8
The Hip Joint and Its Relationship to the Pelvis
Almost every time I give a lecture on the areas of the pelvic girdle, hip, and groin, or even on the knee and ankle joint complex, I always hear myself saying the following to my students:
“If one has an underlying pathology within the complexity of the hip joint, then this will eventually become a potential site for pain and dysfunction in distant sites of the body, especially in certain areas of the pelvis and lower back, and even in the knee joint and lower limb.”
After saying this I tend to remind the students of the famous words of Dr. Ida Rolf:
“Where the pain is, the problem is not.”
This chapter will hopefully highlight those wise words of Dr. Rolf, which relate to not focusing our treatment where the pain is (i.e. the patient’s presenting symptoms). We as physical therapists (who I call “detectives of therapy”) should try to isolate the underlying cause of a patient’s presenting pain and try not to simply “rub where it hurts.”
I have seen a great many patients who have presented to the clinic with what has been defined or classified as the typical presentation of SIJ pain, mainly because the presenting pain is located in this particular area of the pelvis. At my sports injury and back pain clinic at the University of Oxford, I must have seen thousands of patients presenting with ongoing pain in the lumbar spine, lateral hip, groin, buttocks, adductor muscles, and hamstring muscles, as well as in the knee joint and lower limb; the underlying cause of their pain, however, is to be found in a completely different structure/tissue/source than the area of the body that suffers the pain.
Now when you read this, I don’t want you to jump to any conclusions on the basis of what I have just said. I am not saying that every time your patient presents with pain somewhere in their body the primary cause of their symptoms relates to this specific chapter about the hip joint. However, occasionally it may well be that some underlying pathology located within the hip joint complex is actually the key to unlocking the patient’s presenting symptoms. The focus of this chapter is naturally biased toward the hip joint, so the extra knowledge you will gain from reading it will potentially provide some of the answers to the questions you might have been asking yourself about your own patients, or even about some of the issues regarding your own presenting symptoms.
This chapter in itself will hopefully guide you along the right pathway. The extra information you will gain through reading it should at least assist you in providing the correct management strategy for your patients: this can be through either treating using manual therapy techniques or possibly even giving you the confidence to refer patients to a specialist for a second opinion.
The assessment processes that I will be demonstrating below will help you formulate an accurate hypothesis of what might be the underlying causative factor responsible for maintaining your patient’s presenting symptoms. That is why I always like to “screen” the hip joints of almost every patient who walks through the clinic door—I personally want to make sure that there are no underlying pathological changes within this joint, especially when patients present with pain located in the areas of the pelvic girdle, lumbar spine, knee joint, and so on.
Hip Joint Anatomy
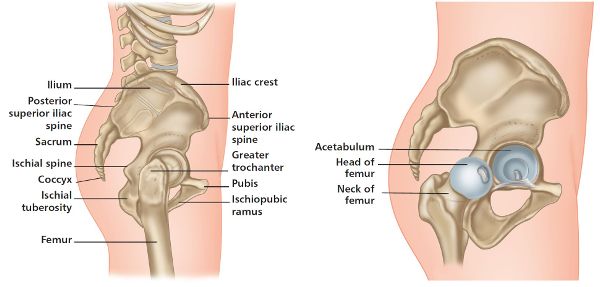
As I am sure you are aware, the hip joint (iliofemoral joint) is classified as a synovial ball and socket joint. This joint consists of the head of the femur articulating with the socket (acetabulum) of the pelvic girdle, which is made up of three bones—the ilium, ischium, and pubis. Because of the multiaxial motion that is possible at the hip joint, it will not come as a surprise that it is one of the most mobile joints of the body. Given its inherent architecture of a deep acetabulum (socket), however, the joint has a great deal of stability as well as mobility (Figure 8.1).
The motion possible at the hip joint can vary between individuals, but the normal ranges are:
• flexion: 0–130 degrees
• extension: 0–30 degrees
• internal rotation: 0–35 degrees
• external rotation: 0–45 degrees
• abduction: 0–45 degrees
• adduction: 0–25 degrees
As already explained in previous chapters, the pelvic girdle is capable of anterior and posterior rotation/tilt, while at the same time the lumbar spine is either flexing or extending. All pelvic girdle rotations/tilts/motions actually result from motion at one or more locations—the left hip, the right hip, or the lumbar spine. It is not essential for movement to occur in all three of these areas; however, motion must exist in one of them for the pelvis to rotate.
Table 8.1 highlights specific motion at the pelvic girdle and the associated motions of the lumbar spine and hip joints.
| Pelvic motion/rotation | Lumbar spine motion | Right hip motion | Left hip motion |
|---|---|---|---|
|
Anterior tilt |
Extension |
Flexion |
Flexion |
|
Posterior tilt |
Flexion |
Extension |
Extension |
|
Left lateral shift |
Left side bending |
Abduction |
Adduction |
|
Right lateral shift |
Right side bending |
Adduction |
Abduction |
|
Left transverse rotation |
Right transverse rotation |
External rotation |
Internal rotation |
|
Right transverse rotation |
Left transverse rotation |
Internal rotation |
External rotation |
Table 8.1. Pelvic, hip, and lumbar motion guidelines.
Screening the Hip Joint
With regard to screening, or assessing, the hip joint, I tend to have a few simple diagnostic tests that will either confirm or discount the presence of associated pathology within the joint:
1. Passive ROM for external rotation
2. Passive ROM for internal rotation
3. Passive ROM for flexion
4. Quadrant test
5. FABER test
6. FAIR test
7. Thomas test and modified Thomas test
These tests are simply used as guidelines in screening for any underlying pathology that might be associated with the hip joint. Remember, this book is all about the pelvis, not about the hip joint. Nevertheless, one needs to make sure that the hip joint in itself is not responsible, or even partly responsible, for dysfunction and pain in the pelvic girdle or lumbar spine regions. The tests I will be demonstrating for the hip joint are taken from my own experiences of treating thousands of patients, so much so that I have included some of my own thoughts on the way one might apply some of the tests. There are numerous other tests that can be used to screen the hip joint, but that will be the choice of the therapist at that time in their own clinic with their own patients; as I have said already, the tests I am demonstrating here have been selected on the basis of my own personal experience and preferences.
