1
Anatomy of the Pelvis and the Sacroiliac Joint
The pelvic girdle is composed of the sacrum, the coccyx, and the three so-called “hipbones”—the ilium, ischium, and pubis. The bones of the adult pelvis join together to form four joints: the left and right sacroiliac joints (SIJs), the sacrococcygeal joint, and the symphysis pubis joint (SPJ), as shown in Figure 1.1.
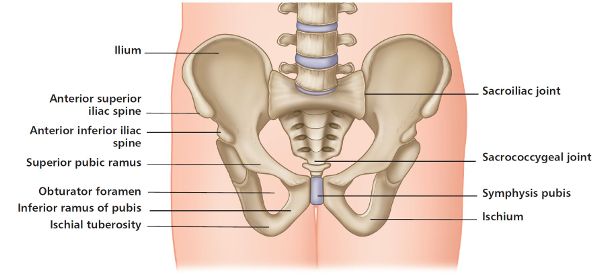
Figure 1.1. Bones of the pelvic girdle, forming the four joints.
At birth the ilium, ischium, and pubis bones are separated by hyaline cartilage; by the end of puberty these bones will have naturally conjoined (fused together), with complete ossification normally occurring by the time a person has reached the age of approximately 20–25. The three bones, once fusion has taken place, are collectively called the innominate bone, or simply the innominate. On the lateral side of the innominate bone is the acetabulum; this area forms the articulation with the head of the femur to create the iliofemoral (hip) joint, as shown in Figure 1.2.
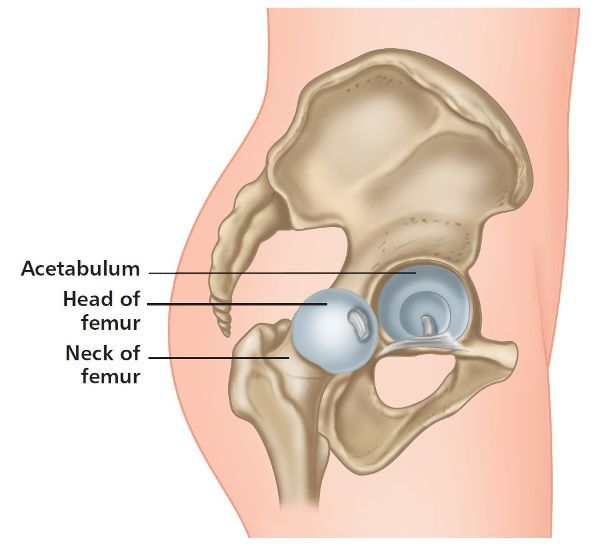
Figure 1.2. Iliofemoral (hip) joint.
Innominate Bones
Ilium
The ilium is fan shaped and is the most superior as well as the largest of the three hipbones; it makes up approximately two-fifths of the deep, cuplike socket of the hip joint, called the acetabulum. The body of the ilium together with the sacrum forms the SIJ. This L-shaped articulation is located on the posterior superior aspect of the ilium and has a vertically (vertical plane) orientated “short arm” and a more horizontally (anterioposterior plane) positioned “long arm,” as shown in Figure 1.3.
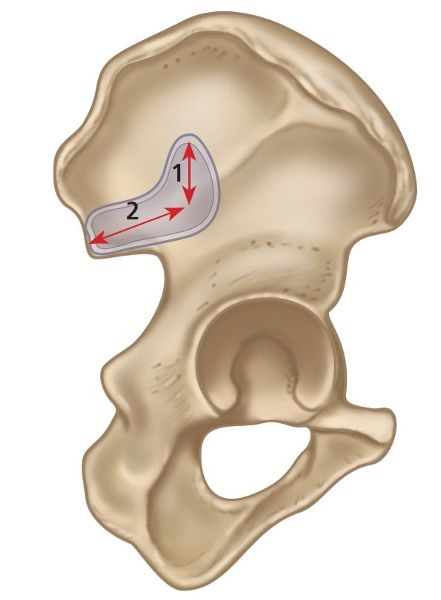
Figure 1.3. L shape of the short (vertical [1]) and long (horizontal [2]) arms of the ilium.
