10
The Lumbar Spine and Its Relationship to the Pelvis
The aim of this chapter is to give the reader an insight into some of the skeletal pathologies that can manifest in the lumbar spine, as well as the potential underlying causes. Let me give you an example: a patient presents to your clinic with localized pain in the muscles of the lumbar erector spinae. On examination you find that the right innominate bone is fixed in an anteriorly rotated position (the most common), which could be caused by an overactivation and subsequent shortness of the right iliopsoas and rectus femoris muscles (as demonstrated in Chapter 7 by the modified Thomas test). The origin of the rectus femoris muscle is on the AIIS of the ilium; because of this attachment, the muscle can naturally “pull” the innominate bone in an anterior and inferior direction. This fixed anterior position of the innominate can cause an inhibition (switching-off) weakness in the right Gmax and was explained in more detail in Chapter 9.
If the Gmax becomes inhibited because of the anteriorly rotated position of the right innominate bone, it will not be able to provide the correct activation sequence when a hip extension action is demanded by the patient (e.g. in walking or running); the lumbar spine erector muscle will be one of many areas that will start to overcompensate for this inhibition weakness of the Gmax (see Chapter 9). In time, an overcompensatory mechanism of the lumbar spine erector musculature in particular will cause the patient to feel tightness in the lower back, as well as potential pain.
There are many different options for treating this particular pelvis dysfunction. One way (and which works very well for me personally) is to utilize a soft tissue method, namely an MET, to normalize the iliopsoas and rectus femoris (this technique is demonstrated in Chapter 7 on METs), in addition to performing a specific MET to correct the anterior position of the innominate (see Chapter 13 on treatment of the pelvis). After having normalized both the muscles and the innominate, you would retest the Gmax firing; if the Gmax is still inhibited, a corrective firing pattern sequence can be initiated to promote the reactivation of the glutes. (For more information on glutes activation and correction, the reader is referred to Gibbons (2014).)
It would be logical to first correct (see Chapters 11 and 12) any/all of the pelvis dysfunctions (iliosacral, sacroiliac, and symphysis pubis) that are found, before continuing, assessing, and treating dysfunction of the lumbar spine (unless the spinal rotation is the primary dysfunction). Perhaps think about why I say this, before reading any further.
Hopefully, you will come to the conclusion that it is essential to address any issues with an underpinning structure before tackling problems in other areas that depend on that structure. For example, I regard the pelvis as being similar to the foundations that are laid before building a house; we would not want to build on top of the foundations if they were not level. I try to use the same analogy when I look at and assess the lumbar spine area. If the pelvis is not level to start with, then the lumbar spine cannot be level either; this area of the spinal column will therefore automatically compensate in some way through changing its natural spinal curvatures, which could result in functional/structural scoliosis. This unnatural positional change to the lumbar spine as a compensation mechanism can only lead to one thing, and you will easily guess what that is—pain, of course!
I am convinced that most of the spinal pathologies discussed in this chapter are a direct or indirect consequence of the overall position and stability integration of the pelvic girdle. It is very difficult, however, to prove this, especially since I haven’t been able to find any recent clinical research to back up what I am saying. What I have stated has to be correct in one way or another, however, because the fundamental foundation (i.e. the pelvis) must be the main area of compensation for all of the various types of dysfunction that might be present within the body; this will have a direct knock-on effect on the entire kinetic chain, and the lumbar spine is clearly part of that compensatory chain mechanism.
Let’s be a little realistic here for a moment. By the time a patient who presents with what might be diagnosed as a specific or non-specific back pain comes to see you, they probably already have some spinal pathology present. The patient might also have had confirmation of their spinal pathology by an MRI scan, X-ray, or some other diagnostic measures. Put simply, what I am saying in the above statement is therefore the following: the patient’s presenting spinal pathology already exists, even before they walk through your clinic door!
Of the thousands of patients I have seen as a practicing sports osteopath and sports therapist, I can probably count on one hand those who have consulted me for an initial osteopathic assessment and treatment to actually prevent the onset of spinal and pelvic pathology, or indeed any other structural and soft tissue ailment. Let me reiterate what I mean by that. I believe that 99.9% of the patients and athletes who have visited my clinic already have a presentation of symptoms of pain/dysfunction somewhere in their body, and more than likely have some underlying form of spinal or pelvic dysfunction/pathology already present—and this is even before we have been formally introduced.
Lumbar Spine Anatomy
There are five individual spinal segments that make up the lumbar vertebrae, and each vertebra comprises the following structures (Figure 10.1):
• Vertebral body
• Spinous process
• Transverse process (TP)
• Superior/inferior facet joint
• Intervertebral foramen
• Spinal canal
• Lamina
• Pedicle
• Intervertebral disc: nucleus pulposus/annulus fibrosus
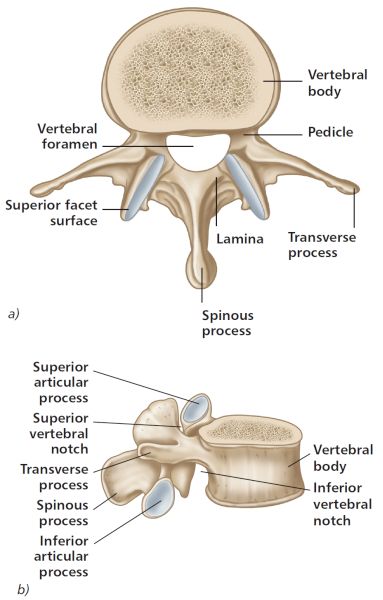
Figure 10.1. General anatomy of a lumbar vertebra (L3); a) superior view, b) lateral view.