The specific passive ROM tests given in this chapter for screening the hip joints for pathology are used in particular for identifying the awareness one would feel through one’s hands at the end range of the joint that is being tested; this technique is called the joint end feel. The end feel of a joint is basically the quality of movement that is perceived by the therapist at the very end of the available ROM. The joint end feel can reveal a great deal about the nature of various pathologies located within the joint that is being tested.
There are four common classifications of what is considered to be a “normal” joint end feel (or joint end range) and which are typically present within any synovial joint:
• Soft end feel, e.g. knee flexion
• Hard end feel, e.g. elbow extension
• Muscular end feel, e.g. hip flexion (hamstrings)
• Capsular end feel, e.g. external rotation of the shoulder joint
When you are assessing your patients/athletes, and especially when you are performing the passive ROM tests, you may experience (through your hands) a different type of joint end feel to what has already been described as a “normal end feel.” In this case you can assume that there is what is called a pathological end feel present within the architecture of the joint; this positive test should be noted down, and further investigation, or even a referral to a specialist, might subsequently be necessary.
Please remember that patients have two legs and one should perform a comparison between the two, just to make sure that an actual pathology is indeed present. For example, if you passively take the patient’s left hip into full flexion, with a range of at least 130 degrees being achieved with no pain or stiffness, and your patient is comfortable at the end of the available range, then one can assume that this movement is normal and no pathology is present. Suppose, on the other hand, only around 110 degrees of flexion or less can be achieved when the same movement (flexion) is performed on the right hip, and the end range of the joint also becomes particularly painful and/or feels restrictive to your patient (especially in the groin area); in addition, you perceive a “harder end feel” during the movement. From these findings, you can safely say that the ROM of the right hip is not normal; moreover, because of the restrictive/painful barrier, the end feel would be classified as pathological, meaning that the test is positive and further investigation is required.
Just a word of caution: in the past I have assessed relatively young patients who have actually demonstrated restrictions in some of the passive ROM tests for both of their hip joints; however, because the motion and the ROM are the same on both sides, we would still regard this movement as being normal in terms of ROM.
Another thing to consider when a hip joint has restricted internal/external rotation is the possibility that this is caused by a pelvic dysfunction. For instance, suppose a patient has a right anterior innominate rotation (the most common dysfunction): internal rotation of the right hip will usually be limited, compared with the left side, and external rotation of the left hip will be limited, compared with the right side. If the patient has a suspected left anterior innominate rotation, the opposite will be found: a left internal rotation restriction and a right external rotation restriction.
Rotational restrictions of the hip joint can occur when pelvic dysfunctions are present, even though the total passive ROM in internal/external rotation for each hip joint will be very similar. What I mean by that is the following. Take the case of a patient presenting with the most common malalignment syndrome of a right anterior innominate rotation, with a compensatory left posterior innominate rotation. Because of the pelvic malalignment, the right hip is restricted to, say, only 25 degrees (35 degrees is classified as normal) on testing passive internal rotation, and it has an increased range of 55 degrees (45 degrees is classified as normal) on testing passive external rotation; this gives a total ROM of 80 degrees. The left hip, however, demonstrates an increased range of 55 degrees for internal rotation, but a limited range of only 25 degrees for external rotation, thus also giving a total ROM of 80 degrees.
The discrepancy between the two hip joints on passive testing arises mainly because of the altered malalignment position of the right and left innominate bones, which has a direct relationship to the position of the adjacent hip joint. Because of this relationship, a change in the position of the innominate bone will have a direct effect on the position of the corresponding acetabulum (hip).
On realignment of the pelvis, one usually finds an improvement in ROM to the extent that the findings for the rotational components for both the left and right hips are normal/equal, even if the total ROM remains the same (i.e. 80 degrees in this case). Pelvic corrections can, however, be very effective in improving overall hip ROM, provided there are no underlying structural pathologies present within the hip joint (corrections for pelvic girdle dysfunctions are explained in Chapter 13).
1. Passive ROM for External Rotation
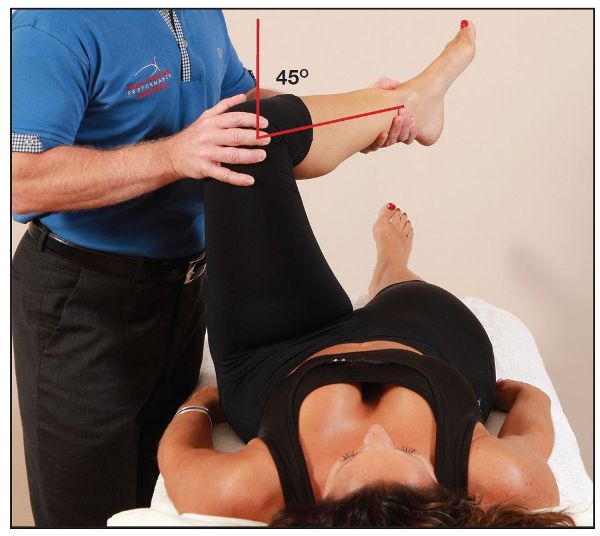
The therapist passively flexes the patient’s hip and knee to 90 degrees (I call it the 90/90 position), as shown in Figure 8.2(a); one hand is placed over the knee and the other hand at the ankle. The hip joint is then passively taken into external rotation. A normal joint end feel range of 45 degrees should be achieved, as shown overleaf in Figure 8.2(b).