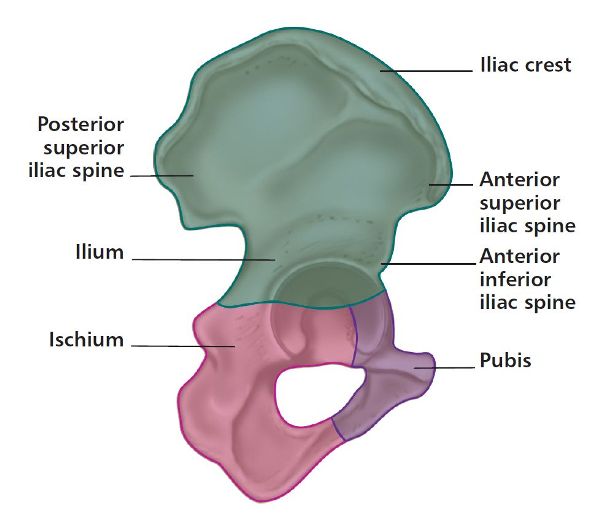
Figure 1.4. Anatomical landmarks of the iliac crest: ASIS, AIIS, and PSIS.
If you place one hand on your hip, you can feel the curved ridge of the superior aspect of the ilium: this is known as the iliac crest. From this crest, if you lightly move your fingers down inferior to the anterior aspect of the ilium, you should feel a bony projection known as the anterior superior iliac spine (ASIS); this area allows the attachment of soft tissues (e.g. the sartorius muscle). If you continue slightly inferior to the ASIS, you will come to another bony landmark called the anterior inferior iliac spine (AIIS); this is where one part of the rectus femoris muscle attaches. Palpating the posterior aspect of the ilium as it curves inferiorly, you will feel the bony prominence of the posterior superior iliac spine (PSIS); again this is an attachment for soft tissues. These two bony projections (ASIS and PSIS) are commonly used as palpatory landmarks, as shown in Figure 1.4, when one is assessing the position of the pelvic girdle.
Ischium
The ischium is narrower than the ilium bone and is located inferior to the ilium and behind the pubis. The ischium has an easily palpable landmark called the ischial tuberosity, as shown in Figure 1.5; it is commonly called the sit bone and provides the necessary landmark for the attachment of the hamstrings. It is this part of the ischium (tuberosity), along with the coccyx, on which you rest your body weight while adopting a sitting position. The ischium is the strongest of the three bones and forms approximately two-fifths of the acetabulum (hip socket).

Figure 1.5. Ischium and ischial tuberosity.
Pubis
The pubis, or pubic bone, is the most anterior as well as the smallest of all the three hipbones and makes up approximately one-fifth of the acetabulum. The body of the pubis is wide, strong, and flat, and together with the opposite pubic bone makes up the SPJ. This joint is classified as an amphiarthrosis, as it is connected centrally by a broad piece of fibrocartilage, as shown in Figure 1.6. On the superior aspect of the pubis there is a bony projection called the pubic tubercle; this structure allows the attachment of the inguinal ligament and is also used as a palpatory landmark when one is assessing the position of the pelvic girdle.

Figure 1.6. Pubis, pubic tubercle and SPJ.
Sacrum
The sacrum (sacred bone) is a large triangular bone located at the base of the lumbar spine and forms the back part of the pelvic cavity. The sacrum starts out from birth as five individual bones before starting to fuse between the ages of 16 and 18; the sacrum is considered to have fully fused into a single bone by the time you have reached 34 years of age.
Considerable differences in the shape of the sacrum between individuals, as well as structural differences between the left and right sides, are well documented. The connection of the sacrum to the ilium forms the SIJ.
