In this chapter, we look at ways to cope with some of the more common discomforts of pregnancy. Being pregnant causes changes in your body; some of them are uncomfortable. Being aware of what they are before you experience them (if you do) may help relieve anxiety.
If you experience back pain during pregnancy, you’re not alone. Between 50 and 80% of all women have back and hip pain at some time during pregnancy. Pain usually occurs during the third trimester as your tummy grows larger. However, pain may begin early in pregnancy and last until well after delivery (up to 5 or 6 months).
It’s more common to have mild backache than severe problems. You may experience backache after walking, bending, lifting, standing or excessive exercise. Some women need to be careful getting out of bed or getting up from a sitting position. Be careful to lift correctly.
The hormone relaxin may be part of the problem. It’s responsible for relaxing joints that allow your pelvis to expand to deliver your baby. However, when joints relax, it can lead to pain in the lower back and legs. Other factors include your weight gain (another good reason to control your weight), larger breasts and your bigger tummy, which can cause a shift in posture.
A change in joint mobility may cause discomfort in the lower back, especially during the last part of pregnancy. All your joints are looser. Check with your healthcare provider if back pain is a persistent problem for you.
Lower-back pain is common during pregnancy, but occasionally it indicates a serious problem, such as a kidney stone. If pain is constant or severe, contact your healthcare provider.
What can you do to prevent or lessen your pain? Try some or all of the following tips as early in pregnancy as possible. They’ll pay off for you later in pregnancy.
•Watch your weight gain; avoid gaining too much weight or gaining weight too fast.
•Stay active; continue exercising during pregnancy. Exercise to strengthen stomach, arm and thigh muscles.
•Swimming, walking and nonimpact aerobics may be beneficial.
•Do your Kegel exercises (see page 208).
•Practice good posture.
•Lift correctly—place feet shoulder-width apart, under your buttocks. Bend at the knees; lift with arms and legs, not your back!
•Get up and move around often. Don’t stand or sit in the same place for a long time.
•Stretch muscles to keep them limber.
•Be sure your mattress provides good support.
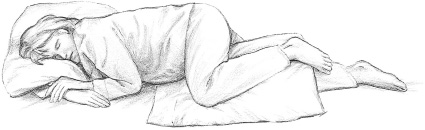
•Lie on your side when you sleep. Sleep on your left side with a pillow between your knees to align legs. Many pillows on the market are designed specifically for this purpose.
•Get out of bed slowly, swinging your legs to the floor and pushing up with your arms. Don’t twist.
•Take a warm (not hot) bath.
•Get a prenatal massage.
•Get off your feet and lie down for 30 minutes on your side.
•Use heat on the painful area.
•Ask your healthcare provider about wearing a lower-back brace or pregnancy support garment.
Treat backache with heat, rest and analgesics, such as acetaminophen. When you have lower-back pain, use an ice pack for up to 30 minutes three or four times a day. If pain lasts, switch to a heating pad, sticking with the same regimen.
Use extra pillows to support your abdomen or your legs as your pregnancy progresses.
During the first stages of your pregnancy, you may find one of the main things on your mind is getting enough rest. Fatigue is one of the first signs of pregnancy. Do yourself a favor by taking it easy and resting when possible. Don’t worry—fatigue is normal, especially in early pregnancy. Your body uses a lot of energy as your baby grows.
Don’t lie on your back or stomach when you sleep or rest; learn to sleep on your side early in pregnancy. After week 16, lie only on your side. As your uterus grows, it presses on important blood vessels that run down the back of your abdomen. Lying on your back decreases circulation to your baby and to the lower parts of your body. You may notice it’s harder to breathe when you lie on your back.
When you’re resting or sleeping, elevate your feet to keep blood moving throughout your body, especially your legs. Rest your top leg on a pillow. Pregnancy pillows that support the entire body can offer great relief.
Drink lots of fluids. Watch your diet; avoid sugar because it can make fatigue worse. If you can’t sleep enough at night to make you feel rested, nap during the day. If you can’t nap, sit down and relax—listen to music or read if that helps. When you relax, lie on your side to help ease any swelling or discomfort in your legs. Use extra pillows to support your abdomen or your legs as your pregnancy progresses.
