcomes. Some experts at the time thought that this was enough to say that taking higher doses of these “anti-oxidants” would prevent these diseases, while other experts worried that people who had higher intakes of vitamin E and beta carotene were simply healthier for numerous reasons. Large randomized trials were eventually done which proved that the anti-oxidants did nothing, and so the associational studies were wrong. It’s because of examples like this that medical research cannot stop with associational studies that suggest possible benefits of higher versus lower blood levels or intakes of vitamin D. We have to go on to prove that taking a higher intake of vitamin D leads to the benefit suggested by the associational studies.
For this reason experts base their decisions about vitamin D recommendations on evidence in the form of controlled clinical trials. The “gold standard” for clinical research trials is a double-blind placebo-controlled study. Here not only is a controlled dose of vitamin D given, but neither the study participant nor the researcher knows who is getting what dose of vitamin D until the end of the study (that’s where the “blind” comes in). Fortunately, the U.S. National Institutes of Health has funded a major vitamin D treatment study to evaluate the health claims of vitamin D. This study is following 20,000 people — some of whom are getting 2,000 IU of vitamin D a day and others who are getting a placebo (a control pill). Researchers won’t know the results of this study for several years.