The superior aspect of the sacrum is called the sacral base and is primarily made up of the 1st sacral segment; the base is angled in a forward direction to form a concavity. The opposite end of the sacrum is called the sacral apex and this is made up of the 5th sacral segment, as shown in Figure 1.7. The natural position of the sacrum is called the sacral angle and is generally thought to be in the range 40–44 degrees (Figure 1.8), although, as discussed by some authors, the angle can be anywhere from 30 to 50 degrees. Moreover, a specific type of motion called nutation (a nodding motion, which will be discussed later) can be responsible for an increase in this angle by anywhere between 6 and 8 degrees on standing up (from a sitting position). The sacral angle increases because of the change in the curvature of the lumbar spine, from an initial flexion curvature when sitting, to an extension curvature (lumbar lordosis) when standing, as one performs the motion from a sitting to a standing posture. This sacral movement allows the whole of the spinal column to adopt an upright position.
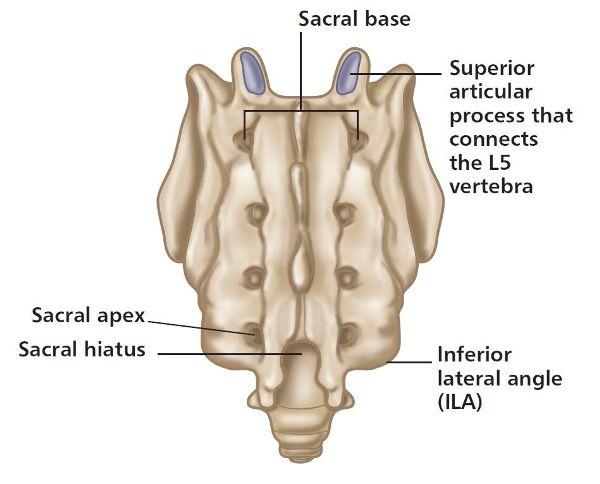
Figure 1.7. Anatomical landmarks of the sacrum (posterior view).
On the lateral sides of the sacrum located between the levels of the first three sacral vertebra (S1–S3) are the alae (wings): these auricular (earlike) L-shaped areas of the sacrum make up the articulation with the ilium—i.e. the SIJ. In an earlier paragraph regarding the ilium I mentioned that there is a short vertical arm and a long anteroposterior (horizontal) arm, as shown in Figure 1.8, which will naturally dovetail with each other, like pieces of a jigsaw puzzle.

Figure 1.8. The short (vertical [1]) and long (horizontal [2]) arm of the sacrum, and the sacral angle (lateral view).
Another way of looking at the sacrum is as a continuation of the lumbar spine, while the SIJs on either side are mimicking what I generally call atypical facet joints. You can think of the sacrum as a single vertebra, and the left and right SIJs as the articulating facet joints, with the superior articular facet being the ilia component and the inferior articular facet being the sacral component (illustrated in Figure 1.11).
Coccyx
The coccyx is the continuation and endpoint of the vertebral column and is commonly referred to as the tailbone. It has between three and five (normally four) vertebral segments called the coccygeal vertebrae, and most textbooks state that these are actually fused; some authors, however, maintain that the coccygeal vertebrae are indeed separate and individual entities (Figure 1.9).
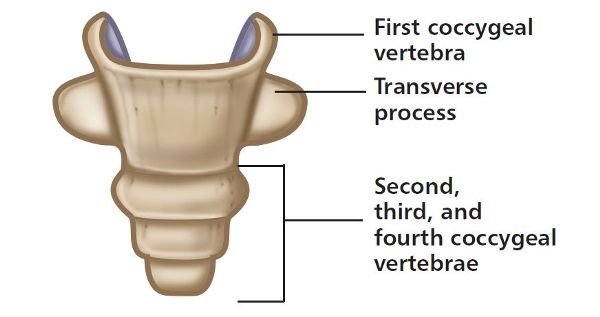
Figure 1.9. Coccyx bone and the individual segments.
There are many muscles with attachments directly on the coccyx: for example, the pelvic floor muscles attach to the anterior surface of the coccyx, and the gluteus maximus (Gmax) muscle and ligaments attach to the posterior surface. Likewise, some ligaments attach directly to the coccyx, such as the sacrococcygeal ligament and some of the fibers of the sacrospinous and sacrotuberous ligaments. The coccyx also plays a role in weight bearing (while sitting), as it forms part of the tripod structure, working in conjunction with the left and right ischial tuberosities (sit bones).