Pregnancy is stressful! Studies show pregnancy ranks #12 in a list of life’s most stressful events. Normal stress probably won’t hurt you or your pregnancy, but major stress may increase your risk of premature birth. Learning to manage stress can go a long way in making your life more manageable—when you’re pregnant and when you’re not!
During pregnancy, stress can be caused by many things. Hormone changes can cause you to react in ways that aren’t normal for you, which can be stressful. Your body is changing, which stresses many women. You may have worked very hard to get and/or to maintain your figure. Now that you’re pregnant, there’s not much you can do about it.
You can’t always eliminate stress, but you can learn to cope with it. The following suggestions may help you deal with everyday stressful situations.
•Get enough sleep each night. Lack of sleep can make you feel stressed.
•Rest and relax during the day. Read or listen to music during a quiet period. Slow down your daily activities.
•When you feel anxious or upset, practice deep breathing and relaxation exercises you learn in childbirth-education classes.
•Talk about it instead of acting out when you have problems. Be specific and listen to what others tell you in response. Work together toward practical solutions.
•Take time out. When stress gets to be too much for you, go into another room and stretch, practice breathing exercises or listen to soothing music.
•When you feel stressed, stop and take a few slow, deep breaths to help turn off the stressed part of your nervous system.
•Set realistic priorities. Manage your time with priorities in mind. Use a daily calendar. Learn to say, “No.”
•Exercise can help you work off stress. Take a walk or visit the gym. Put on an exercise video for pregnant women. Do something active and physical (but not too physical) to relieve stress. Ask your partner to join you.
•Turn your thoughts to good things; it actually sends a chemical message to your brain that flows through your entire body and helps you relax.
•Eat nutritiously. Having enough calories available through the day will help avoid “lows.”
•Decide to be more positive. Smiling instead of frowning can help ease stress.
•Do something you enjoy, and do it for you.
•If smells are important to you, include them in your life. Burn scented candles, or buy fragrant flowers to help you relax.
•Seek help. You may need outside help to make it through a difficult time or to change behavior patterns. If necessary, ask your healthcare provider for a referral.
•Don’t go it alone. Share concerns with your partner, or find a group of pregnant women you can talk with.
Pregnancy can also make your partner feel stressed. Encourage him to try some of these stress-relieving activities if he’s also feeling the stress of pregnancy.
Bowel habits often change during pregnancy. Constipation is common and often accompanied by irregular bowel habits and hemorrhoids. These problems are usually the result of a slowdown in the movement of food through the gastrointestinal system and the ingestion of iron as supplements or in prenatal vitamins.
Two situations add to the problem of constipation in pregnancy. One is increased hormones—your body produces progesterone, which relaxes the smooth muscles of the intestinal wall and stomach, resulting in a slowdown of digestion. Second, your blood volume increases; you may not be drinking enough fluid to keep up with the increase, which can cause dehydration in you.
To help relieve the problem, increase your fluid intake. Eat foods that contain a lot of water, such as frozen juice treats, watermelon or a slush made with fresh lemon juice and water. In addition, foods with lots of fiber hold onto water longer, which helps soften your stools. For example, eating lentils or bran cereal can help increase fiber intake.
Exercise may be beneficial; try to exercise three or four times a week. It helps shift body position, which may stimulate your bowels and increase muscle contractions that help move food through your intestines.
Many healthcare providers suggest prune or apple juice or a mild laxative, such as milk of magnesia, Metamucil or Colace. However, avoid excessive use of any preparation that contains magnesium. High-fiber foods, such as bran and prunes, may help relieve constipation.
Don’t use laxatives, other than those mentioned above, without consulting your healthcare provider. Try not to strain when you have a bowel movement; straining can lead to hemorrhoids. If constipation is a continuing problem, discuss it at your next office visit.
