2
Motion of the Pelvis and the Sacroiliac Joint
Previous authors have suggested that there are approximately 14 individual types of dysfunction possible within the pelvic girdle complex. This in itself suggests to me that, because there are so many types of potential dysfunction which can be present within the pelvic girdle, there logically have to be just as many types of natural motion available as well.
Pelvis Motion
Put in a relatively simple way, there are three main types of motion available within the pelvic girdle:
• Sacroiliac motion, which comprises the motion of the sacrum on the innominate bone.
• Iliosacral motion, which comprises the motion of the innominate bone on the sacrum.
• Symphysis pubis motion, which typically relates to the motion of the pubic bone on one side with respect to the bone on the other side.
Sacroiliac Motion
Sacroiliac motion is the movement of the sacrum within the innominate bone, and there are two main types: (1) anterior/forward motion, or nutation (think of this as sacral flexion); and (2) posterior/backward motion, or counter-nutation (think of this as sacral extension). Bilateral movement of the sacrum occurs with forward and backward bending of the trunk; on the other hand, unilateral movement of the sacrum occurs with flexion and extension of the hip joint and lower limbs, such as when we initiate the walking/gait cycle.
Nutation
The word nutation actually means “nodding”, and this motion of the sacral base (top part of the sacrum) is directed anteriorly and inferiorly, while the sacral apex (bottom part of the sacrum)/coccyx moves posteriorly and superiorly relative to the innominate bone, as illustrated in Figure 2.1(a).
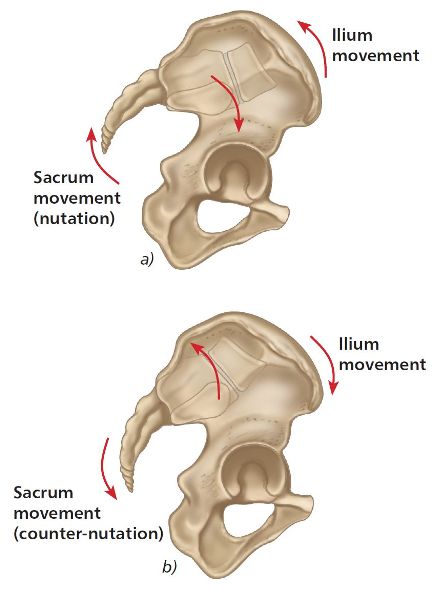
Figure 2.1. (a) Sacral nutation. (b) Sacral counter-nutation.
During nutation (which is also known as anterior nutation), the sacrum is considered to glide inferiorly down the short (vertical) arm and posteriorly along the long (horizontal) arm of the L-shaped articular surface (see Figure 2.2).
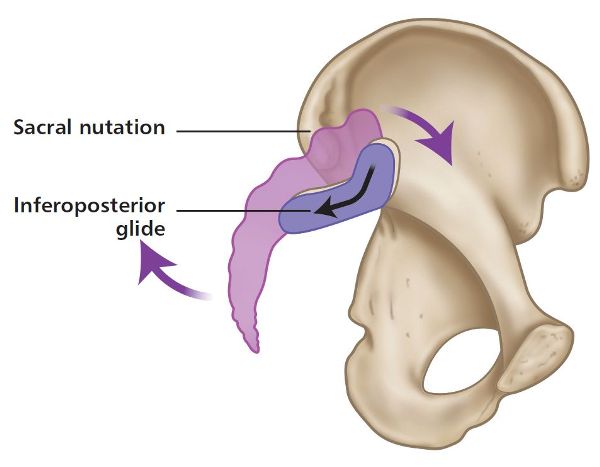
Figure 2.2. Sacral nutation: the sacrum glides inferiorly down the short arm and posteriorly along the long arm.
The natural wedge shape of the sacrum, as well as the ridges and grooves of the articular surfaces, limits nutation. In addition, the interosseous, sacrotuberous, and sacrospinous ligaments will limit how much nutation is possible, as they become taught in this position; this is considered to be the most stable position.
Vrahas et al. (1995) mention that nutation represents a movement that tightens most of the SIJ ligaments, among which are the vast interosseous and dorsal sacroiliac ligaments (with the exception of the long dorsal ligament), thereby preparing the pelvis for increased loading.