Symphysis Pubis Joint
The symphysis pubis joint (SPJ) is classified as a non-synovial fibrocartilaginous amphiar-throsis, connecting the left and right pubic bones.
In adults only 0.08” (2mm) of movement (shift) and one degree of rotation are considered to be possible in this joint; however, these values will increase in women during pregnancy and childbirth. The available movement of the SPJ is also influenced by the natural shape of the joint, and by muscular activation from the adductor and abdominal muscles.
The ends of each pubic bone are covered by hyaline cartilage that connects to the piece of fibrocartilage located in the center of the SPJ. The joint has strong superior and inferior ligaments and a thinner posterior ligament (Figure 1.10).
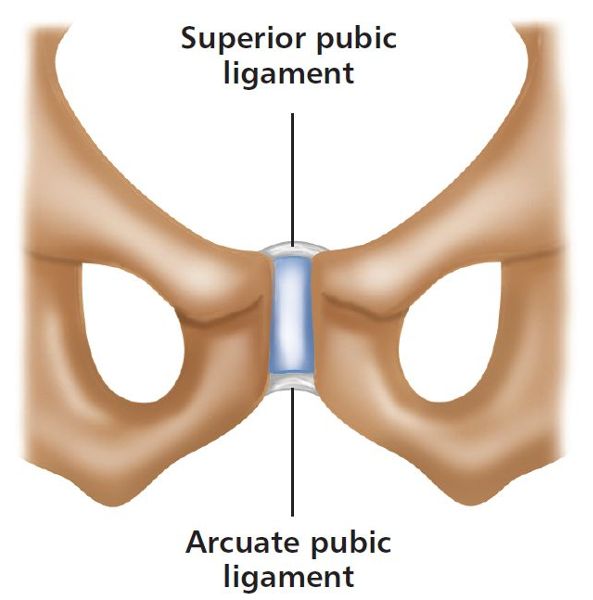
Figure 1.10. Symphysis pubis joint and associated ligaments.
One can think of the design of the symphysis pubis as being similar to the intervertebral discs of the spine, with a central disc of fibrocartilage that cushions against compressive loads, as well as providing shock absorption and contributing to passive stabilization. Because of this similarity, the articular disc of the SPJ is also vulnerable to both degeneration and trauma, particularly when the joint is subjected to traumatic or repetitive shear forces (e.g. osteitis pubis).
Functionally, the SPJ helps to resist tension, shearing, and compression forces, and remarkably is able to widen during pregnancy. The anatomist Andreas Vesalius, who challenged the Hippocratic belief that the pubic bones separated during childbirth, was the first to recognize this joint in 1543.
Sacroiliac Joint
Lower back pain and the link with the sacroiliac joint (SIJ, or SI joint) date back to the era of Hippocrates (c.460–377 BC); the medical practitioners (obstetricians) at the time felt that under normal conditions the SIJs were immobile. I am very pleased to say that things have progressed enormously over the last few decades with all the information now readily available in respect of the general consensus of the role and function of the pelvic girdle, and in particular of the SIJ. I can guarantee, though, that over time some things will nevertheless change, so this book may well need to be updated in the future.
I have been lecturing courses on the pelvic girdle, and on the SIJ in particular, for many years at my venue based at the University of Oxford, which means I have come into contact with thousands of physical therapists, ranging from osteopaths and physiotherapists to chiropractors and lots of sports therapists, to mention but a few. If I am honest with myself, I personally consider that the area of the pelvis is a relatively difficult subject to try to get across to my students (mainly therapists); this is because I consider the SIJ to be something of a “mystery” to many therapists, and it becomes especially difficult when I am trying to explain the subject matter to my athletes and patients.
The majority of physical therapists attending the course on the pelvic girdle tell me at some point that they see patients and athletes on a daily basis with what they consider to be a presentation of sacroiliac joint dysfunction. In the past, patients with presenting SIJ issues have even been referred directly to them by the local GP or a colleague.
Vleeming et al. (2007) say that mobility of the pelvic joints is difficult to measure objectively, especially in the weight bearing position, and that feeling motion at the sacroiliac joint during active and passive motion is difficult to prove.