Some pregnant women experience headaches during pregnancy. Increased hormone levels and increased blood volume can contribute to headaches. Headaches may also be caused by blood-sugar-level changes, changing hormones, dehydration or lack of sleep.
You may experience more tension headaches during pregnancy; they can be caused by many things, including stress, fatigue, heat, noise, thirst, hunger, loud music and bright lights. Some foods can trigger a headache, including peanuts, chocolate, cheese and some meats. Congested sinuses may also increase headaches. Tension headaches may decrease in the second and third trimesters of pregnancy as your body (and mind) adjust to your pregnancy.
Cluster headaches come in groups, last about an hour each time and can continue for weeks or months. Acetaminophen is OK to use for these types of headaches.
You may hesitate to take medication for headaches during pregnancy. Try any of the following medicine-free techniques for headache relief.
•Use deep-breathing exercises and relaxation techniques.
•Drink plenty of fluids so you don’t become dehydrated.
•Close your eyes and rest in a quiet place.
•Avoid foods or substances that can cause headaches.
•Apply an ice pack to the back of your head.
•Get enough sleep.
•Exercise to help relieve headaches.
•Massage your neck and shoulders to help relax tight muscles.
•Put a warm washcloth over your nose and eyes to relieve a sinus headache.
•Put a cold pack on the base of your neck.
•Massage your head/neck/shoulder area, or ask your partner to do it for you.
If your headache doesn’t go away using these techniques, you may take regular or extra-strength acetaminophen. If this doesn’t help, call your healthcare provider.
Migraine headaches are often an inherited disorder. Nearly one in five pregnant women has a migraine at some point during pregnancy. A migraine can last for a few hours up to 3 days. Some women suffer more during pregnancy because of their changing hormone levels. Be aware that a headache or migraine that doesn’t go away in late pregnancy could signal pre-eclampsia.
A migraine headache is characterized by severe, throbbing pain and is aggravated by physical activity, such as walking. Nausea, vomiting or diarrhea often accompany a migraine headache.
Some women who regularly experience migraines do not suffer from them during pregnancy; others have worse migraine headaches, especially in the first trimester. For some, the second and third trimesters are migraine-free.
You can attempt to deal with migraine headaches without medicine. Lie in a darkened room with a cold compress on your forehead. Try various relaxation methods, such as listening to relaxation tapes, doing deep-breathing exercises or practicing meditation/yoga exercises. Avoid things that might trigger a migraine, including aged cheese, cured meat, chocolate, caffeine, cigarette or cigar smoke, bright lights, stress or disruptions in sleeping or eating patterns.
Ginger may help with migraines. Studies show a pinch of powdered ginger in water may be as effective as prescription medicine. When you first feel symptoms of a migraine, mix  teaspoon of powdered ginger in a cup of water. Drink this mixture three or four times a day for 3 days for relief.
teaspoon of powdered ginger in a cup of water. Drink this mixture three or four times a day for 3 days for relief.
If the above measures don’t help, talk with your healthcare provider; he or she will prescribe the safest medication available. Do not take any medication, other than acetaminophen, for a migraine headache without discussing it first with your healthcare provider.
Other conditions can cause nausea and vomiting in early pregnancy besides morning sickness, including pancreatitis, gastroenteritis, appendicitis and pyelonephritis as well as some metabolic disorders. If you don’t have morning sickness in early pregnancy then experience nausea and vomiting later in your pregnancy, it’s not morning sickness.
Heartburn? Indigestion? Which one is it?
Some people who suffer from heartburn say they are suffering from indigestion. However, indigestion isn’t the same thing as heartburn. Although they have similar triggers and treatment may be the same in many instances, they are different.
Indigestion is a condition and refers to an inability to digest food or difficulty digesting food. It includes a vague feeling of discomfort and pain in the upper abdomen and chest, a feeling of fullness and bloating, and may be accompanied by belching and nausea.
Several things can trigger indigestion, including overeating, eating a particular food, drinking alcohol or carbonated beverages, eating too fast or too much, eating fatty or spicy foods, drinking too much caffeine, smoking or eating too much high-fiber foods. Studies show that anxiety and depression can worsen symptoms. Other causes include a duodenal ulcer or gastric ulcer and use of antibiotics, aspirin and/or NSAIDs.