Counter-Nutation
In counter-nutation the sacral base moves posteriorly and superiorly, while the sacral apex/coccyx moves anteriorly and inferiorly relative to the innominate bone (Figure 2.1(b)). During this type of motion (which is also known as posterior nutation), the sacrum is considered to glide anteriorly along the long arm and superiorly up the short arm of the L-shaped articular surface, as shown in Figure 2.3.
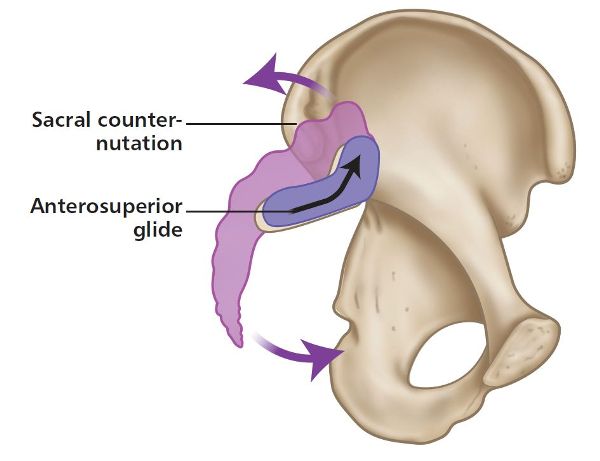
Figure 2.3. Sacral counter-nutation: the sacrum glides anteriorly along the long arm and superiorly up the short arm.
The long dorsal ligament limits this specific motion of counter-nutation. Because of the laxity of the interosseous and sacrotuberous ligaments, this sacral position of counter-nutation is considered to be the least stable.
Iliosacral Motion
Iliosacral motion is the movement permitted by the innominate bone on the sacrum. Bilateral movement (anterior and posterior rotation) of the innominate bones occurs with forward and backward bending of the trunk; on the other hand, unilateral movement (anterior and posterior rotation) of the innominate bone occurs with flexion and extension of the hip joint and lower limbs, for example during the gait cycle (similar to unilateral sacral motion).
Anterior Innominate Motion
When the hip and lower limb are extended, the innominate rotates anteriorly as the L-shaped articular surface glides inferiorly down the short arm and posteriorly along the long arm, as shown in Figure 2.4. This anterior motion of the innominate is reminiscent of counter-nutation of the sacrum.
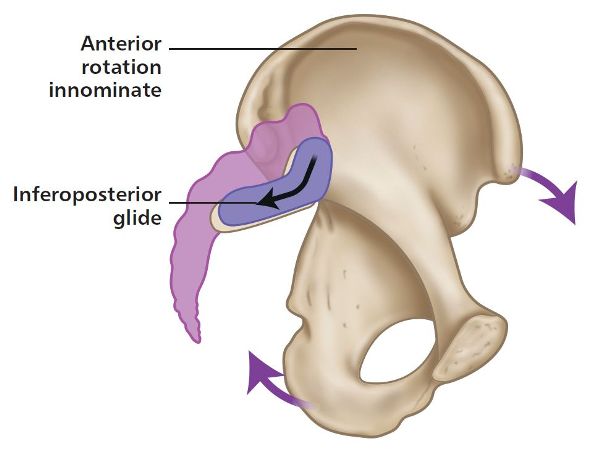
Figure 2.4. Anterior rotation of the innominate bone: the L-shaped articular surface glides inferiorly down the short arm and posteriorly along the long arm.
Posterior Innominate Motion
When the hip and lower limb are flexed, the innominate rotates posteriorly as the L-shaped articular surface glides anteriorly along the long arm and superiorly up the short arm, as shown in Figure 2.5. This posterior motion of the innominate is reminiscent of nutation of the sacrum.
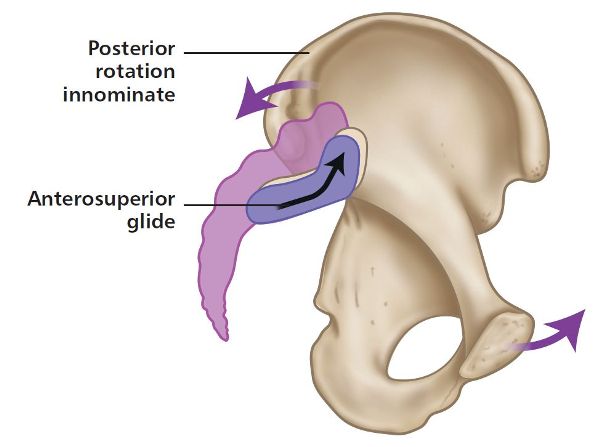
Figure 2.5. Posterior rotation of the innominate bone: the L-shaped articular surface glides anteriorly along the long arm and superiorly up the short arm.