Bearing in mind the above quote, you can imagine that teaching a specific course on this fascinating but undoubtedly complex area of the body is not as straightforward as one might think.
Anatomy
The SIJ, as shown in Figure 1.11, is located between the sacrum and the ilium and is classified as a true synovial arthrodial joint, as it contains a joint capsule, synovial fluid, articular cartilage, and a synovial membrane.
The SIJ is unique: on the ilia side, the cartilage is made up mainly of fibrocartilage, whereas on the sacral side, the cartilage consists of hyaline, or articular, cartilage. The articular (hyaline) cartilage is thicker (0.04–0.12”, or 1–3mm) on the sacral side than on the ilia side. Kampen and Tillman (1998) found that in adults the cartilage on the sacral surface of the joint can reach 0.16” (4mm) in thickness, but does not exceed 0.04–0.08” (1–2mm) on the iliac surface. The lack of thickness of the cartilage on the ilia side might be one of the factors responsible for hardening (sclerosis).
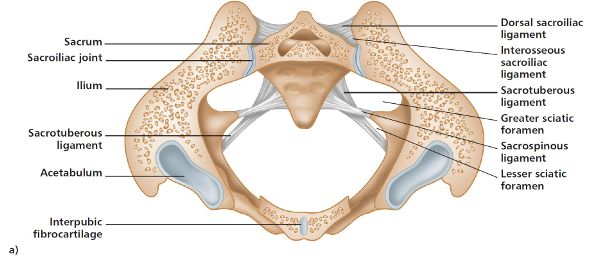
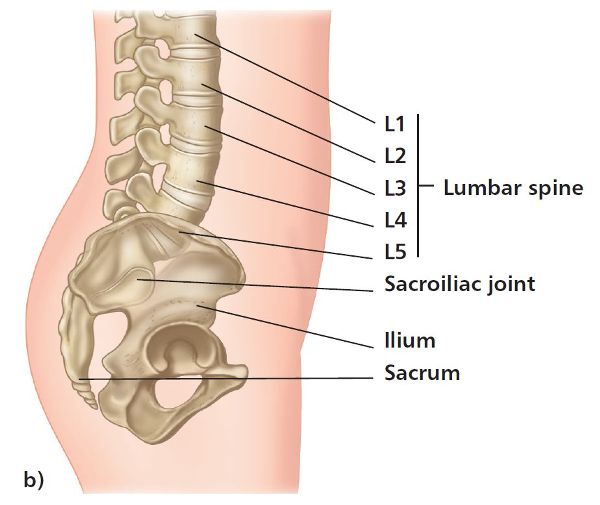
Figure 1.11. Anatomy of the SIJ; a) transverse section; b) lateral view.
The SIJs have an auricular L-shaped appearance, similar to a kidney, with a short (vertical) upper arm and a longer (horizontal) lower arm (as already mentioned earlier).
Regarding the shape of the SIJ, different characteristics between individuals have been clinically proven; moreover, there can be significant structural differences between the left and right sides of the joint surfaces within the SIJs of the same individual. There is also clear evidence of the fact that the paired SIJs, and even the PSISs, are generally asymmetric in appearance, which can also be the case in patients and athletes who present with no symptoms of pain or dysfunction (i.e. are asymptomatic).
In terms of motion, the pelvis is capable of moving in all three planes of the body: flexion and extension in the sagittal plane (forward and backward bending); lateral flexion (side bending) in the frontal plane; and rotation of the trunk in the transverse plane. It has been debated that the SIJ can move anywhere between 2 and 18 degrees, but more recent evidence provided by many clinicians demonstrates that there are roughly 2–4 degrees of rotation and 0.04–0.08” (1–2mm) of translation. Studies have shown us that movement is possible, but only in very small amounts; this was demonstrated by Egund et al. (1978) and Sturesson et al. (1989, 2000a, 2000b), who found the motion of the SIJ to be at best approximately 2–4 degrees in rotation and 0.08” (2mm) in translation.