If you have indigestion, you can take steps to relieve it. Eat foods that agree with you; avoid spicy foods. Eat small meals frequently. If you need antacids after meals, use them but don’t overmedicate yourself.
One of the most frequent discomforts of pregnancy, especially among older pregnant women, is heartburn. Heartburn is a burning discomfort related to the lower end of the esophagus and is felt behind the lower part of the sternum; it may be a symptom of indigestion. It occurs when your digestive tract relaxes and stomach acid creeps back into the esophagus.
Heartburn may begin early in pregnancy and often becomes more severe as pregnancy progresses. Women often want to know the difference between heartburn and indigestion.
Two main causes of heartburn during pregnancy are a reflux (backing up) of stomach acids into the esophagus and the hormonal changes of pregnancy. During pregnancy, your body produces hormones that relax involuntary muscles; one such muscle normally prevents stomach acids from backing up into the esophagus. Because the muscle isn’t doing its usual job, you experience heartburn. You may notice heartburn during the third trimester especially, when the expanding uterus crowds the stomach and intestines. This can cause some stomach contents to back up into the esophagus.
Antacids may provide considerable relief. Follow your healthcare provider’s instructions and/or package directions relating to pregnancy. Don’t overdo it and take too much in an effort to find relief. You can use some antacids, such as Amphojel, Gelusil, milk of magnesia and Maalox, without too much concern. However, avoid excessive use of any product that contains sodium or magnesium. Sodium can contribute to water retention. Excessive use of magnesium antacids has been linked to magnesium poisoning. In addition to taking antacids, try the following suggestions.
•Eat smaller meals more frequently.
•Avoid overeating.
•Use less fat when cooking.
•Avoid carbonated beverages.
•Don’t eat foods you know give you heartburn, such as rich or spicy foods.
•Avoid eating before bedtime.
•When lying down, elevate your head and shoulders.
•Wear loose clothing.
•Stay upright after meals, especially in late pregnancy.
•Chew gum for 30 minutes after meals and when heartburn strikes. Chewing gum increases saliva production, which counteracts stomach acids.
•Suck on hard candy to promote saliva production.
•Get some exercise, but don’t eat for the 2 hours before you begin. Use smooth moves to avoid pushing acids into your esophagus.
•Reduce stress in your life.
Another way to help relieve heartburn is to mix the juice of ½ lemon and a pinch of salt in 8 ounces of water, and drink it before meals. After meals, 1 teaspoon of honey may help ease discomfort.
Two popular over-the-counter medications are Pepcid AC (for acid control) and Tagamet HB (for heartburn relief). However, we advise women not to use these products during pregnancy unless there is clear indication they are needed. Don’t take these or any other medication without first discussing the situation with your healthcare provider.
Gina was having a hard time with heartburn. She loved to eat Italian food, Mexican food and spicy foods, but she paid for it. With a few modifications, she found she could eat the things she liked and not suffer from heartburn afterward. She ate earlier in the evening, at least 2 hours before going to bed. She ate smaller amounts, and she always carried antacids, such as Tums or Mylanta. She started to call her antacids “my after-dinner mints”!
GERD (gastroesophageal reflux disease) or acid-reflux disease may be mistaken for heartburn during pregnancy. It is very common but often overlooked.
How can you tell the difference? With GERD, stomach acid flows back up into the esophagus. The three most common symptoms of acid-reflux disease include heartburn, sour or bitter taste, and difficulty swallowing. Other symptoms may include persistent cough, hoarseness, upset stomach and chest pain.
Be careful with the foods you eat. Eating too much food that is spicy, highly acidic or high in fat may aggravate acid reflux.
Only your healthcare provider can determine if you have GERD, so talk to him or her at a prenatal appointment if you have concerns. He or she may prescribe medication that is safe to use during pregnancy. If you’re now taking prescription or over-the-counter medication to treat your problem, check with your healthcare provider before continuing its use.