Symphysis Pubis Motion
Anteriorly, the two hipbones are joined together to form a connection known as the symphysis pubis joint. During normal walking, the symphysis pubis joint acts as a type of pivot point for the motion of the two hipbones.
Although movement is possible at the symphysis pubis joint, it is normally restricted because of the attachments of the strong superior and inferior ligaments. The limited motion that is available mainly occurs during the walking cycle; however, movement is also possible at this joint when one adopts a stabilized standing position while balancing on one leg.
Symphysis pubis dysfunction (SPD) is generally classified according to the position in which the joint is fixed—either a superior symphysis pubis or an inferior symphysis pubis, as shown in Figure 2.6.
Studies have shown that if you were to maintain a one-legged standing position for a few minutes, a superior motion (shear) of the symphysis pubis would be seen. If the one-legged motion is maintained over an extended period of time, recurrent SPD can result.
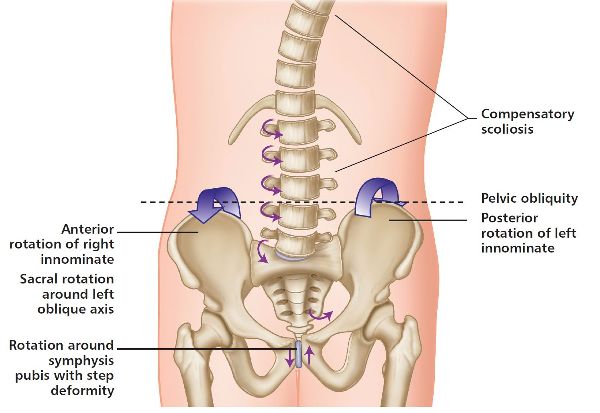
Figure 2.6. Superior and inferior motion of the symphysis pubis joint.
SPD is commonly associated with pregnancy and childbirth; it is thought to affect to varying degrees around one in five women who are pregnant, with around 5–7% of them continuing to experience ongoing painful symptoms after childbirth. During pregnancy, and especially during childbirth, the symphysis pubis ligaments become more lax in order to allow a natural separation of this joint, since this increased movement is needed to widen the internal diameter of the pelvic bowl.
Combined Sacroiliac and Iliosacral Motion
We have looked at the individual motion of the sacrum during nutation and counter-nutation within the innominate bones (sacroiliac) and how the innominate bone rotates around the sacrum (iliosacral). Next, we will combine the motion of the sacroiliac, iliosacral, lumbar, and hip joints during forward and backward bending of the trunk.
When the pelvic girdle, i.e. the two innominate bones and the sacrum, rotate as a unit through the hip joint, this motion is known as an anterior pelvic tilt or a posterior pelvic tilt.
Bilateral Motion—Forward Bending
Bilateral (both sides) nutation and counter-nutation are the natural movements that the sacrum performs when we forward and backward bend our trunk while in a stable position on two legs.
On the initiation of forward bending of the trunk, the pelvic girdle will shift posteriorly to control the center of gravity in order to maintain the balance. The sacrum will be in a position of nutation and will stay there throughout the full range of motion (ROM). The left and right innominates rotate symmetrically on the femur in an anterior direction (anterior pelvic tilt), and the PSIS will move symmetrically in a cephalic direction (superior) as the lumbar spine (L5) flexes on the sacrum. As trunk flexion continues, there will come a natural point when tension is increased within the sacrotuberous ligament, biceps femoris, and thoracolumbar fascia, and a position where sacral nutation ceases. At this point the innominate bones continue rotating anteriorly; however, because of the increased tension in the soft tissues (explained earlier), especially the hamstrings, the final position of trunk flexion is that in which the sacrum is considered to be in a position of relative counter-nutation, even though the sacrum will appear to be in a position of nutation, as shown in Figure 2.7.