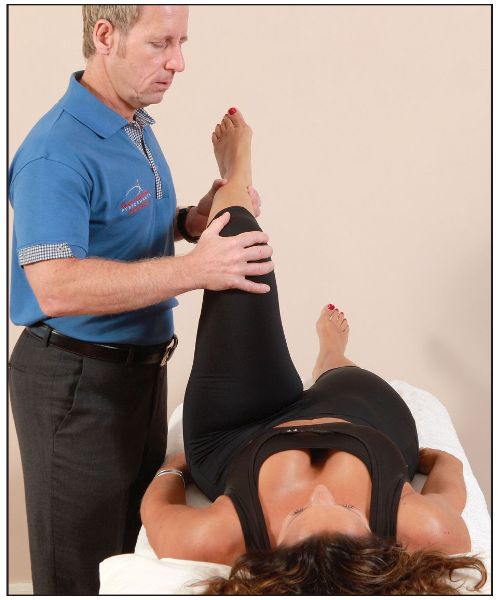
Figure 8.2. Passive ROM tests: (a) The left hip and knee are passively taken into 90 degrees of flexion—the 90/90 position.
Figure 8.2. (b) The left hip is passively taken into external rotation through a normal range of 45 degrees.
2. Passive ROM for Internal Rotation
The therapist passively flexes the patient’s hip and knee to 90 degrees (as above), with one hand placed over the knee and the other hand at the ankle. The hip joint is then passively taken into internal rotation. A normal joint end feel range of 35 degrees should be achieved, as shown in Figure 8.2(c).
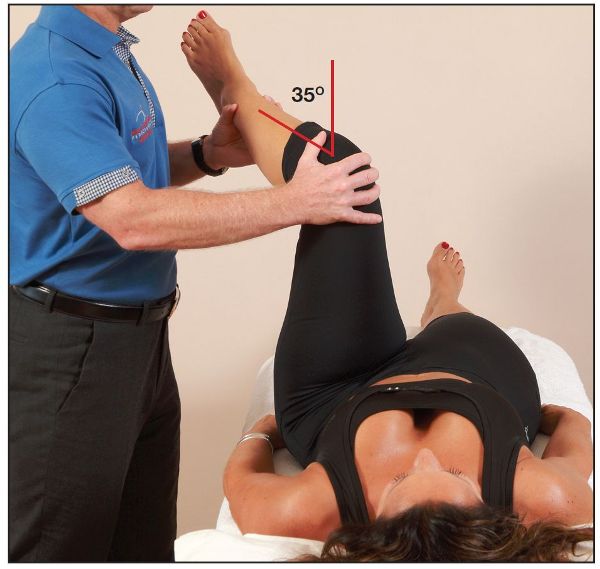
Figure 8.2. (c) The left hip is passively taken into internal rotation through a normal range of 35 degrees.
3. Passive ROM for Flexion
The hip joint is passively taken into full hip flexion. A normal joint end feel range of 130 degrees should be achieved, as shown in Figure 8.2(d).
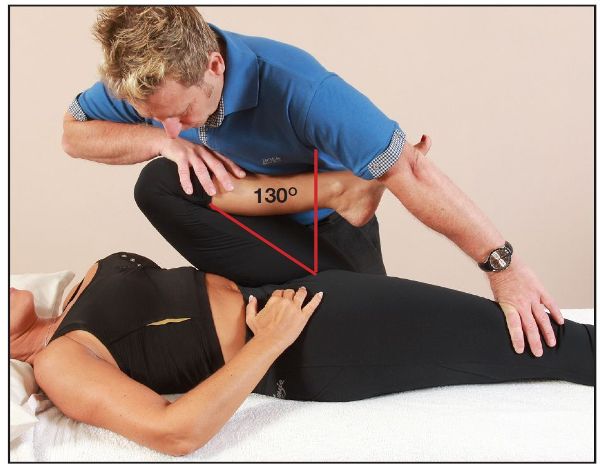
Figure 8.2. (d) The left hip is passively taken into flexion through a normal range of 130 degrees.
Note: You can see from Figure 8.2(e) that the right leg has lifted off the couch during the movement; this potentially indicates a relative shortness of the right iliopsoas muscle. This test is also known as the Thomas test and is utilized to look for a fixed flexion deformity of the hip joint, normally caused by a tight iliopsoas.
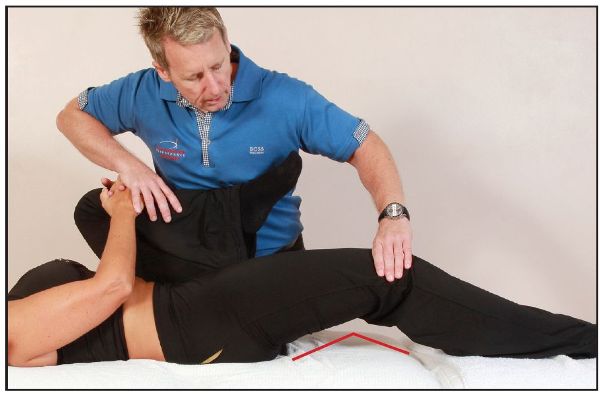
Figure 8.2. (e) The right hip is seen to be held in flexion, indicating a short iliopsoas muscle (Thomas test).
4. Quadrant Test
The quadrant test is designed to assess the inner and outer quadrants of the hip joint. The therapist passively flexes the patient’s hip to 90 degrees; one hand is placed over the knee and the other hand at the ankle. Next, the therapist applies a force longitudinally through the long axis of the femur, as shown in Figure 8.3(a). The therapist then abducts (with compression) the hip in order to assess the outer quadrant, as shown in Figure 8.3(b), and adducts the hip (with compression) to assess the inner quadrant, as shown in Figure 8.3(c).
If there were any underlying pathology located within the hip joint, this test would be positive, as indicated by the motion becoming resistant, as well as the patient perceiving some form of discomfort or even pain.
