5
Leg Length Discrepancy and its Relationship to the Kinetic Chain and the Pelvis
I would personally say that the majority of patients and athletes who visit my clinic in Oxford generally present with pain somewhere in their bodies. Part of my initial screening is to have the patient stand with their back to me; with them in this position, I place both my hands on top of their iliac crest to see if there is any pelvic obliquity; in other words, I look for a low or a high side, as shown in Figure 5.1. Very often I do find that there is a discrepancy in the level of the height of the iliac crest between the two sides, which could possibly indicate a leg length discrepancy (LLD), or, as it has been alternatively termed, a short-leg syndrome or a long-leg syndrome.
LLD is possibly the most significant postural asymmetry that presents itself to the physical therapist. The existence of a considerable difference between the two sides can be very detrimental to how we function on a day-to-day basis, not least during the walking/gait cycle: the discrepancy can significantly affect not just the pelvis and SIJ but also our overall posture.
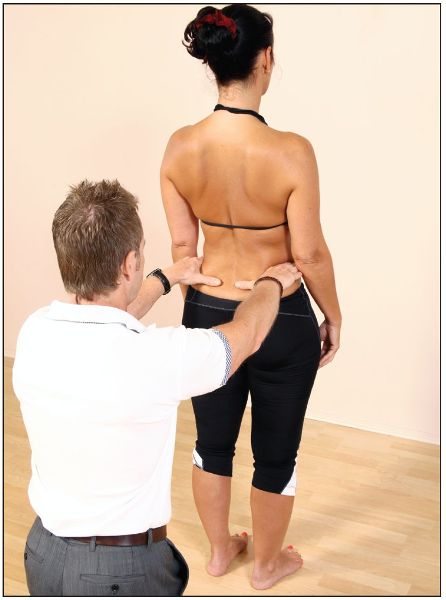
Figure 5.1. Observation of measurement of leg length by palpation of the iliac crest.
Definition: Leg length discrepancy (LLD) is a condition where one leg is shorter than the other.
One has to decide if there is an “actual” (or “true”) anatomical LLD or an “apparent” LLD, as the condition has been implicated in all sorts of deficiencies related to our gait pattern and running mechanics. LLD has also been linked to postural dysfunctions, as well as to increased incidence of scoliosis, lower back pain, SIJ dysfunction, and osteoarthritis of the spine, hip, and knee. Even stress fractures of the hip, spine, and lower extremity have been related to changes in leg length.
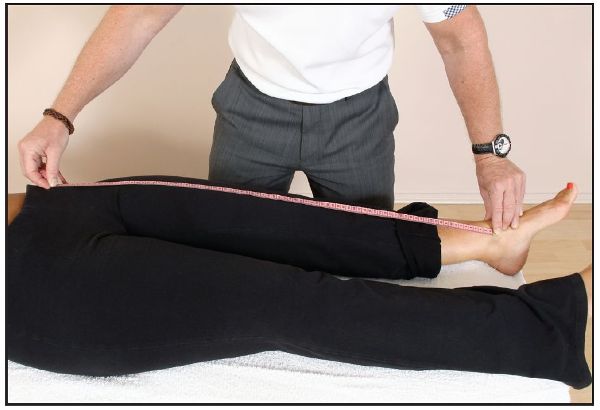
Figure 5.2. True leg length measurement, taken from the ASIS to the medial malleolus.
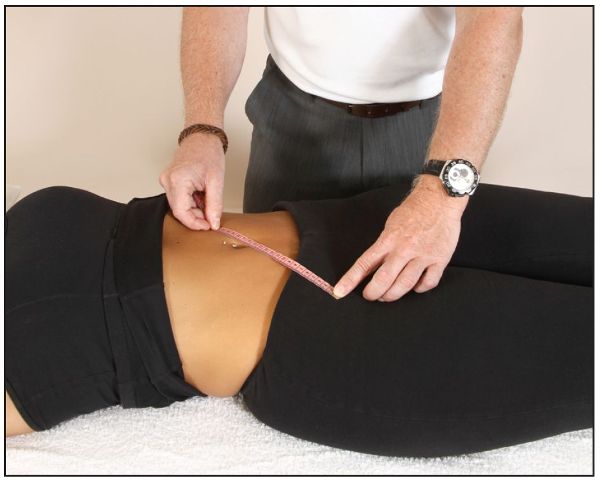
The actual (true) leg length measurement is the length that is typically determined by the use of a tape measure from a point on the pelvis—the ASIS—to the medial malleolus (distal part of the tibia), as shown in Figure 5.2; the ASIS is normally used as the landmark, since it is impossible to truly palpate the femur below the iliac crest. Before taking this measurement, it is beneficial to measure the distance from the ASIS on the left and right sides to the umbilicus, as shown in Figure 5.3, to ascertain if any pelvic rotation is present. If a difference in the two measurements is found, the pelvic rotations need to be corrected before a reassessment is done (Chapter 13).
If the measurements taken from the ASIS to the medial malleolus on both sides are the same, it can then be assumed that the lengths of the two limbs are effectively equal; on the other hand, if the measurements differ, one can assume that an actual (true) LLD is present.
The apparent leg length measurement is taken from the umbilicus to the medial malleolus, as shown in Figure 5.4. If the measurements taken on both sides are different, one can assume that a dysfunction exists somewhere, which will require further investigation.