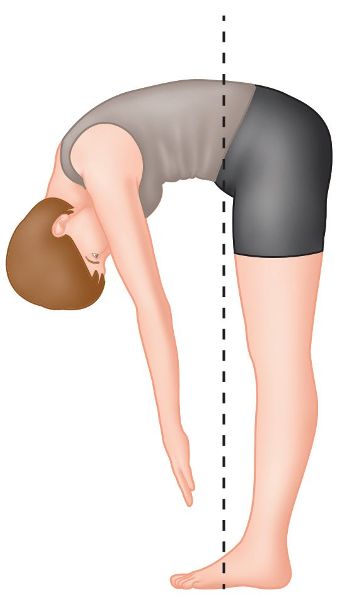
Figure 2.7. Bilateral motion during forward bending.
On the return to a standing position, the sacrum remains in a position of nutation until the erect posture is achieved; at this crucial point, the sacrum slightly counter-nutates to maintain a suspension between the two innominate bones. (Note that, even though I have mentioned counter-nutation, the sacrum still maintains an overall position of nutation.)
Bilateral Motion—Backward Bending
This time, on the initiation of backward bending, the pelvic girdle will shift anteriorly, while the innominate bones symmetrically rotate posteriorly on the femur (posterior pelvic tilt); the PSIS can be seen and felt to rotate in a caudal direction (inferiorly), while the thoracolumbar spine continues extension until L5 extends on the sacrum, as shown in Figure 2.8. The sacrum remains in a position of nutation throughout backward bending; this position is considered to be the most stable because of the compression of the SIJs.
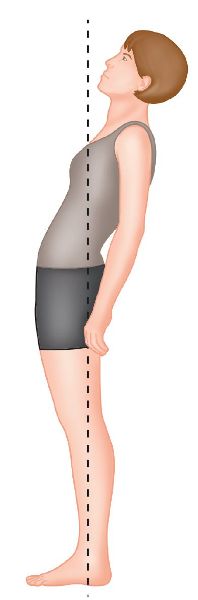
Figure 2.8. Bilateral motion during backward bending.
Unilateral (One Side) Motion of the Sacrum
During the walking/gait cycle, the sacrum is required to perform its natural motion in a way that is completely opposite to that during forward and backward bending movements. This time we need a specific type of unilateral (one-sided) motion of the sacrum, not a bilateral motion. What I mean by this is the following: as we walk from point A to point B, we need one side of the sacrum (e.g. the left side) to move forward into nutation, while at the same time the opposite side (right side in this case) is moving backward into counter-nutation (or posterior nutation). This movement gets a little bit more complex, as the nutation/counter-nutation will naturally induce a movement of sacral rotation. The problem we encounter now is that when you have a rotation of the sacrum (or in fact any vertebrae), a coupled (combined) motion with side bending also occurs; the general rule (according to the current research) is that the side bending motion will be coupled to the opposite side of the sacral rotation. This follows what is typically known as a Type I or neutral mechanic (explained in detail in Chapter 6), in which the rotation and side bending are coupled to the opposite side; for instance, the sacrum can perform a side bending motion to the left side, but it will rotate to the opposite side (to the right side in this case).
Consider the following example to illustrate what I am trying to say. If the left side of the sacrum goes forward into anterior nutation, it will rotate to the right side (the sacral base will palpate deeper on the left side) and will also side bend to the left (Figure 2.9). However, the right side of the sacrum will also rotate to the right side, but this time the sacral base will be in a posterior nutation position (counter-nutation, as the sacral base will now palpate shallow on the right side).
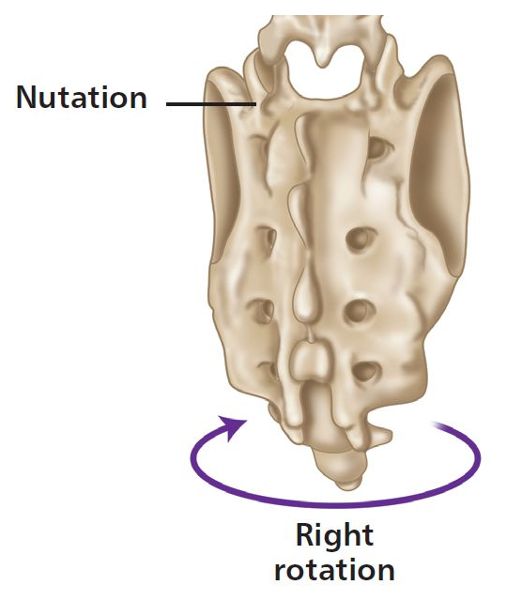
Figure 2.9. Example of a unilateral motion of the sacrum.