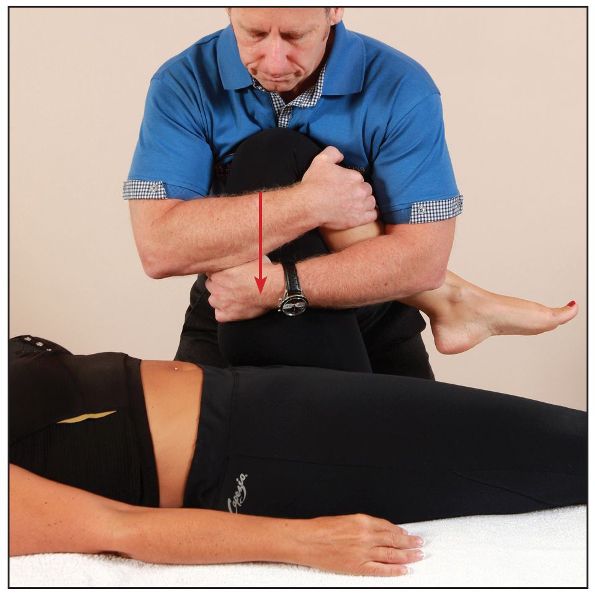
Figure 8.3. Quadrant test: (a) The left hip is compressed in neutral (90 degrees).
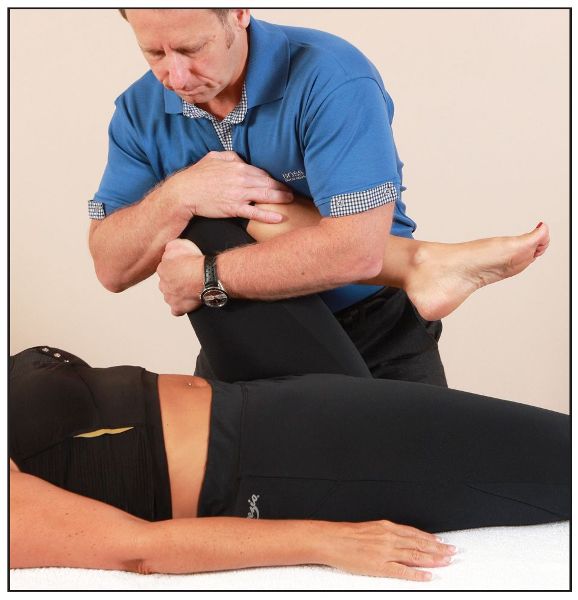
Figure 8.3. (b) The outer quadrant is tested through abducting and compressing.
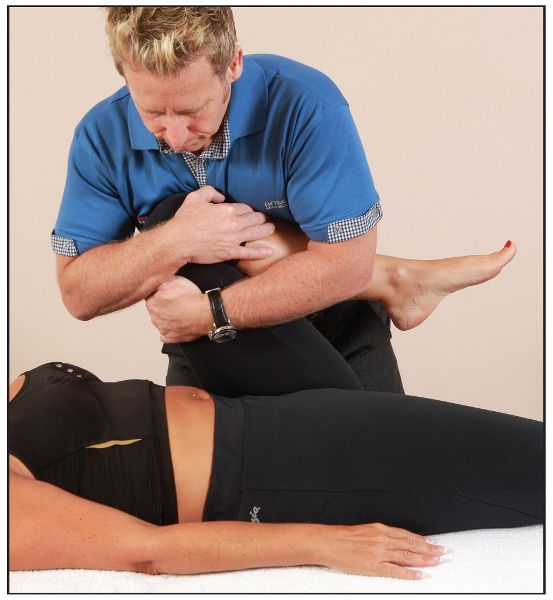
Figure 8.3. (c) The inner quadrant is tested through adducting and compressing.
5. FABER Test
The FABER test (or Patrick’s test, named after Hugh Talbot Patrick) relates to the specific motion of flexion, abduction, and external rotation.
The therapist places the patient’s hip into a position of flexion, abduction, and external rotation, as shown in Figure 8.4. The presence of a restriction or pain might indicate a pathological change within the hip joint or possibly a pelvic (SIJ) dysfunction, especially if this motion is particularly painful to the SIJ. Let’s look at an example. If you notice that the left side is restricted or painful (to the groin or lateral hip), while trying to simply place your patient into the FABER position of flexion, abduction, and external rotation, then this could be caused by a pathological condition within the left hip joint. Alternatively, the restriction/pain could actually be related to the right-side innominate being held in a position of anterior rotation and showing a positive FABER test on the left side; in this case a correction of the right anterior innominate (see Chapter 13) might improve the overall interpretation of the FABER test on the left side. However, if an innominate correction makes no difference whatsoever to the FABER position, one can assume that there is either an actual musculoskeletal issue present within the hip joint, or the SIJ is implicated (if there is pain in the area of the posterior part of the pelvis, near to the PSIS); both of these pathological conditions would require further investigation.
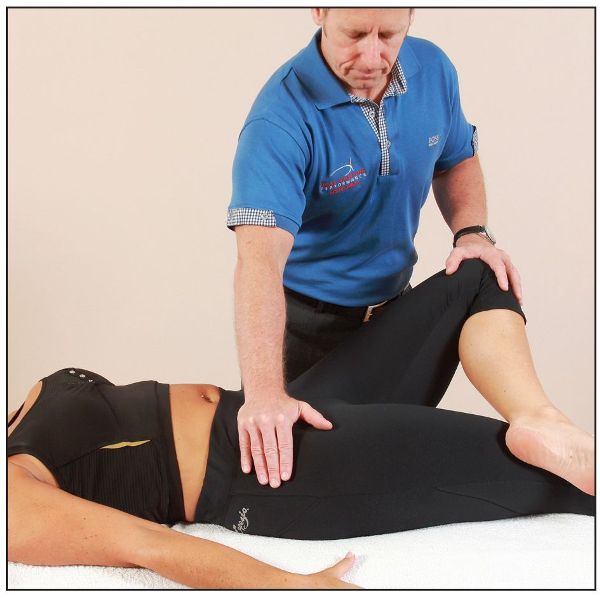
Figure 8.4. FABER test: testing the left hip.
6. FAIR Test
The FAIR test stands for flexion, adduction, and internal rotation and is commonly used to identify piriformis syndrome (this test is also known as the FADIR test—flexion, adduction, internal rotation). For the particular motion I will be demonstrating, however, I have modified the test to rule out any underlying pathology within the hip joint.