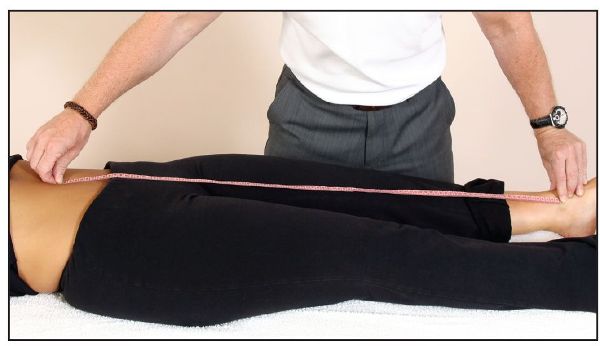
Figure 5.4. Apparent leg length measurement, taken from the umbilicus to the medial malleolus.
Supine to Long Sitting
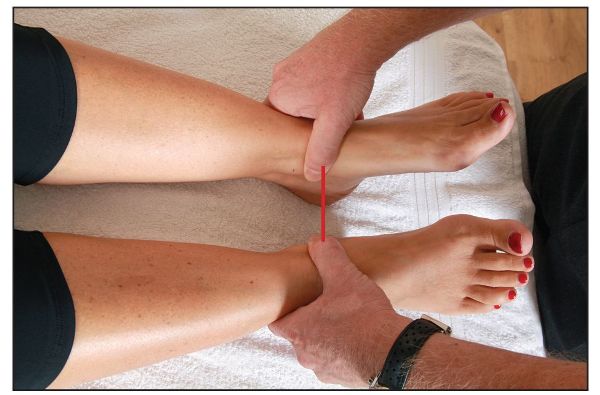
The supine to long sitting test is commonly used to ascertain the relevance of the SIJ to an apparent or true LLD. With the patient in a supine position, the therapist initially compares the relative positions of the two medial malleoli, to see if a difference exists between these two bony landmarks, as shown in Figure 5.5(a).
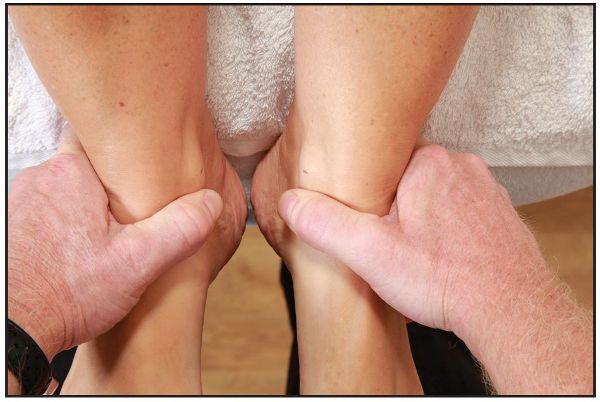
Figure 5.5. (a) Palpation for the positions of the medial malleoli (leg length) in the supine position.
Next the patient is asked to sit up, while keeping their legs extended. The positions of the two medial malleoli are compared once again, to see if there is any change, as shown in Figure 5.5(b–c).

Figure 5.5. (b) Observation of the positions of the medial malleoli (leg length) after the supine to long sitting test.
Figure 5.5. (c) Close-up view of the positions of the medial malleoli (leg length) after the supine to long sitting test. The malleoli appear to be level in this case.
If, for example, there is a posterior innominate present, the leg that appeared shorter in the supine position will now appear to lengthen with the sitting-up motion. If there is an anterior innominate present (very common on the right side), the leg that appeared longer in the supine position will now appear to shorten with the sitting-up motion, as shown in Figure 5.5(d).
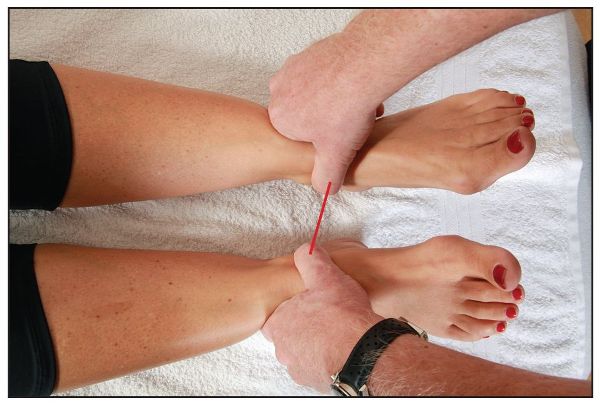
Figure 5.5 (d). Close-up view of the positions of the medial malleoli (leg length) after the supine to long sitting test. The right leg appears shorter, possibly indicating a right anterior innominate rotation.
If an actual (true) LLD is present, the true long leg will appear to be longer in the supine position as well as in the sitting position, so no obvious change will be observed (this, along with further discussion on leg length changes, will be presented in more detail in Chapter 12). For now, it is sufficient to simply note down if there are any changes in the position of the medial malleoli in the supine and long sitting positions.
Note: This test can help in differentiating between a true LLD and a sacroiliac dysfunction. Please be careful when asking your patients to perform this test: the motion of the test (sitting up) can easily exacerbate a patient’s symptoms because of the forces needed to perform the action. Assistance by the therapist might sometimes be necessary.
Types of LLD
LLD can be divided into three main groups:
1. Structural: This is an actual (or true) shortening of the skeletal system, typically caused by one of four things:
• Congenital defect, e.g. congenital dysplasia of the hip joint
• Surgery, e.g. total hip replacement (THR)
• Trauma, e.g. fractured femur or tibia
• Disease process, e.g. tumor, osteoarthritis, Osgood–Schlatter disease, or Legg–Calvé–Perthes disease
Fractured bones in children have been known to grow faster for many years after the healing process: this can naturally result in the limb becoming anatomically longer.