We know that when we are developing through the natural aging process, the SIJ characteristics change. In early life the SIJ surfaces are in general initially flat, but as we start to walk and progress through puberty, these surfaces develop distinct ridges and grooves and lose their naturally flattened appearance. These ridges and grooves actually fit into one another to some extent; this will potentially aid the overall stability of the SIJ, while still allowing some degree of movement.
The text Greenman’s Principles of Manual Medicine (DeStefano 2011) mentions that “during the aging process, there is an increase in the grooves on the opposing surfaces of the sacrum and ilium that appears to reduce available motion and enhance stability.” The author also says that “it is of interest to note that the age at which the incidence of disabling back pain is highest (range: 25 to 45 years) is the same age when the greatest amount of motion is available in the sacroiliac joints.”
Because of the relationship of the three main pelvic joints (the two sacroiliac and the symphysis pubis), as well as their relationship to the iliofemoral joint (hip joint), a dysfunction existing in any one of these joints can have a direct impact on the other two/three joints.
Ligaments of the SIJ
The SIJ has very strong ligaments, which increase the joint’s stability and make potential dislocations very rare.
Stability of the SIJ is provided partly through ligamentous attachments. These specific ligaments will provide joint integrity as well as resistance to shearing-type forces. The ligaments that bind the sacrum directly to the innominate are (Figure 1.12):
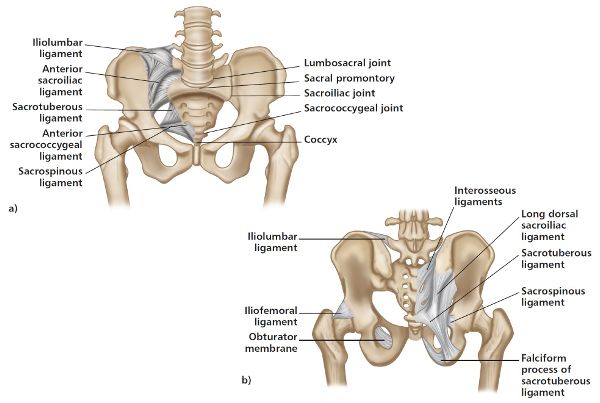
Figure 1.12. Ligaments relating to stability of the SIJ; a) anterior view, b) posterior view.
The iliolumbar ligament will also have a stabilizing influence on the SIJ as well as on the lumbar spine.
Sacrotuberous Ligament
The sacrotuberous ligament attaches from the PSIS and also has an attachment to the posterior sacroiliac ligaments. The ligament then continues and attaches onto the ischial tuberosity and splits into three individual bands: the outer (lateral) side attaches from the PSIS to the ischial tuberosity; the inner (medial) band attaches from the coccyx to the ischial tuberosity; and the superior band connects the PSIS to the coccyx.
Four muscles have an attachment directly to the sacrotuberous ligament and will contribute to the overall stability of the SIJ:
• Biceps femoris
• Gluteus maximus (Gmax)
• Multifidus
• Piriformis
Vleeming et al. (1989a) found that in approximately 50% of subjects the lower border of the sacrotuberous ligament was directly continuous with the tendon of the origin of the long head of biceps femoris; this muscle could therefore act to stabilize the SIJ via the sacrotuberous ligament.
Part of the role of the sacrotuberous ligament is to resist the anterior nodding type of motion of the sacrum known as nutation. This ligament will also prevent posterior rotation of the innominate bone with respect to the sacrum. If for some reason there is laxity in the sacrotuberous ligament (along with the sacrospinous ligament), the decreased tension can result in a posterior rotation of the innominate bone, and also lead to increased nutation of the sacrum.
Sacrospinous Ligament
The sacrospinous ligament has an attachment from the lateral aspect of the sacrum and coccyx and attaches to the spine of the ischium, appropriately named the ischial spine. The ligament has the appearance of a thin triangle and, together with the sacrotuberous ligament, it modifies the greater sciatic notch in the greater sciatic foramen. In one respect, the function of the sacrospinous ligament is similar to that of the sacrotuberous ligament: it prevents posterior rotation of the innominate bone relative to the sacrum, and also limits nutation (forward motion) of the sacrum relative to the innominate bone.