The patient adopts a supine position and the therapist places the patient’s hip into a starting position of flexion, abduction, and external rotation, as shown in Figure 8.5(a); the therapist then continues the motion, with flexion, adduction, and internal rotation, as shown in Figure 8.5(b). If there is a restriction or pain present (normally felt within the groin area) during this test, then pathological changes within the hip joint might be indicated. However, if the patient perceives pain only to the central part of their buttocks, and not to the area of the groin, then the piriformis muscle would be implicated.
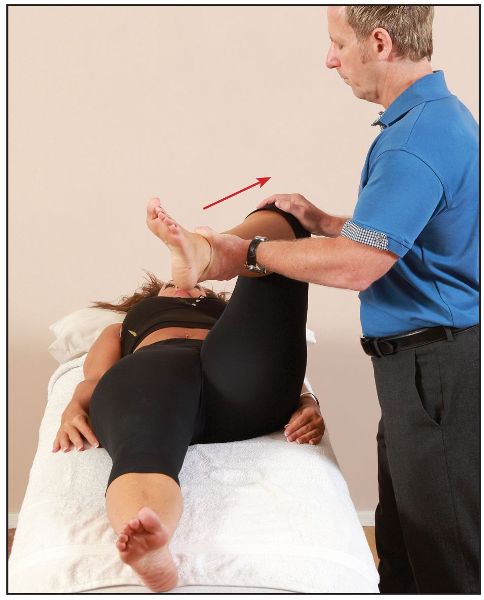
Figure 8.5. FAIR test: (a) Starting position for testing the left hip.
7. Thomas Test and Modified Thomas Test
Thomas Test
This test is used to look for a fixed flexion deformity of the hip joint and the relationship to the apparent shortness of the hip flexors and in particular of the iliopsoas muscle.
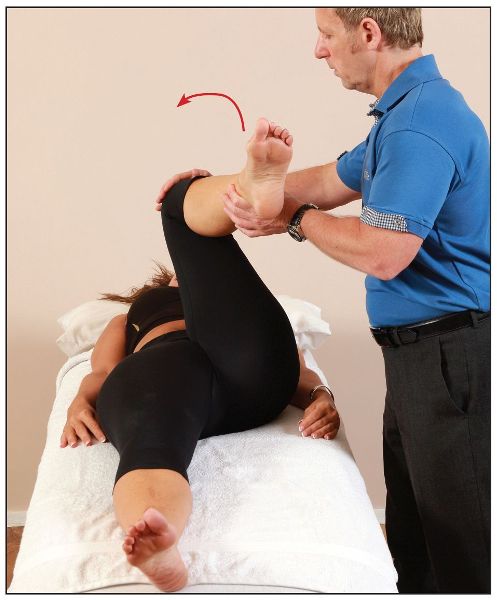
The patient is asked to lie on their back on the couch and hold onto their left knee. As the patient rolls backward, they pull their left knee as far as they can toward their chest (the therapist can assist with this motion if needed), as shown in Figure 8.6(a). The full flexion of the hip encourages full posterior rotation of the innominate bone and helps to flatten the lumbar lordosis. A normal length of the iliopsoas, and a negative test, will be found where the right posterior thigh stays in actual contact with the couch, as shown in Figure 8.6(a).
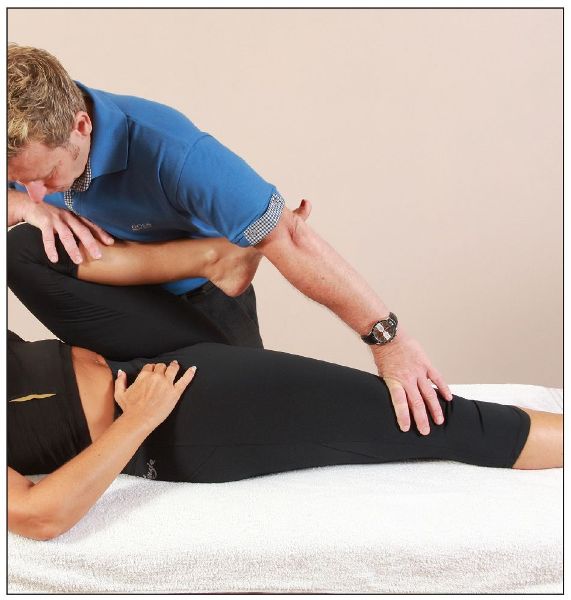
Figure 8.6. Thomas test: (a) A normal length of the right iliopsoas, as indicated by the posterior part of the hip in contact with the couch.
A fixed flexion deformity, potentially caused by shortness of the right iliopsoas, is indicated if the patient’s right hip has lifted off the couch, as shown by the arrow in Figure 8.6(b).
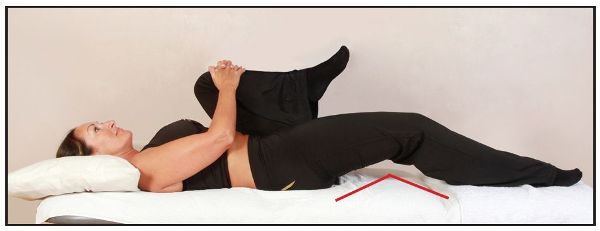
Figure 8.6. (b) The right hip is off the level of the couch, indicating a shortness of the iliopsoas.
Modified Thomas Test
You may recall that this test was demonstrated in Chapter 7 on METs; however, it is important to mention the test again, as I believe it is very relevant, especially as the specific muscles tested (iliopsoas/rectus femoris) will have a direct effect on the hip joint as well as on the pelvis.
The modified Thomas test is used to test for relative shortness of the iliopsoas, rectus femoris, adductors, and TFL/ITB. I always point out to my students that the iliopsoas muscle in particular (out of all the muscles mentioned) is always involved in one way or another in any pathological changes to the hip joint, as well as being an integral part of the functionality of the pelvis and lumbar spine.