2. Functional: This can be a development from altered biomechanics of the lower body, such as ankle and foot over-pronation or supination, pelvic obliquity, muscle imbalances (as a result of, for instance, a weak Gmed and abdominals or tight adductors and hip flexors), hip or knee joint dysfunction, and even poor inner core stabilization, to name just a few.
3. Idiopathic: If there are obvious findings during the history taking and assessment process, the physical therapist may have an idea as to the cause of the patient’s LLD. However, if the therapist cannot ascertain a reason for the change in the presenting leg length, the condition would be classified as idiopathic, which means that it arises independently, not as a result of some other condition.
Kiapour et al. (2012) estimate that a LLD of as little as 0.4” (1cm) increases the load across the SIJ fivefold.

Figure 5.6. Left long-leg syndrome versus right short-leg syndrome.
Assessment
The therapist has to be very intuitive during the initial assessment. When placing their hands on top of the iliac crest of a patient in a standing position in order to ascertain pelvic obliquity, the therapist needs to be aware of a “pelvic shift” as the patient stands. Let me give you an example: if the patient has a weak Gmed muscle on the left side, the pelvis might appear to drop to the right side and deviate or laterally shift to the left; this will have the effect of the left iliac crest appearing elevated on that side (left), thus giving the natural appearance of a longer left leg.
When the patient presents to the clinic, one can assume that the pain has been present for a while; since the pain has persisted for an extended period of time we can safely say that the presenting condition is now in the chronic stage. Because of the natural overcompensatory mechanisms that occur through soft tissue chronicity, the postural muscles are probably held in a shortened and subsequently tight position; one particular lumbar spine muscle that has a natural tendency to shorten as a result of LLD is the QL. A perceived problem can arise when the patient lies on their back (supine position), so that you can observe the positions of the left and right medial malleoli when looking for any LLD. You may notice that the left medial malleolus appears nearer to the patient’s head (cephalic) than the one on the right, giving the appearance of a short left leg. This apparent shortness of the leg is possibly a result of a tight left QL muscle. When the patient was standing, however, you may have convinced yourself that the patient’s left leg actually looked longer!
This might seem initially confusing, but just think about it for a moment. Could it not simply mean (this is only one example because there are many potential causes of a higher iliac crest) that when the patient adopts a standing position the Gmed on the left side is weak, causing the pelvis to shift to the side of weakness, now giving the appearance of a longer left leg? Conversely, is it not possible that when the patient is in a supine position, the left QL is held in a shortened position, which is responsible for hitching up the pelvis, having the effect of pulling the leg closer to the head and thus making the left leg appear shorter?
The following phrase might help you remember this process:
“When you are standing, the weak muscles show themselves; when you are lying, the short muscles show themselves.”
Foot and Ankle Position
One of the most neglected aspects of the body, especially when patients present to the clinic, is the position of the lower limb. Every single day osteopaths, chiropractors, and physical therapists see lots of patients who initially present with lower back, pelvis, and sacroiliac pain. These specialist therapists naturally spend a lot of time observing and assessing the pelvis and lumbar spine to ascertain which tissue they personally consider to be responsible for giving the person the pain. This presenting pain may, however, just be a symptom, and the cause of the pain could be somewhere else, away from the actual site of the pain.
Dr. Ida Rolf, who invented the Rolfing soft tissue technique, states: “Where you think the pain is, the problem is not.” One of my popular sayings that I impress on my students (which I consider to relate to what Dr. Rolf states) is the following:
“The only person interested in the pain is your patient; you the therapist should try to find the actual cause of the pain and not simply treat where it hurts.”
It is very important that when assessing your patients, you should observe the position of the lower limb and in particular the foot and ankle complex, as a faulty foot and ankle structure can profoundly affect leg length and the natural position of the pelvis. The most common asymmetrical foot position that patients present with has to be what is commonly called an over-pronated foot (or pes planus), as shown in Figure 5.7.
It has been widely thought that when we actually present with a true LLD, the body will try to compensate for the longer leg through lowering the medial arch of the foot by pronating at the STJ. The action of pronation is called tri-planar motion and consists of three movements: dorsiflexion of the ankle, eversion, and abduction of the foot complex. The position of this increased pronation is basically the body’s natural compensatory mechanism to try to “shorten” the leg because it is anatomically longer.

Figure 5.7. Over-pronation syndrome.
The plantar surface of our feet has thousands of sensory receptors that are responsible for the position of the foot; the smallest shift in weight will be enough to signal the brain to induce a compensatory reaction. On the contralateral side (shorter leg), the compensatory mechanism will cause the medial arch to adopt a supinated position (tri-planar motion of plantar flexion, inversion, and adduction). The compensatory mechanism changes the position of the arch in an attempt to lengthen the apparent shorter leg. When physical therapists assess their patients they will need to check for this compensatory pattern, because, if left unchecked, excessive foot pronation caused by an anatomically longer leg (subsequent supination of the contralateral foot as compensation) will in turn cause an internal rotation of the lower extremity and an external rotation of the contralateral lower limb. This compensatory mechanism will then have the effect of altering the whole kinetic chain from the foot all the way up to the occiput.
True LLD and the Relationship to the Pelvis
Let’s continue with a “thought process” just for a moment. Now consider that your patient has an actual longer leg on the left side, which you have ascertained because of the higher position of the iliac crest and the possible compensatory pronation of the STJ on the same side, as well as the leg length appearing longer (through observation of the medial malleoli) in the supine and long sitting position. Before I continue with the discussion, just have a think to yourself about what position the innominate bone might be in if the left leg, say, is anatomically longer.