The movement discussed above, in which you have a rotation to one side and a side bending motion to the other, is also known as a sacral torsion; this specific type of sacral movement is considered to occur around an oblique axis (see figure 2.10).
Sacral Axis
There are approximately six types of sacral axis (Figure 2.10):
• Superior transverse axis
• Middle transverse axis
• Inferior transverse axis
• Left oblique axis
• Right oblique axis
• Vertical axis
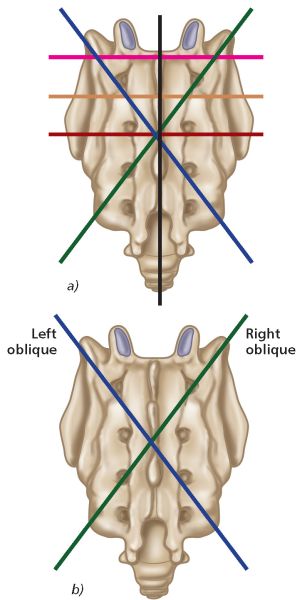
Figure 2.10. (a) Sacral axis, (b) Left oblique axis and right oblique axis.
It is not within the scope of this book to cover all the different sacral axis variations. For this text, however, the one of particular relevance is the middle transverse axis (MTA), because sacral dysfunctions are palpated and treated about this horizontal axis, according to Mitchell terminology. Moreover, this axis is considered to undergo a transformation during the gait cycle into the oblique axis, which is the specific axis that will be focused on in this text.
Oblique Axis
It has been suggested by some authors that there is a left oblique axis and a right oblique axis (see Figure 2.10(b)). The left oblique axis runs through the left sacral base and continues through the right inferior lateral thangle (ILA); the right oblique axis runs through the right sacral base and continues through the left ILA.
In Chapter 3 I will take you through exactly how the oblique axis is utilized in combination with the movements of the kinetic chain as we perform sacral motion during the walking/gait cycle. For now, however, we will focus on the two natural physiological motions that the sacrum is capable of: “left rotation on the left oblique axis,” which is typically called a left-on-left (L-on-L) sacral torsion, and a “right rotation on the right oblique axis,” commonly known as a right-on-right (R-on-R) sacral torsion.
There are, however, also two non-physiological motions of the sacrum: “left rotation on the right oblique axis,” which is typically called a left-on-right (L-on-R) sacral torsion, and a “right rotation on the left oblique axis,” commonly known as a right-on-left (R-on-L) sacral torsion.
When authors mention the word “sacral torsion,” they can mean one of two things: a naturally occurring motion of the sacrum that is performed, for example, during the gait cycle (Chapter 3 will explain this); or a dysfunction of the sacrum, in that it becomes fixed in this specific type of position or torsion.
Physiological Motions (Anterior Motion Fixation/Nutation)
Before we look at sacral torsions, let’s just remind ourselves of the neutral position of the sacrum, as shown in Figure 2.11(a) and indicated by the model in Figure 2.11(b).
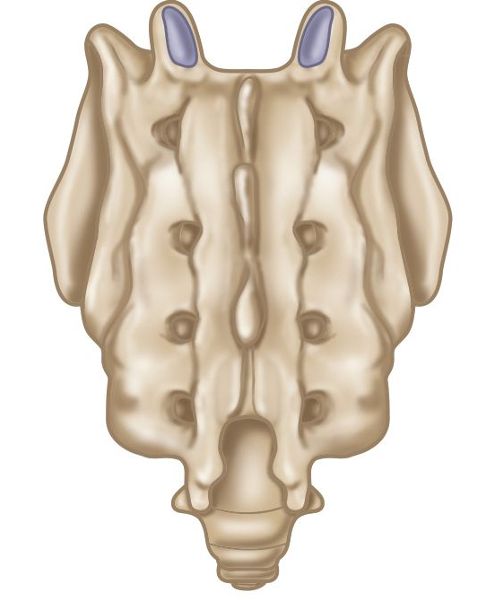
Figure 2.11. (a) Neutral position of the sacrum.