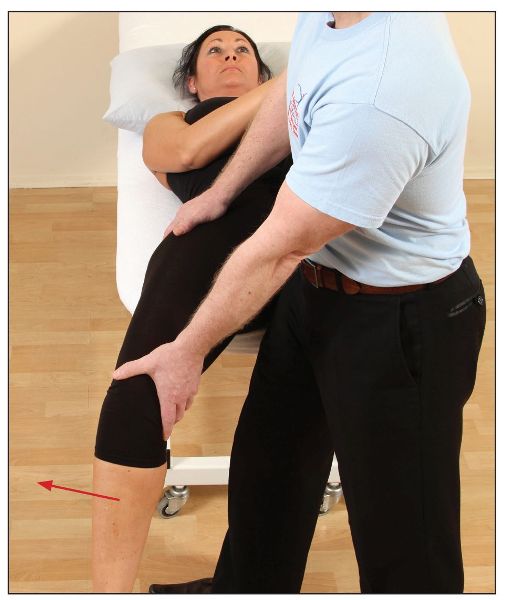
To test the right hip, the patient is asked to lie back on the edge of a couch while holding onto their left knee. As they roll backward, the patient pulls their left knee as far as they can toward their chest, as shown in Figure 8.7(a). The full flexion of the hip encourages full posterior rotation of the innominate bone and helps to flatten the lumbar lordosis. In this position, the therapist looks at where the patient’s right knee lies, relative to the right hip. The position of the knee should be just below the level of the hip; Figure 8.7(a) demonstrates a normal length of the right iliopsoas and rectus femoris.
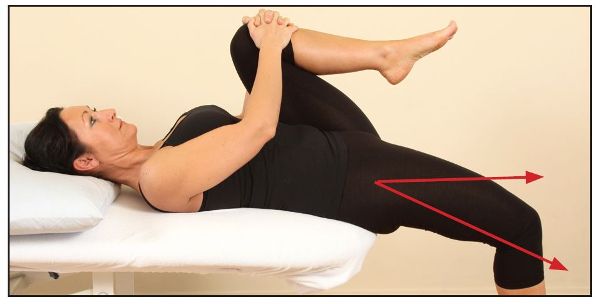
Figure 8.7. Modified Thomas test: (a) The right knee is below the level of the hip, indicating a normal length of the iliopsoas and rectus femoris.
In Figure 8.7(b) the therapist is demonstrating with their arms the position of the right hip compared with the right knee. You can see that the hip is held in a flexed position, which confirms the tightness of the right iliopsoas in this case. A tight rectus femoris muscle can also be seen, because the knee is held in extension.
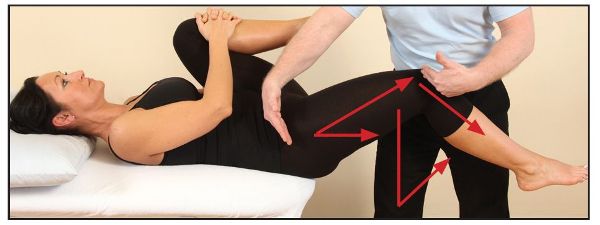
Figure 8.7. (b) A tight right iliopsoas is confirmed. Because the knee is held in extension, a tight rectus femoris is also evident.
With the patient in the modified Thomas test position, the therapist can apply an abduction of the hip (Figure 8.8), and an adduction of the hip (Figure 8.9). A ROM of 10–15 degrees for each of these is commonly accepted to be normal.
If the hip is restricted in abduction, i.e. a bind occurs at an angle of less than 10–15 degrees, the adductor muscles are held in a shortened position; if the adduction movement is restricted, the ITB and the TFL are held in a shortened position.
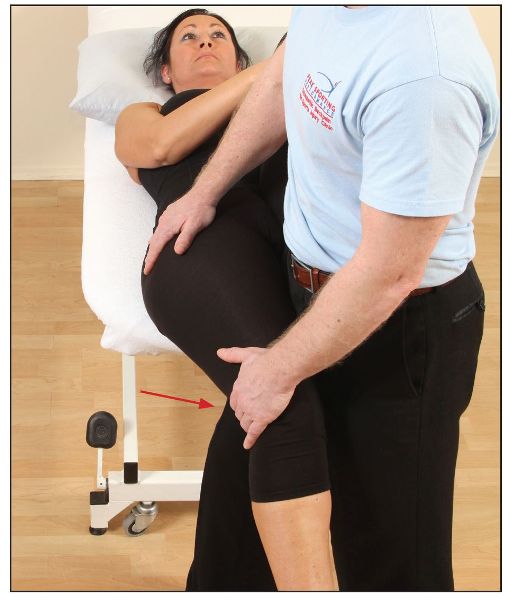
Figure 8.9. Restricted hip adduction, indicating a tight ITB/TFL.
Hip Joint Pathology
Mitchell et al. (2003) carried out a study entitled “Hip joint pathology: Clinical presentation and correlation between magnetic resonance arthrography, ultrasound, and arthroscopic findings in 25 consecutive cases.” They discussed that the hip joint is becoming increasingly recognized as a source of groin pain as well as buttock and lower back pain.
In their study they found that all of the subjects’ hips had undergone an arthroscopy at some stage, and that they had some underlying pathology; furthermore, 72% of the patients examined reported pain in the lumbar spine and also in the groin area. Some of the patients, however, presented with pain in the buttocks (36%), lateral side of knee (20%), thigh (16%), hamstring (12%), and sciatic nerve (16%), and even in the area of the abdomen (8%).
Those authors mentioned that, although back pain is a very common musculoskeletal symptom, a possible cause of the back pain seen with hip joint pathology is the close association of the psoas muscle with the anterior surface of the hip joint.