The innominate rotation will naturally be coupled with a LLD as a result of the compensatory mechanisms: if you look at Figure 5.8(a), you will see that the femoral head on the long-leg side forces the innominate into a superior and posteriorly rotated position. Conversely, the innominate on the low femoral head side drops down and anteriorly rotates, as shown in Figure 5.8(b). What we have now, therefore, is the left innominate being forced into a posterior rotation and the right innominate into an anterior rotation.
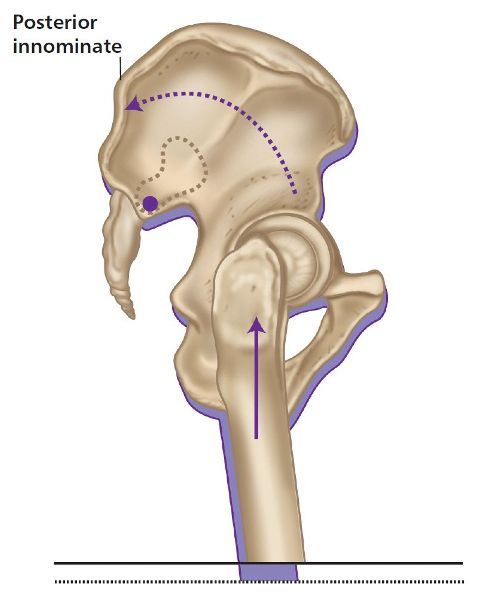
Figure 5.8. (a) Long-leg innominate compensation.
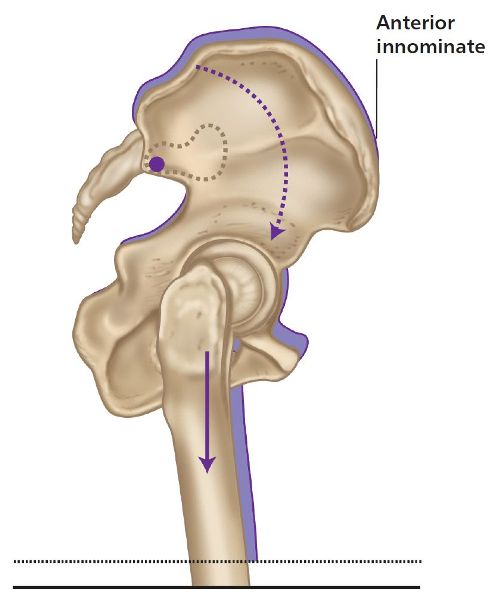
Figure 5.8. (b) Short-leg innominate compensation.
Think about what lies between the two innominate bones—yes, the sacrum. As a result of the compensatory rotation of both of the innominate bones (because of the anatomical LLD) in opposite directions to each other, a motion of the sacrum occurs—left-on-left (L-on-L) sacral torsion (Figure 5.9), which was covered in Chapter 2. Recall, a L-on-L sacral torsion means that the sacrum has rotated to the left on the left oblique axis and has side bent to the right, as it is ruled by Type I spinal mechanics (rotation and side bending are coupled to opposite sides, as established by Fryette (1918) and the law of spinal mechanics, which will be discussed in Chapter 6). This complexity of the innominate rotations that are coupled with a sacral torsion is usually depicted as a pelvic torsion, or even a pelvic obliquity, and will require a good understanding before a treatment plan is introduced.
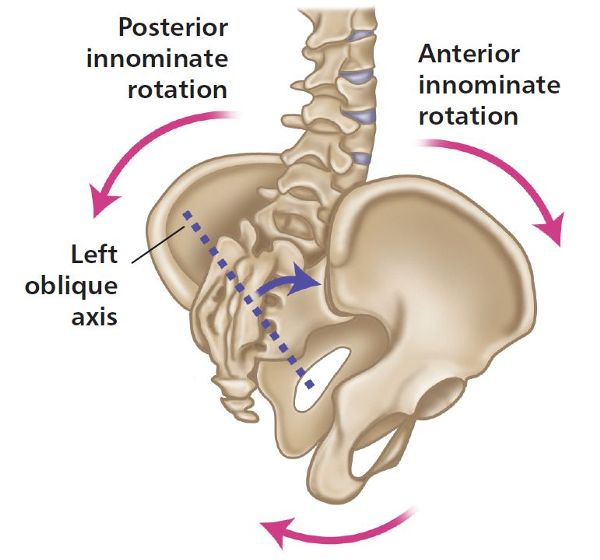
Figure 5.9. L-on-L sacral torsion.
True LLD and the Relationship Between the Trunk and the Head
You will notice in Figure 5.10(a) & (b) that on the left side there is a lower shoulder position on the high innominate side: this is a common finding in the case of a compensatory functional scoliosis. Some authors, however, have considered this to occur as a result of a “handedness pattern”: for example, if you are left handed, the left shoulder might appear to be lower, and if you are right handed, the right shoulder might appear to be lower. I agree that the pattern of handedness is probably true, but only if the iliac crests are level; otherwise some form of scoliosis has to exist, especially if the iliac crest and shoulder positions are asymmetric.
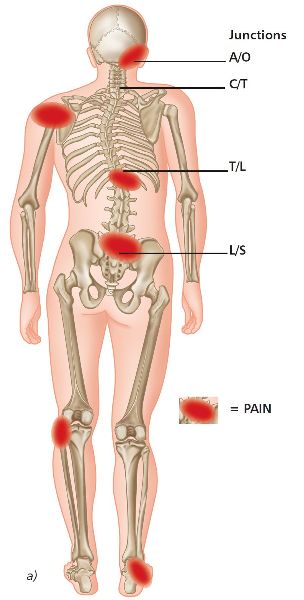
Figure 5.10. (a) Functional scoliosis compensation.