Hemorrhoids can be an uncomfortable problem during pregnancy. Hemorrhoids are dilated blood vessels (varicose veins) of the rectum that can itch, bleed and hurt. They appear around the area of the anus or inside the anus. They are caused by decreased blood flow in the area around the uterus and pelvis because of the weight of the uterus, causing circulation blockage. Older women are especially vulnerable to developing hemorrhoids; they may have some dilated blood vessels around the rectum even before pregnancy.
Some women have the problem only during pregnancy, when body tissue changes, with some loss of elasticity. Pressure from your enlarging uterus blocks blood flow in the pelvic area. These changes encourage hemorrhoid formation.
Pregnant women most often develop hemorrhoids during the second and third trimesters. Hemorrhoids may worsen toward the end of pregnancy. They may also get worse with each succeeding pregnancy.
Eat lots of fiber, and drink lots of fluid. Stool softeners and bulk fiber products may also help. Fiber tablets, wafers or fiber products you can add to any food or drink without adding texture may also be beneficial. If you have hemorrhoids, try any or all of the following suggestions for relief.
•Rest at least 1 hour every day with your feet and hips elevated.
•Take warm baths for relief.
•Suppository medications, available without a prescription, may help.
•Stool softeners can prevent hard stools from forming; hard stools can aggravate delicate tissues.
•At work, try to arrange a time every day to take off your shoes and put up your feet.
•Apply ice packs, cold compresses or cotton balls soaked in witch hazel to the affected area.
•Don’t sit or stand for long periods.
•Over-the-counter products that contain hydrocortisone may help relieve itching and swelling. Ask your doctor about them.
•If you experience pain, acetaminophen may help relieve it.
After pregnancy, hemorrhoids usually improve, but they may not go away completely. Continue to use the treatment methods discussed above when pregnancy is over.
Discuss the situation with your healthcare provider if hemorrhoids become a major problem. In rare cases, the problem is relieved with surgery after pregnancy.
Time-Saving, Energy-Saving Tip
When you have a backache, swelling or other pregnancy discomforts, an ice pack may offer relief. If you don’t have any commercial ice packs at home, make your own! Fill a heavy-duty zipper freezer bag with 1 part rubbing alcohol to 3 parts water. Add some food coloring (blue or green are good choices) so you won’t mistake it for something else. Freeze, then use it when you need it. You can make many different sizes—as many as there are sizes of freezer bags. This enables you to cover a small or a large area.
Stretching your legs can help relieve leg cramps. Sit on the floor, and place your feet flat against the wall. Pull toes away from the wall, keeping heels on the floor. Repeat six to eight times when you experience leg cramps.
Leg cramps, also called charley horses, can be bothersome during pregnancy, especially if you experience them at night. Cramps are characterized by a sharp, grabbing pain in the calf. A cramp is a spasm in two sets of muscles that forces your foot to point involuntarily.
The best way to relieve a leg cramp is to stretch muscles. Flex or bend your foot to stretch leg muscles in the opposite direction. You can do this by standing up or by gently pressing the knee down with one hand while you gently pull the upper part of the foot toward you with your other hand. Stretching exercises before you go to bed at night may help. Don’t point your toes or stretch your legs before getting out of bed. The following suggestions may help relieve or prevent leg cramps.
•Wear maternity support hose during the day.
•Take warm (not hot) baths.
•Do stretching exercises.
•Have your partner massage your legs.
•Take acetaminophen for pain.
•Rest on your left side.
•Use a heating pad set on low for up to 15 minutes (no longer) on the cramp.
•Avoid standing for long periods of time.
•Don’t wear tight or restrictive clothing.
One study showed women who eat high amounts of saturated fat—the kind found in cheese and red meat—in the year before they got pregnant had a higher risk of suffering severe morning sickness during pregnancy.
Some medical experts believe leg cramps occur more frequently if there is an imbalance of calcium and phosphorous in the body. Don’t consume more calcium than you need—1200mg is the recommended daily dose during pregnancy. That’s about 4 cups of milk. (See also the chart on page 188 for the calcium content of some foods.) Soft drinks, snack foods and processed foods are high in phosphates; you may need to cut down on them or eliminate them from your diet. Drinking lots of water may help prevent leg cramps.