The only consistently positive clinical test result was a restricted and painful hip quadrant compared with the contralateral hip (the pain in this test could be in the groin, lateral hip, buttock, or lower back). It should be noted that a painful hip quadrant can also arise from some other local pathology (such as a psoas bursitis or tendinopathy), and that a tight hip quadrant can arise from tight gluteal muscles. A positive FABER test result was found in 88% of the subjects examined, with pain usually in the lateral hip, but occasionally in the groin or buttock. The differential diagnosis of a positive FABER test result is SIJ pathology, especially if it refers to the contralateral buttock.
The conclusion was that hip pathology, particularly acetabular labral pathology (68% diagnosed with labral tears), might be more common than had previously been thought. In those patients with chronic groin and lower back pain, especially where there is a history of an acute injury, a high index of suspicion should be maintained. Clinical signs of a painful, restricted hip quadrant and a positive FABER test result should suggest magnetic resonance (MR) arthrography in the first instance, and the consideration of hip arthroscopy if positive.
Acetabular Labral Tear
The acetabular labrum is a ring of fibrocartilage that connects around the rim of the acetabulum; its main function is to help deepen the socket to assist in preventing dislocations. It is similar to the glenoid labrum located within the shoulder joint.
Some patients and athletes (mostly women) who I have seen have torn the labrum mainly through a rotatory type of sporting motion, e.g. aerobics, skiing, or hockey. However, I have also come across a lady who tore her right acetabular labrum (Figure 8.10) by forcefully trying to pull her wellington boot out of the mud when it got stuck. There are other types of injury mechanism, such as a fall; as discussed in the case study later, this trauma caused the person in question to sustain a tear of the labrum.
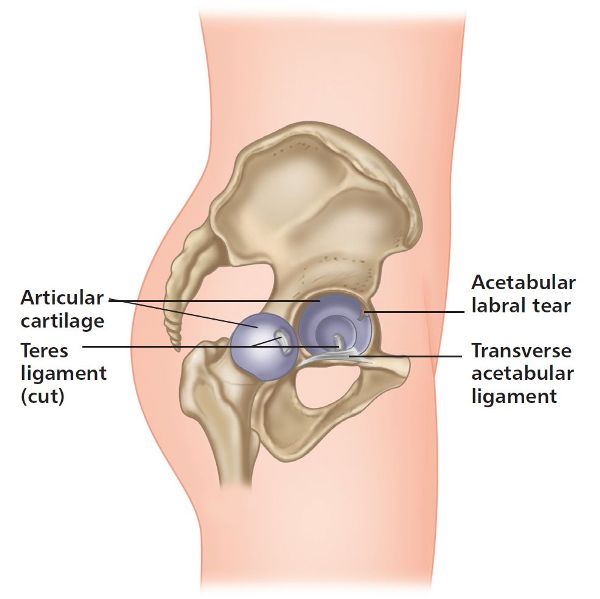
Figure 8.10. Acetabular labral tear.
Patients generally tend to have some discomfort in the area of the groin. This is not always true, however—some have pain in all sorts of places (think back to the Mitchell research article), and one would not even consider the hip joint to be the responsible structure in those cases.
It has been said that patients who have an acetabular labral tear do not get diagnosed for at least 18 months to two years; I believe the likely reason for this is that the majority of physical therapists have difficulty in confirming the tear. This must also be true of me, especially in my clinic at Oxford, as the majority of patients who I consider to be presenting with a suspect labral tear have had pain, as well as a restricted motion of the hip joint, for well over a year. What I have also noticed in the past is that most of my patients diagnosed with an acetabular labral tear are female.
I remember once discussing with a patient on the telephone the pain she was suffering around the hip and groin areas. The next bit may sound rather strange, but while I was chatting to her I asked her to lie on the floor on her back and bring her knee all the way toward her chest on her non-symptomatic side. She reported back, saying that the movement was no problem and that no pain or stiffness was felt. I then asked her to repeat the same movement on the symptomatic side; this time she said it was a struggle to perform the movement without pain, and her groin area was particularly stiff. I told her to go for an MRI scan of her hip joint, as I said it was probably a labral tear. My theory of her hip problem was correct, as she emailed me a few weeks later to tell me the news and to also say that she was being scheduled for an arthroscopy to resolve the tear.
A clicking sensation and even a locking type of feeling in the groin area are some of the symptoms that patients have mentioned to me. I strongly believe that the longer the labral tear is left (without treatment), the more the hip joint will accumulate deterioration and permanent damage, e.g. osteoarthritis, especially later on in life.
Case Study
An osteopath friend of mine asked me if I could have a look at her, as she was suffering from pain that she felt was located in the right lower part of her buttock, near to the area of the ischial tuberosity. However, she also mentioned that sometimes she would feel the pain in other areas of her body, for example to the upper part of her right hamstrings; at other times, she would feel the pain in the central aspect of her right buttock. Weirdly, on yet another day, the pain was felt in the greater trochanter of her right hip—very confusing or what?
The history was very important, as the initial injury sustained occurred well over four months previously. It happened while she was running and she fell on some ice, landing heavily on the right side of her body; she said it was a nasty fall, because at the time, she experienced a lot of pain, and there was substantial bruising around the right hip and thigh.
She rested for a week or so, but every time she went for a run she felt pain in one of the four areas that I have already mentioned. She had consulted a few practitioners during that time and received various opinions on the diagnosis. Some said the pain originated from a disc prolapse, while others said it was caused by a hamstring tendinopathy, piriformis syndrome, trochanteric and ischial bursitis, a sacrotuberous ligament sprain, and even facet joint syndrome, to name but a few conditions. She had an MRI scan of her lumbar spine and pelvis, but nothing of relevance was found.
I must admit that when I palpated the potential sites of pain, the areas of the ischial tuberosity, sacrotuberous ligament, piriformis, and trochanteric bursa were particularly tender. One might suspect any of these structures to be responsible for her pain; I even considered that the lumbar spine might be responsible, as after initially screening her hip joint, I found nothing of concern at the time of the examination.