What else do you observe in Figure 5.10(b)? If you look at what is happening to the left QL, you might assume that this muscle is being held in a shortened position because of the higher left innominate. This assumption is correct, as you can also see that the lumbar spine is side bending toward the longer left leg (concavity) and rotating toward the shorter right leg (convexity).
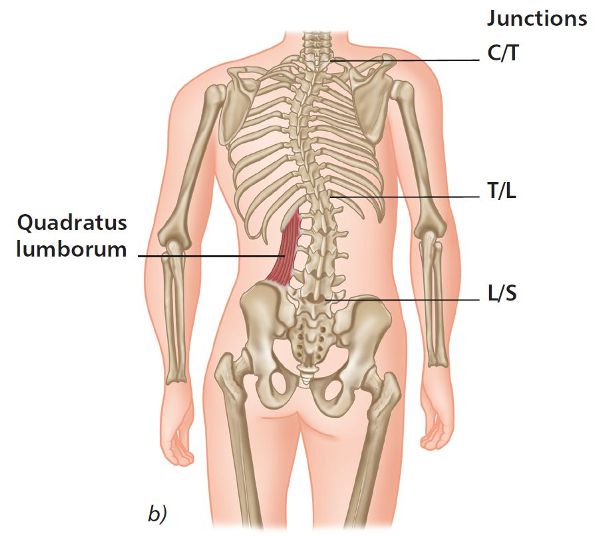
Figure 5.10. (b) Functional scoliosis compensation. Quadratus lumborum on left is short/tight.
As a result of the ascending functional scoliosis, the right shoulder is higher. You might also notice a short “C” curve in the cervical spine; this will probably cause the scalenes, sternocleidomastoid (SCM), upper trapezius, and possibly the levator scapulae muscles on the right side to adopt a shortened and subsequently tight position. This typical adaptation of muscular imbalance will help maintain an erect head position with the eyes level. The body will always want to be level no matter what and will do almost anything to accomplish this, through naturally adapting the position of the occipitoatlantal joint (OAJ), and in so doing can suffer enduring pain to maintain equilibrium. Common painful conditions that patients might present with are headaches, active trigger points, tinnitus, temporomandibular joint (TMJ) dysfunction, and even eye and facial pain.
LLD and the Gait Cycle
As we walk, if our gait cycle pattern has been altered because of an actual or an apparent LLD, the shorter leg will feel like it is stepping down, and the long leg will compensate by a sort of “vaulting” motion. It is almost like stepping into a small pothole with every step you take; imagine repeating this at least ten to fifteen thousand times a day—it will easily cause potential pain patterns of dysfunction! Common compensations are sometimes seen when patients are asked to walk: on the short-leg side, the patient might have a tendency to walk on their toes, and on the long-leg side, the patient may have a tendency to flex their knee, but this will depend on the discrepancy.
For the body to be an effective locomotor during the gait cycle, a well-aligned and symmetrical body is essential. When the positions of the innominate bones of the pelvis are altered by actual or apparent leg length discrepancies, it is easy to see how patients can present with pain, not only at the SIJ and lumbar spine but also everywhere else in their body that is going through a compensation pattern.
I mentioned earlier that there could be a weakness of the Gmed on one side of the body; this weakness could lead to a potential compensatory pattern for subsequent shortness issues with the tensor fasciae latae (TFL) and ITB on the other side. If there is weakness of the Gmed, the patient can have either a Trendelenburg pattern of gait or a compensatory Trendelenburg pattern of gait (see “Standing Balance Test,” later in this chapter). Whichever way you look at this, the patient is going to have an antalgic type of gait, which simply means that they will walk with some form of limp; this compensation can only cause one thing over time and that will simply be pain.
Summary of LLD Compensations to the Sacrum
• The sacrum typically rotates toward the long leg and side bends toward the short leg.
• A posterior sacrum (counter-nutation) has been found to be associated with same-side piriformis spasm.
• An anterior sacrum (nutation) has been found to be associated with same-side Gmed spasm.
Summary of LLD Compensations to the Lumbar Spine
• The lumbar spine typically rotates toward the side of the low sacral base/short leg and side bends toward the long leg.
• Facet pain due to compression is common on the concavity side (side-bending side) of the lumbar spine.
• The iliolumbar ligament can cause pain as it is stretched on the convex side of the lumbar spine and has been argued to refer pain to the groin, testicle, and medial thigh on the same side as the stretched ligament.
Summary of LLD Compensations to the Iliopsoas Muscle
• The iliopsoas muscle is generally considered to be tight on the side of the short leg. Note that a left iliopsoas muscle spasm can cause a pelvic side shift to the right, mimicking a shorter left leg.
• The iliopsoas muscle (iliacus in particular) can cause the innominate bone to compensate by rotating anteriorly on the side of the short leg, functionally causing a lengthening of that leg, while the innominate bone on the long side may do the opposite (posterior innominate rotation).
• Unilateral spasm (contraction) of the iliopsoas can create a lumbar concavity on the same side (because of side bending), with rotation to the opposite side, and potentially sets up a positive side shift on the side opposite to the spasm. It is important that the physical therapist always assesses for and treats iliopsoas spasm in the case of a suspected short leg or a positive pelvic lateral side shift.
• Iliopsoas spasm pain is generally worse on standing from a seated position, and less pain is perceived as the iliopsoas stretches out.