Figure 2.11. (b) Neutral position of the sacrum, as indicated by the model.
Left-on-Left (L-on-L)
Let’s discuss a L-on-L sacral motion/torsion a bit further: it relates to the sacral bone being in a position of left rotation on the left oblique axis. This will be specific to the case where the sacrum has rotated to the left side, so the sacral sulcus (the area that is naturally formed by the junction of the sacral base with the corresponding ilium) will palpate as deep on the right. Moreover, the ILA as well as the sacral sulcus will palpate as posterior (shallow) on the left side, which will indicate that the right side of the sacrum has anteriorly nutated to the left, as shown in Figure 2.12(a).
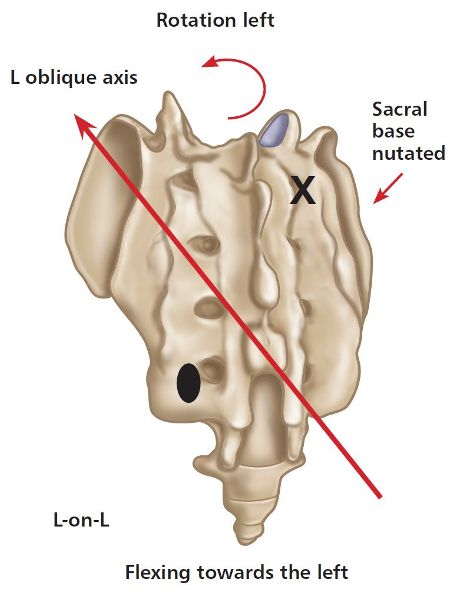
Figure 2.12. (a) Left-on-left (L-on-L) sacral motion/torsion. X = Anterior or deep. ![]() = Posterior or shallow.
= Posterior or shallow.
The specific motion of a L-on-L sacral torsion is demonstrated in Figure 2.12(b).

Figure 2.12. (b) L-on-L sacral torsion, as demonstrated by the model—sacral nutation is shown on the right side.
Right-on-Right (R-on-R)
A R-on-R sacral torsion relates to a right rotation on the right oblique axis. This will be specific to a sacrum that has rotated to the right side, so the sacral sulcus will palpate as deep on the left side. The ILA and the sacral sulcus will palpate as posterior (shallow) on the right, which will indicate that the left side of the sacrum has anteriorly nutated to the right, as shown in Figure 2.13(a).
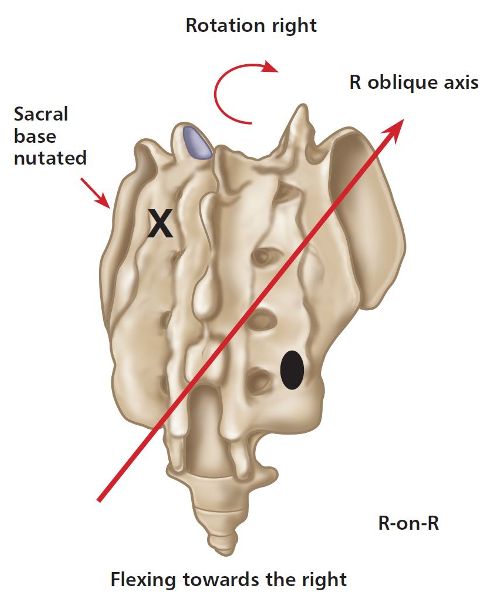
Figure 2.13. (a) Right-on-right (R-on-R) sacral motion/torsion. X = Anterior or deep. ![]() = Posterior or shallow.
= Posterior or shallow.
The model in Figure 2.13(b) is demonstrating the specific motion of a R-on-R sacral torsion.

Figure 2.13. (b) R-on-R sacral torsion, as demonstrated by the model—sacral nutation is shown on the left side.
Physiological Summary
As I have already mentioned, L-on-L and R-on-R sacral torsions are naturally occurring motions around the sacrum, although these specific motions can be fixed in a position of nutation. For example, if you have a dysfunctional position, say a L-on-L sacral torsion, then the sacrum is capable of performing this movement, as it is already fixed in this position and is potentially capable of rotating back to a “neutral” position. However, it is unable to perform a “R-on-R” sacral torsion due to the fact that the left side of the sacrum is unable to counter-nutate (posterior nutation), as this side (left) is held in a fixed position of anterior nutation.