If you want to try a folk remedy, mix together 2 teaspoons of apple-cider vinegar and 1 teaspoon of honey in a glass of warm water. Drink it before bed.
An early symptom of pregnancy for many women is nausea, sometimes accompanied by vomiting, often called morning sickness. About 50% of all pregnant women experience nausea and vomiting, about 25% of pregnant women have nausea only and 25% experience no symptoms. The condition may affect you, especially if you suffer from motion sickness or migraines before pregnancy.
Morning sickness usually occurs around week 6 and lasts until week 12 or 13, when it usually starts to subside. Sometimes it can last throughout pregnancy.
The problem may be worse in the morning. Whether it occurs in the morning or later in the day, morning sickness often starts early and improves throughout the day as you become active.
Morning sickness is more common in women carrying multiples. Heart-burn and reflux can also impact morning sickness, making nausea and vomiting worse.
There is some good news about morning sickness—women with nausea and vomiting in pregnancy have a lower incidence of miscarriage. The sicker you are, the lower the chance you will miscarry.
Be aware that morning sickness can affect your pregnancy weight gain. For many women, weight gain may not begin until the beginning of the second trimester, when nausea and vomiting often pass.
Try the following suggestions to deal with the nausea and vomiting related to morning sickness.
•Eat small portions of nutritious food throughout the day instead of three large meals.
•Eat a snack, such as dry crackers or rice cakes, before you get out of bed in the morning. Or ask your partner to make some dry toast for you.
•Avoid heavy, fatty foods.
•Keep up your fluid intake—fluids may be easier to handle than solids and will help you avoid dehydration.
•Alternate wet foods with dry foods. Eat only dry foods at one meal, then wet foods and liquids at the next.
•Try fresh ginger—it’s a natural remedy for nausea. Grate it onto vegetables and other foods. Or make a tea with it.
•Avoid things that trigger your nausea, such as odors, movement or noise.
•Suck on a fresh-cut lemon when you feel nauseated.
•Get enough rest.
•Avoid getting sweaty or overheated, which can contribute to nausea.
•Apply pressure to pressure points on your wrists. (See the illustration and instructions on page 161.)
•Wear a ReliefBand. See the box below.
There is no completely successful treatment for pregnancy nausea and vomiting. Research has found that quite a few women find relief by taking vitamin B6 supplements. It’s good therapy to try because it’s readily available and inexpensive. Ask your healthcare provider about taking PremesisRx, a once-a-day tablet. If vitamin B6 alone doesn’t work, he or she might want to add doxylamine, an antihistamine.
You can also ask about taking over-the-counter antinausea medication, such as Emetrol. In addition, ask your healthcare provider about using a different prenatal vitamin that might be easier on your stomach. You might ask about taking a regular multivitamin—not a prenatal vitamin—or a folic-acid supplement during the first trimester.
A ReliefBand may help relieve morning sickness. It’s worn like a wrist watch on the inside of your wrist. It stimulates nerves in the wrist with gentle electric signals; this stimulation is believed to interfere with messages between the brain and stomach that cause nausea. It has various stimulation levels to allow you to adjust signals for maximum control for individual comfort. It can be used when nausea begins, or you can wear it before you feel ill. It doesn’t interfere with eating or drinking. It’s water resistant and shock resistant, so you can wear it just about any time!
To help relieve nausea, find the pressure point three fingers above your wrist fold. Press on the point on each wrist at the same time—you’ll probably need help doing this. Hold for 1 minute; repeat 3 times.
Acupressure, acupuncture and massage may also prove helpful when dealing with nausea and vomiting. Acupressure wristbands, worn for motion and seasickness, and other devices help some women feel better.
This is an extremely important period in the development of your baby. Don’t expose your unborn baby to herbs, over-the-counter treatments or any other “remedies” for nausea that are not known to be safe during pregnancy.