In summary, when looking at the level of the iliac crest, one has to determine if there is a LLD. If there is, one then has to ascertain if the dysfunction is a true discrepancy or a functional discrepancy, as the compensation pattern can change depending on the diagnosis. For example, if you find a true anatomical LLD, the innominate bone on the longer leg will normally try to compensate by rotating posteriorly, as seen in Figure 5.7 and explained earlier. Moreover, the femur and lower limb on the anatomically longer leg will follow the compensatory model by rotating medially, as seen in Figure 5.5, and the foot will try to pronate at the STJ, since the longer leg will attempt to shorten itself. At the same time, the actual shorter leg will compensate by supinating at the ankle mortise; this in effect can cause the tibia and femur to rotate externally and the innominate bone to rotate anteriorly as the leg tries to make itself appear longer.
Over-Pronation Syndrome
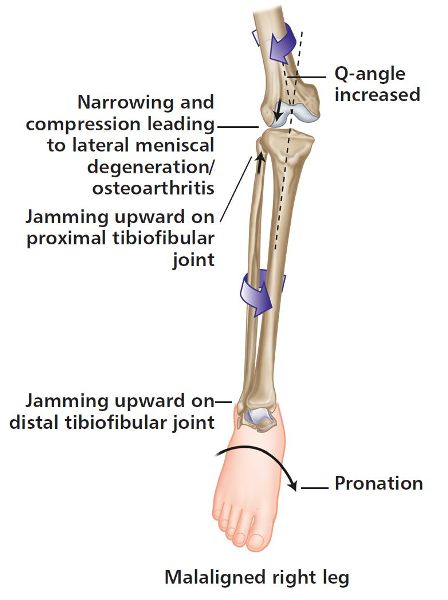
Let’s look at another compensation model for a patient who appears to have a LLD. In this case it is a functional LLD, and the apparent shorter leg of the patient exhibits an over-pronation of the STJ, rather than the true longer leg compensating by pronating to shorten itself. As a result, the body will try to compensate by causing an internal rotation of the tibia and femur, as shown in Figure 5.11(a); this will have the effect of the innominate bone rotating anteriorly (posteriorly in a true LLD, as explained earlier), which in turn can cause an increased lumbar lordosis with subsequent lower back pain.
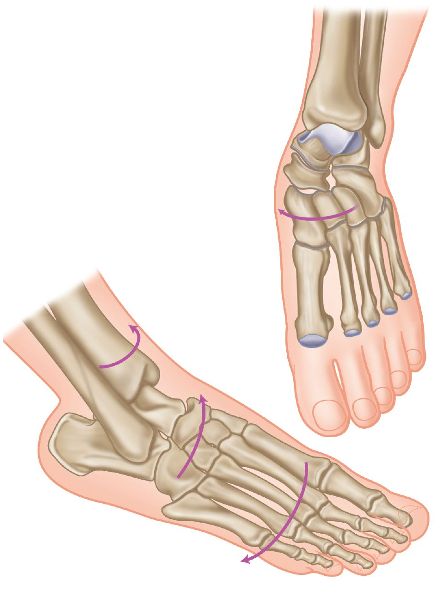
Figure 5.11. (a) A foot in over-pronation with internal tibial rotation.
According to podiatrists, over-pronation syndrome is a very common pattern found in the majority of people to some extent or another. It is best identified with the patient standing barefoot. The big clue is that one arch is lower or flatter than the other: the lower arch side is over-pronating. Sometimes, both sides may be over-pronating, but one side is generally over-pronating more than the other, or one side might be normal and the other side lower.
It is easy to confirm the condition by simply placing one finger under the patient’s arch, noting how much of your finger goes underneath, and comparing the result with the other side. Are they the same or different? If one side is noticeably lower than the other, you have found a patient with an over-pronation syndrome. Another test to confirm over-pronation is to observe the Achilles tendon from the posterior aspect: you will typically notice a bowing on the side with the lower arch.
It should be noted that over-pronation syndrome could originate not only from the foot and ankle but also from the innominate bone of that side. When the foot and ankle complex over-pronates, the innominate bone will normally rotate anteriorly. However, if we look at it the other way around, an anterior rotation of the innominate (common on the right side) can force the medial arch of the foot into an over-pronated position. This becomes a chicken and the egg situation, but that is irrelevant, as the only consideration is whatever presents itself now. In my experience, you might need to correct the innominate rotation and the over-pronation to help reduce the patient’s presenting symptoms.
If you feel the pronation is attributed to the most common presentation of a right anterior innominate rotation with a compensatory left posterior innominate rotation, then you might also notice the right foot appears to be in a position of relative external rotation or abduction, even though the tibia is still in a position of internal rotation because of the pronation of the STJ. This is possibly caused by the anticlockwise (left) rotation of the pelvis (compared with the left foot, which appears to be in supination and relative internal rotation or adduction). As mentioned earlier, even though the foot appears to be externally rotated, the tibia is still in an overall position of internal rotation, as shown in Figure 5.11(b).

Figure 5.11. (b) External rotation/abduction of the foot and ankle with STJ pronation, commonly found with a right anterior innominate rotation.
On the side that appears to be pronated with a relative external rotation or abduction of the foot (most common on the right side; the tibia is still maintained in an internally rotated position), the following musculoskeletal presentations are common:
• Medial collateral ligament and medial plica
• Groin and/or medial thigh pain
• Medial tibial stress syndrome (shin splints)
• Medial ankle ligaments sprain
• Posterior tarsal tunnel syndrome/posterior tibial nerve
• Compression of the sural nerve at the lateral ankle
• Increased Q angle (valgus) and stress to the lateral compartment of the knee
• Lateral tracking of the patella
• Plantar fasciitis
• Sesamoiditis
• Achilles tendinopathy
Figure 5.11. (c) Internal tibial rotation and ankle/foot with STJ pronation, commonly found with a right anterior innominate rotation.