You will read in Chapter 3 that most of the activity of our musculoskeletal system will involve the walking/gait cycle. As humans, we especially need to be able to maintain ongoing L-on-L and R-on-R sacral (torsion) motions, since these are of paramount importance to enable us to ambulate normally through the gait cycle. If the sacrum cannot perform these naturally occurring sacral torsions (motion), dysfunction occurs as a consequence.
Non-Physiological Motions (Posterior Motion Fixation/Counter-Nutation)
Non-physiological motions of the sacrum are a little bit more complex to grasp, as they are considered to be unnatural motions that occur around an oblique axis of the sacrum. If you do happen to find this type of posterior sacral dysfunction with your patients, it often tends to be caused by the lumbar spine/trunk being placed into a position of increased (forced) flexion with a combined movement of rotation (as in the motion of rotating your body to pick up a heavy weight from the floor).
It may take you a while to think about and understand this next concept but I will try my best to explain this in a relatively simple way, even though many people will still have difficulty understanding what it is I am trying to portray due to the natural complexity of this fascinating area.
Before we start I would like you to think of this motion simply as a backward/posterior torsion, whereas the other two types I mentioned in the earlier paragraphs are forward/anterior torsions.
Left-on-Right (L-on-R)
A L-on-R sacral torsion relates to a left rotation on the right oblique axis, and this will be specific to the case where the sacrum has rotated to the left side. However, because of the posterior motion of the left side of the sacrum, the sacral sulcus will now palpate as shallow on the left, and the ILA will palpate as posterior (shallow) on the left; this will indicate that the left side of the sacrum has counter-nutated or posteriorly nutated, as shown in Figure 2.14(a).
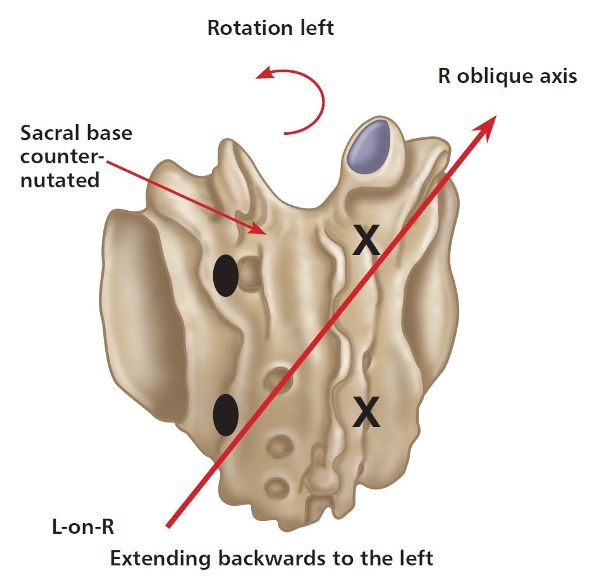
Figure 2.14. (a) Left-on-right (L-on-R) sacral torsion. X = Anterior or deep. ![]() = Posterior or shallow.
= Posterior or shallow.
This specific motion of a L-on-R sacral torsion can be seen in Figure 2.14(b), as demonstrated by the model.

Figure 2.14. (b) L-on-R sacral torsion, as demonstrated by the model—sacral counter-nutation is shown on the left side.
Right-on-Left (R-on-L)
It follows that a R-on-L sacral torsion must be the opposite of a L-on-R sacral torsion; thus, the sacral torsion this time relates to a right rotation on the left oblique axis, and this will be specific to the sacrum having rotated to the right side. Because of the posterior motion of the right side of the sacrum, however, the sacral sulcus will now palpate as “shallow” on the right, and the ILA will palpate as posterior (shallow) on the right. This will indicate that the right side of the sacrum has counter-nutated, or (if easier to understand) that the sacrum has posteriorly nutated (think of this simply as a backward motion), as shown in Figure 2.15(a).