If your morning sickness is wearing you down, call your doctor’s office. Ask about different ways to deal with morning sickness. Reassurances that this situation is normal and your baby is OK can be comforting.
Nausea does not usually cause enough trouble to require medical attention. However, a condition called hyperemesis gravidarum (severe nausea and vomiting) causes a great deal of vomiting, which results in loss of nutrients and fluid. Only 1 to 2% of all pregnant women experience hyperemesis gravidarum.
If you experience severe vomiting and can’t eat or drink, you may be suffering from hyperemesis gravidarum. If you’re unable to keep down 80 ounces of fluid in 24 hours, if you lose more than 2 pounds a week or 5% of your prepregnancy weight, or if you vomit blood or bile, contact your doctor immediately!
You may need to be treated in the hospital if you become dehydrated and lose weight. You will receive fluids and electrolytes intravenously and can usually resume liquids and eating solid food after a couple of days. Hypnosis is another treatment that can be successful.
An interesting note: Studies show if you experience hyperemesis gravidarum, your chance of having a daughter increases by more than 75%. Experts believe the cause is an overabundance of female hormones produced by the fetus and mother-to-be in the first trimester.
During the last part of pregnancy, your ankles and feet may swell; some women also observe swelling in their hands and fingers. Swelling often begins around week 24. Nearly all pregnant women suffer from swollen fingers, ankles and feet.
Swelling occurs because your body produces as much as 50% more blood and fluids to meet your baby’s needs. Some of this extra fluid leaks into your body tissues. When your enlarging uterus pushes on pelvic veins, blood flow in the lower part of your body is partially blocked. This pushes fluid into your legs and feet, causing swelling.
The best way to deal with the swelling is to improve your circulation through exercise and position changes. When possible, walk short distances. Do ankle circles while standing in line or sitting in a chair. Flexing your feet and ankles during the day helps keep blood circulating. When sitting, press your toes down as if you were pushing on the gas pedal of your car to accomplish the same thing.
To deal with normal swelling in legs and feet, wear sneakers, flats or shoes with low heels (no higher than 1½ inches) that fit comfortably. Choose the right kind of shoe for you. An ideal shoe has a 1-inch heel, good arch support, a roomy, box-shaped toe and adjustable straps or laces.
Prenatal massage may help with swelling. Eat foods high in potassium; a potassium deficiency may allow your cells to fill with water, increasing swelling. You can also try standing on your tiptoes—it helps pump blood back to the heart.
If swelling becomes extreme, especially during the last trimester, consult your healthcare provider; it could be a sign of problems. Lie on your left side as frequently as possible. Don’t stand for long periods.
Time-Saving, Energy-Saving Tip
If your hands swell so much you can’t wear rings, put your rings on a pretty chain and wear them around your neck or wrist.
Many women experience an occasional excruciating pain in their buttocks and down the back or side of their legs as pregnancy progresses. It is called sciatic-nerve pain or sciatica. The sciatic nerve is located behind the uterus, in the pelvic area, and runs down into the leg. We believe pain is caused when the enlarging uterus puts pressure on the nerve.
The best treatment is to lie on your opposite side to help relieve pressure on the nerve. Sitting on a tennis ball on a hard surface may also help. If you have to stand for any length of time, rest the toes of one foot on some object that is 3 to 4 inches off the ground, such as a thick book (the phone book or a dictionary works great!) to relieve pressure on the sciatic nerve.
Some people may mistakenly refer to sciatic-nerve pain as sacroiliac pain. However, sciatica pain and sacroiliac pain are not the same thing. Sciatica is a sharp, searing pain. Sacroiliac joint pain (SJP) is joint related and feels like a sharp jolt of pain on either side of the back or hips. It may extend down your legs. Warm baths (not hot) and acetaminophen may help.
Are you having trouble sleeping? Nearly 80% of all pregnant women have trouble sleeping at some time during pregnancy. Some reasons include hormone changes, altered respiration and the increased size of the abdomen. A short nap during the day may pep you up and help make up for sleep lost during the night.