On the side that appears to be supinated with a relative internal rotation or adduction of the foot as compared to the other side (common on the left side; the tibia is still maintained in an externally rotated position), the following musculoskeletal presentations are common:
• Strain to the hip abductors
• Greater trochanteric bursitis
• Lateral shin pain
• Lateral ankle ligaments sprain
• Nerve traction injury to the lateral femoral cutaneous and superficial peroneal nerves
• Increased pressure to the medial knee compartment due to varus position and decreased Q angle
• Traction of the lateral collateral ligament
• Tibial and metatarsal stress fractures
• Plantar fasciitis
• Morton’s neuroma
• Achilles tendinopathy
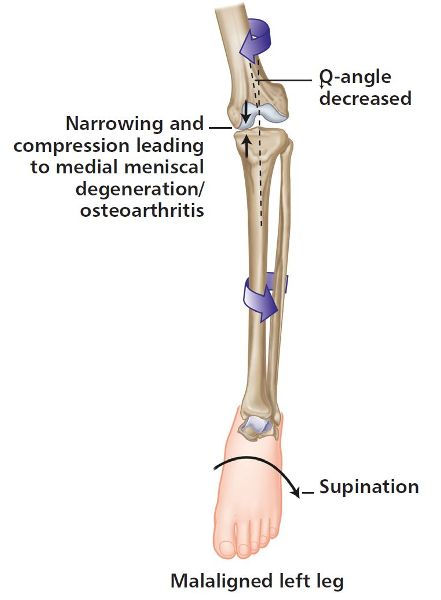
Figure 5.11. (d) External tibial rotation and ankle/foot with STJ supination, commonly found with a posterior innominate rotation.
You can see already that both compensatory mechanisms I have mentioned throughout this chapter have a pronation issue at the STJ; however, the true leg length compensation of the longer leg forced the innominate bone to rotate posteriorly, whereas the functional LLD of the over-pronation syndrome caused the innominate bone to rotate anteriorly.
You can probably gather from all the information above that there can be a lot going on at the same time throughout the kinetic chain; everything that has been mentioned can affect the length of the leg. It is correct to assume that this area of discussion is somewhat complex, and it might be difficult to know where to start in the assessment or even in the treatment program.
In all that has been discussed above, there lies a potential solution to the jigsaw puzzle of patients’ symptoms and dysfunctions. There exists what I call a key to unlocking the problem; the difficulty in physical therapy, however, is finding where to start and “insert the key” (excuse the expression). I can guarantee that, over the years, inexperienced therapists will have time and time again inserted the key into the wrong place, i.e. where the patient feels the pain and not where the problem lies. Recall the wise words of Dr. Ida Rolf!
During the practical components of my lectures to physical therapists attending my courses, I sometimes hear myself saying the following:
“Treat any dysfunctions that you find at the time during the treatment session, and the body will hopefully guide you onto the correct pathway.”
After that statement I normally say this:
“If, however, after three or even five physical therapy sessions, the patient’s symptoms are not reducing, then you the therapist will need to alter your thought process and reassess and potentially treat other areas of the patient’s body that you initially felt might not be related to the cause of their presenting symptoms.”
LLD and the Relationship to the Gluteal Muscles
So how does all this affect the glutes? When you have a compensation pattern, the femur not only rotates to compensate in the transverse plane (as explained earlier), but also experiences a compensatory mechanism of adduction and abduction in the frontal plane. Thus, in simple terms, if you have a lower limb that is held in an adducted position, then the abductor muscle group can be forced into a lengthened and subsequently weakened position, while the adductors will be held in a shortened and subsequently tight position. For a leg that is held in abduction, the situation is reversed.
If you look back at Figure 5.6 you will see that the left leg appears longer because of the higher left iliac crest, the innominate has rotated posteriorly, the femur has internally rotated, and the foot has pronated. In this compensation the left leg will be in a position of adduction (Figure 5.12), and consequently the right leg will be held in a position of abduction (Figure 5.13). This will have an effect on the musculature of the associated areas: some of these muscles will be held in a shortened position and some in a lengthened position.
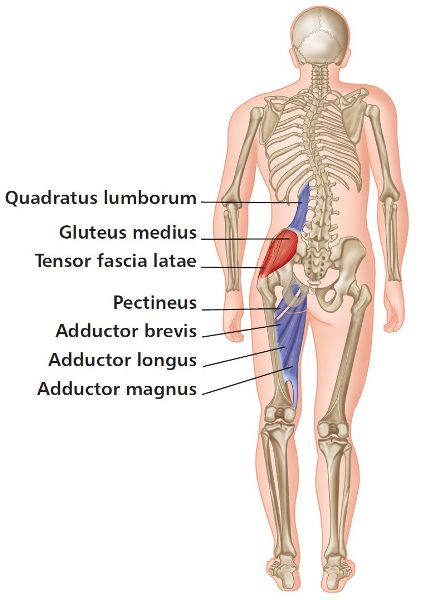
Figure 5.12. Left leg compensations—adductors and QL short and tight, with Gmed and TFL long and weak.
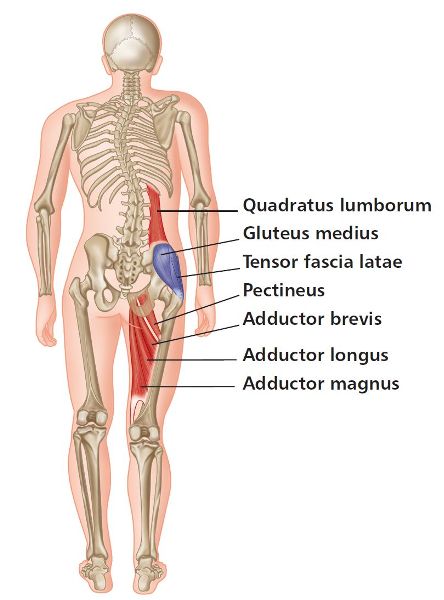
Figure 5.13. Right leg compensations—adductors and QL long and weak, with Gmed and TFL short and tight.