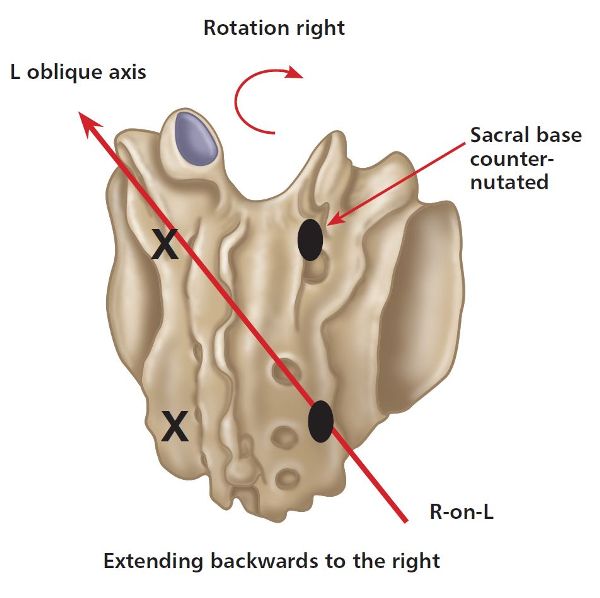
Figure 2.15. (a) Right-on-left (R-on-L) sacral torsion. X = Anterior or deep. ![]() = Posterior or shallow.
= Posterior or shallow.
Figure 2.15(b) illustrates the specific motion of a R-on-L sacral torsion, as demonstrated by the model.

Figure 2.15. (b) R-on-L sacral torsion, as demonstrated by the model—sacral counter-nutation is shown on the right side.
Non-Physiological Summary
What I would like to do now is give a brief review of the main points discussed above, so that you can better understand these specific types of dysfunction. We know that L-on-R and R-on-L sacral torsions are unnatural motions of the sacrum, hence their being termed non-physiological. These specific motions can be fixed in a position of counter-nutation or a backward torsion. For example, if you have a dysfunctional position of a L-on-R sacral torsion, the sacrum is capable of performing this backward type of movement, as it is already fixed in that position. The sacrum is, however, unable to perform the normal physiological motion of a L-on-L or a R-on-R sacral torsion, because of the fact that the left side of the sacrum is unable to nutate, since it is held in a fixed position. Another way of thinking about this is that the left side of the sacrum cannot perform the motion of anterior nutation, or simply go forward on the left, as it is held backward in a fixed position of counter-nutation or posterior nutation.
Sacral Torsions Summary
Tables 2.1 and 2.2 summarize the physiological and non-physiological motions of the sacrum. You will notice that the tables contain extra components, namely the position of the 5th lumbar vertebra, seated flexion test, lumbar spring test, sphinx test, lumbar lordosis curvature, and position of the medial malleolus. All of these will be explained in more detail in later chapters, especially Chapter 12, but have been mentioned here because my aim in this chapter is to whet your appetite to continue reading. For now, I just wanted you to be aware of all the different types of physiological and non-physiological motion that the sacrum is capable of before we progress through the rest of the chapters.
| L-on-L sacral torsion
Forward/nutation |
R-on-R sacral torsion
Forward/nutation |
|
|---|---|---|
|
Deep sacral sulcus (neutral) |
Right |
Left |
|
Shallow sacral sulcus (neutral) |
Left |
Right |
|
ILA posterior |
Left |
Right |
|
L5 rotation |
Right—ERS(R) |
Left—ERS(L) |
|
Seated flexion test |
Right |
Left |
|
Lumbar spring |
Negative |
Negative |
|
Sphinx test |
Sacral sulci level |
Sacral sulci level |
|
Lumbar lordosis |
Increased |
Increased |
|
Medial malleolus (leg length) |
Short left |
Short right |
Table 2.1. Normal physiological motion: anterior/forward sacral torsions.
| L-on-R sacral torsion
Backward/counter-nutation |
R-on-L sacral torsion
Backward/counter-nutation |
|
|---|---|---|
|
Deep sacral sulcus (neutral) |
Right |
Left |
|
Shallow sacral sulcus (neutral) |
Left |
Right |
|
ILA posterior |
Left |
Right |
|
L5 rotation |
Right—FRS(R) |
Left—FRS(L) |
|
Seated flexion test |
Left |
Right |
|
Lumbar spring |
Positive |
Positive |
|
Sphinx test |
Left sacral sulcus shallow (right sacral sulcus deeper) |
Right sacral sulcus shallow (left sacral sulcus deeper) |
|
Lumbar lordosis |
Decreased |
Decreased |
|
Medial malleolus (leg length) |
Short left |
Short right |
Table 2.2. Non-physiological motion: posterior/backward sacral torsions.