A few weeks passed, and after a long run of approximately 10 miles (16km), the patient felt pain in her groin and started to run with a limp because of the discomfort. Her GP was a little frustrated, as the MRI of her lumbar spine and pelvis confirmed no pathology was present, so a local corticosteroid was injected into the hip joint, just to see if the symptoms would change. The pain seemed to reduce almost immediately, especially over the following few days; she was therefore scheduled for an MR arthrogram of her hip joint, and a posterior labral tear of the acetabulum was eventually diagnosed. The labral tear was quite substantial, so an arthroscopy was performed and the labrum repaired. The patient is now able to run with no pain in any of the areas initially reported as problematic.
This case study hopefully reinforces Dr. Ida Rolf’s words regarding not treating where the pain is. If the area of the above patient’s presenting pain had been treated, then without a doubt she would not have gotten any better unless she had simply rested completely from running, which in this case she definitely did not want to do.
Femoroacetabular Impingement
Another pathological problem associated with the hip joint that I have come across many times in my patients is a condition called femoroacetabular impingement (FAI). This condition can also be responsible for causing a referred type of pain to various sites of the body, similarly to the presenting symptoms of an acetabular labral tear.
The words “femoroacetabular impingement” relate to an area of entrapment between the femur (thigh bone) and the acetabulum (socket). This is a condition whereby some of the soft tissues around the hip joint are being compressed (impinged), and this pathology is generally considered to be caused by abnormally shaped bones at this joint. Because of the altered shape, the femur and the acetabulum do not fit together perfectly, hence the reason why they start to rub against each other and cause damage in the joint.
With femoroacetabular impingement, bone spurs tend to develop around the femoral head (ball) and/or along the acetabulum (socket) of the hip bone. The extra bone overgrowth causes these bones to rub against each other, rather than gliding smoothly. Over time, this can result in the tearing of the labrum and the breakdown of articular cartilage, which can eventually cause degenerative changes that can later lead to osteoarthritis.
Types of FAI
There are three main types of FAI: cam, pincer, and combined cam and pincer.
1. Cam-Type FAI
Cam-type FAI is generally more frequent in men than in women. With this condition the femoral head is not as round as it naturally should be and cannot rotate smoothly inside the acetabulum. A bump forms on the edge of the femoral head that can have the appearance of a “pistol grip” (Figure 8.11). As a result of this extra growth of bone spur, increased shearing-type forces are placed on the articular cartilage and also on the acetabular labrum.
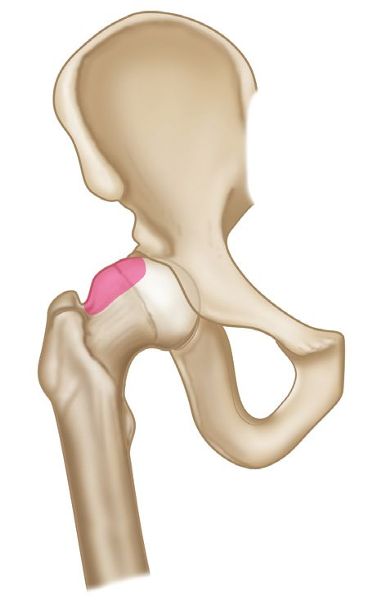
Figure 8.11. Cam-type impingement.
2. Pincer-Type FAI
A pincer-type impingement occurs more often in women than in men. In this case an extra bone growth extends out over the normal rim of the acetabulum (Figure 8.12). As a result of this pincer-type impingement, the labrum can be forcefully compressed and subsequently torn under the prominent rim of the acetabulum.
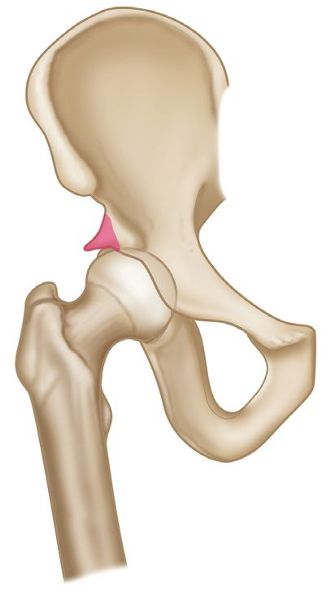
Figure 8.12. Pincer-type impingement.
3. Combined Cam-Type and Pincer-Type FAI
Combined impingement just means that both the pincer and the cam types are present simultaneously (Figure 8.13).
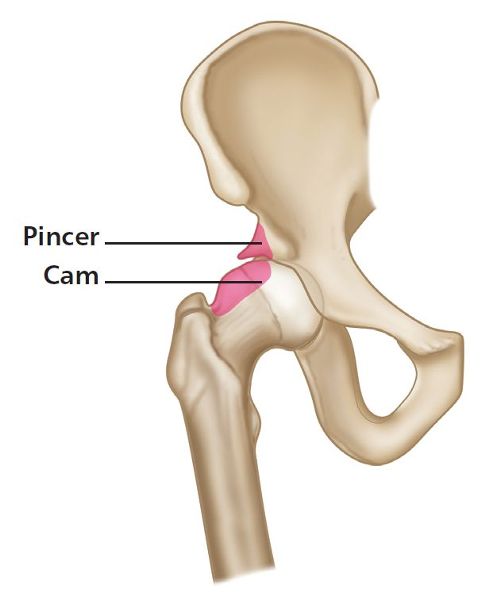
Figure 8.13. Combined cam-type and pincer-type impingement.
With femoroacetabular impingement, patients tend to have pain initially in their groin; this is normally associated with symptoms of clicking, locking, or catching, especially when chronic impingement has resulted in an acetabular labral tear. When a labral tear and FAI both exist at the same time, the presenting symptoms tend to get worse, usually with prolonged periods of standing, sitting, or walking, but particularly with pivotal movements on the affected leg. Because of the chronicity of the condition, secondary problems naturally tend to be present: for example, some patients may limp because of the pain and stiffness, and some may present a Trendelenburg sign. Other patients can experience ongoing pain in their buttocks, lower back, and SIJs, as well as in their thighs and knees.