Standing Balance Test
When a patient is asked to stand on one leg and lift the opposite knee toward their waist, the physical therapist needs to observe the level of the PSIS as the patient transfers their weight to one leg. The patient should be able to shift their weight onto the stance leg (the right leg in Figure 5.14) with good muscular control of the Gmed of that leg. If the PSIS dips down on the leg that is being lifted (the left leg in Figure 5.15) rather than remaining level (Figure 5.14), it might be assumed that the Gmed on the opposite side (right side) is unable to control the movement; the patient might then have an altered pattern of gait when they go through the gait cycle, as shown in Figure 5.16. This altered gait pattern is called a Trendelenburg gait and is illustrated for a weak left Gmed in Figure 5.16. If this dysfunctional gait is present over a prolonged period, a compensatory Trendelenburg might develop, as shown in Figure 5.17. The reasons for this altered gait can be numerous to say the least, but one cause could be that one of the legs is held in an adducted position because of the shortening of the adductors (as mentioned above). This altered pattern will in turn result in a reciprocal inhibition (RI) to the antagonistic muscles: the abductors—in particular the Gmed—will now be held in a lengthened position that can then predispose the Gmed to becoming weak.
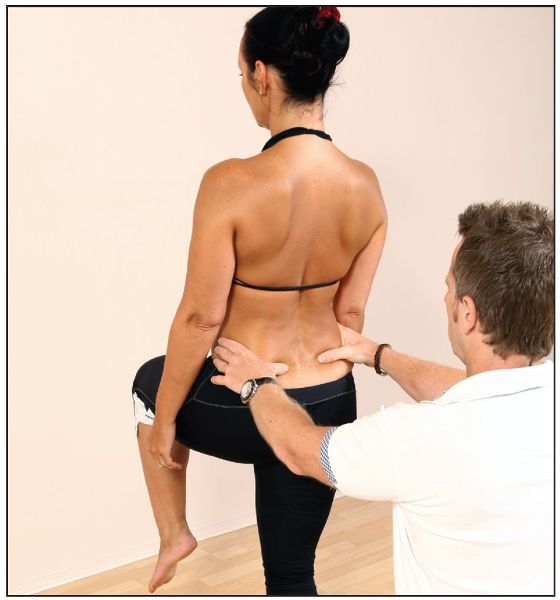
Figure 5.14. Standing balance test—normal.
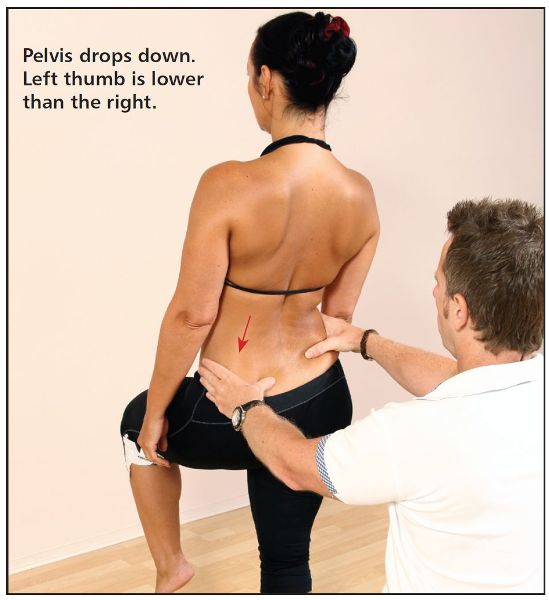
Figure 5.15. Positive test for weakness of the right Gmed—the left PSIS dips down on the left.

Figure 5.16. Trendelenburg gait—weak left Gmed.
When I teach the standing balance test (Figure 5.14), I say to my students that you need to look out for three things:
1. Position of the PSIS
The first, as I mentioned above, is the position of the PSIS as the patient transfers their weight from one leg to the other.
2. Shift of the pelvis
The second is how much movement occurs as the patient shifts onto the weight-bearing leg; you may notice one side shifting more than the other, indicating a possible Gmed weakness.
3. Stability on one leg
Finally, the third is how stable the patient is when they stand on one leg compared with the other. You will be amazed how many very fit athletes struggle to stand on one leg unaided and maintain good control. This instability could be a result of a weak Gmed, but remember also that a change in a patient’s ability to stabilize might be due to a previous injury/trauma to the ankle complex, thus affecting the neurological proprioceptors in controlling the specific position.
Friel et al. (2006) conducted a study about ipsilateral hip abductor weakness after an inversion ankle sprain; their results showed that hip abduction and plantar flexion were significantly weaker on the involved side. They concluded that unilateral ankle sprains led to weaker hip abduction (Gmed), and suggested exercises to strengthen the hip abductors when developing rehabilitation protocols for ankle inversion sprains.
Schmitz et al. (2002) demonstrated through an EMG study that there was an increase in Gmed activity during sudden ankle inversion motion in healthy subjects as well as in those with functionally unstable ankles.
Hopefully, after reading this chapter, you will have some understanding of what is happening when a patient presents with musculoskeletal dysfunctions, such as LLD, over-pronation syndrome, and muscle imbalances. In the next chapter I will continue with the journey on this theme by looking at the specific movement mechanics of the spine.