Interosseous Ligament
The interosseous ligament consists of a dense, short, thick collection of strong collagenous fibers that run in a horizontal plane and connect the sacral tuberosities of the sacrum to the ilium. This ligament lies deep in the narrow recess between the sacrum and the ilium, and has deep and superficial components to it. The main function of the interosseous ligament is to prevent a separation or abduction of the SIJ by strongly binding the sacrum to the ilium, as this will help secure the SIJ interlocking mechanism.
Long Dorsal Ligament (Posterior Sacroiliac Ligament)
The long dorsal ligament attaches from the medial and lateral crests of the sacrum and to the PSIS. There is also a connection of this ligament to the thoracolumbar fascia, as well as to the multifidus and erector spinae muscles.
The long dorsal ligament mainly resists counter-nutation of the sacrum (posterior nutation) as well as anterior rotation of the innominate bone. Consequently, this ligament will naturally slacken when the sacrum is in a state of nutation and/or if there is posterior rotation of the innominate bone.
If sacral torsion is present (discussed in later chapters) and the sacral base is found to be “posterior,” this ligament will be under constant tension and may be tender when palpated.
Lee (2004, p. 22) mentions that the skin overlying the long dorsal sacroiliac ligament is a frequent area of pain in patients with lumbosacral and pelvic girdle dysfunction, and that tenderness on palpation of the ligament does not necessarily incriminate this tissue, given the nature of pain referral from both the lumbar spine and the SIJ.
Iliolumbar Ligament
The iliolumbar ligament is a very strong ligamentous structure; it attaches from the transverse processes (TPs) of the 4th and 5th lumbar vertebrae and travels to the inner border of the ilium.
This ligament, which has five individual bands, is one of three vertebrae–pelvis ligaments responsible for stabilizing the lumbosacral spine in the pelvis, along with the two mentioned already, namely the sacrospinous and sacrotuberous. The main function of the iliolumbar ligament is essentially to limit the motion of the lumbosacral junction by stabilizing the connection between the pelvis and the lower lumbar vertebrae (L4 and L5).
Function of the SIJs
The SIJs’ primary responsibility is to transfer the weight of the upper body to the lower extremities. The body weight is transferred through the vertebral column to the lumbar spine (L5), to the sacrum and across the SIJs to the ischial tuberosities, and then out to the acetabula of the hip joints. This mechanism of bony attachments demonstrates the SIJs’ role as weight-bearing joints, as shown in Figure 1.13. The SIJs are also able to transfer the forces in the opposite direction when one is walking, standing, or sitting: the pressure is directed through the legs to the innominates and the sacrum, and then dissipated upward through the lumbosacral junction.
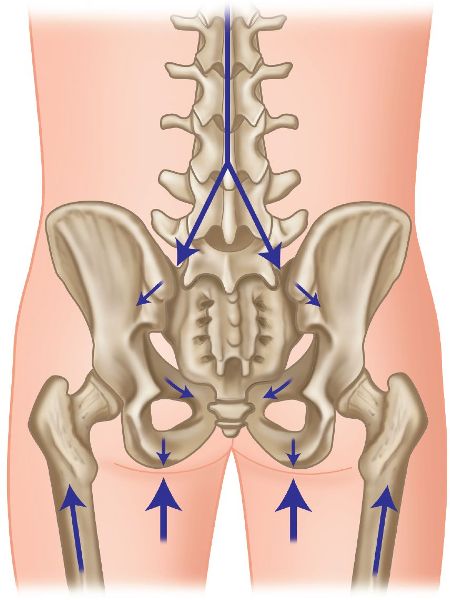
Figure 1.13. Weight transfer forces through the pelvis and the SIJs.
In their secondary role, the SIJs can be thought of as shock absorbers (mainly at the point of heel contact), as they help cushion the increased stress that is forced upon the lumbar spine and in particular upon the lower lumbar intervertebral discs. Authors in the past have suggested that the incidence of lower lumbar disc disease/degeneration increases when the SIJs present with pathological changes.
Lee and Vleeming (2007) discussed the analysis of gait mechanics and demonstrated that the SIJs provide sufficient flexibility for the intra-pelvic forces to be transferred effectively to and from the lumbar spine and lower extremities.