Many moms-to-be wake up five or more times a night, which can cause fatigue during the day. Baby’s movements, leg cramps and shortness of breath may also keep you up during the night later in pregnancy. You need to get enough rest during the night, especially late in pregnancy. Research shows women who slept fewer than 6 hours at night were four times more likely to have a Cesarean delivery.
Varicose veins, also called varicosities or varices, are large, distended veins deep under the skin. They are caused by problems with the one-way circulatory valves inside veins. Valves become clogged with blood then grow larger, which keeps blood from flowing through the vein as it should.
Tips for Getting a Good Night’s Sleep
•Go to bed and wake up at the same times each day.
•Don’t drink too much fluid at night. Decrease fluid intake after 6pm.
•Avoid caffeine after late afternoon.
•Get regular exercise.
•Sleep in a cool bedroom; 70F (21.1C) is the maximum temperature for comfortable sleeping.
•If you experience heartburn at night, sleep propped up.
They occur to some degree in most pregnant women; however, varicose veins develop more often in older women. There seems to be an inherited predisposition to varicose veins that can become more severe during pregnancy. If your mother had varicose veins, you are more likely to develop them.
Varicose veins usually occur in the legs but can also be found in the birth canal or vulva. Hemorrhoids are varicose veins. Pressure from the uterus and the change in blood flow during pregnancy can make varices worse. Varicose veins in the legs, birth canal, vulva or rectum (hemorrhoids) can cause pain and discomfort.
Symptoms vary; for some women varicose veins are only a blemish or purple-blue spot on the legs, causing little or no discomfort except in the evening. For other women, varices are bulging veins that require elevation at the end of the day or other measures. They can cause itching and aching in the affected area.
You may also experience spider veins. They are small groups of dilated blood vessels near the skin surface. You see them most commonly on face and legs.
Varicose veins may get worse during pregnancy. Increasing weight (from the growing baby, uterus and placenta), tight clothing that constricts at the waist or legs, and standing a great deal can worsen varicose veins. If you continue to have problems with varicose veins after pregnancy, you may need surgery.
The most effective way to prevent varicose veins is to improve circulation in your legs, especially through exercise and changes in position. Exercising regularly helps improve blood flow through the veins. Walk when possible, and do ankle circles while sitting and standing. Even sitting and rocking in a rocking chair can help—rocking contracts and relaxes leg muscles, which moves blood from your feet to your heart.
When you lie down, lie on your left side to improve blood flow. Elevate your hips and legs. Keep your total pregnancy weight gain within normal range—between 25 and 35 pounds for a normal-weight woman.
Drinking citrus juice or eating citrus fruit may help with varicose veins. The vitamin C helps keep capillary and vein walls strong. Eating spinach, broccoli and asparagus may help lessen the severity of varicose veins. These foods are high in vitamin K, which helps activate a protein that impedes the mechanism that can lead to vein distortion.
If you get varicose veins during pregnancy, ask your healthcare provider about wearing medical support hose to reduce swelling and ease leg pains. Many types of maternity support hose or graduated-compression stockings are available. Maternity support hose help many women, but they can be very difficult to get on. The following tricks can help.
Put on your support hose before you get out of bed in the morning—your legs may tend to swell as soon as you get up. (You may need to change your habits and bathe before you go to bed.) Turn the stockings inside out before you put them on. Starting at the toe, unroll the stockings up your leg.
Choose clothes that don’t restrict circulation at the knee or groin. Wear loose panties to help prevent vulvar varicosities (varicose veins in the vulva area) from causing discomfort.
Spend as little time as possible on your feet. Wear flat shoes. Don’t cross your legs at the knee, and don’t stand for long periods. If you must stand, bounce gently on the balls of your feet every few minutes.
Some women notice changes in their vision during pregnancy. If you experience vision changes or problems during pregnancy, talk to your healthcare provider. If you notice your contact lenses don’t seem to fit as well, your corneas may be swollen from fluid retention. Unless perfect vision is necessary for your work, wait to get a new prescription. Your eyes should return to normal after pregnancy.