Intervertebral Discs
Between adjacent lumbar vertebrae there is a structure known as an intervertebral disc; in total we have 23 of these soft tissue structures in the human vertebral column. A disc is made up of three components: a tough outer shell, called the annulus fibrosus; an inner gel-like substance in the center, called the nucleus pulposus; and an attachment to the vertebral bodies, called the vertebral end plate. As we get older, the center of the disc starts to lose water content, a process that will naturally make the disc less elastic and less effective as a cushion or shock absorber.
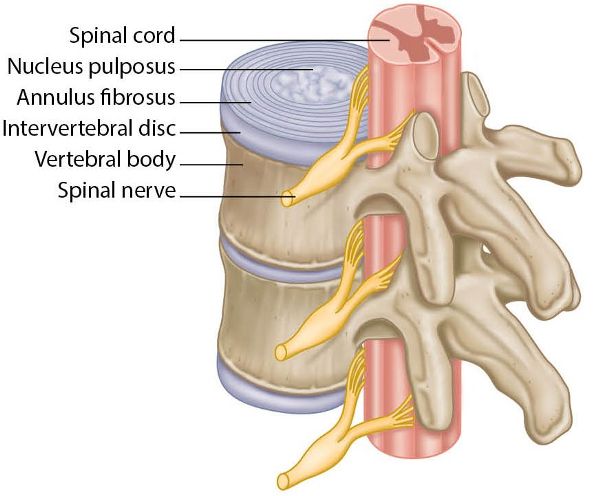
Figure 10.2. Anatomy of the lumbar spine and the intervertebral discs.
Nerve roots exit the spinal canal through small passageways between the vertebrae and the discs: such a passageway is known as an intervertebral foramen. Pain and other symptoms can develop when a damaged disc pushes into the spinal canal or nerve roots—a condition commonly referred to as a herniated disc.
Disc Herniation
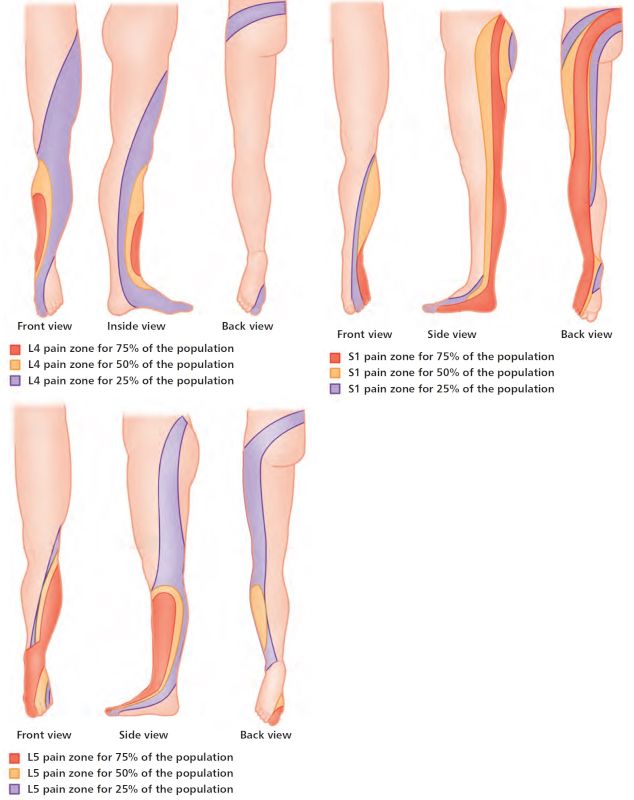
Herniated discs are often referred to as bulging discs, prolapsed discs, or even slipped discs. These terms are derived from the nature of the action of the gel-like content of the nucleus pulposus being forced out of the center of the disc. Just to clarify, the disc itself does not slip; however, the nucleus pulposus tissue that is located in the center of the disc can be placed under so much pressure that it can cause the annulus fibrosus to herniate or even rupture, as shown in Figure 10.3. The severity of the disc herniation may cause the bulging tissue to press against one or more of the spinal nerves, which can cause local and referred pain, numbness, or weakness in the lower back, leg, or even ankle and foot. Approximately 85–95% of lumbar disc herniations will occur either at the lumbar segments L4–L5 or at L5–S1; the nerve compression caused by the contact with the disc contents will possibly result in perceived pain along the L4, L5, or S1 nerve root pathway, as shown in Figure 10.4.

Figure 10.3. Disc herniation.
Degenerative Disc Disease
Degenerative disc disease (DDD) tends to be linked to the aging process and refers to a syndrome in which a painful disc can cause associated chronic lower back pain, which can radiate to the hip region. The condition generally occurs as a consequence of some form of injury to the lower back and the associated structures, such as the intervertebral discs. A sustained injury can cause an inflammatory process and subsequent weakness of the outer substance of the disc (annulus fibrosus), which will then have a pronounced effect on the inner nucleus pulposus. This reactive mechanism will create excessive movement, because the disc can no longer control the motion of the vertebral bodies that are located above and below the disc. This excessive movement, combined with the natural inflammatory response, will produce chemicals that will irritate the local area, which will commonly produce symptoms of chronic lower back pain.
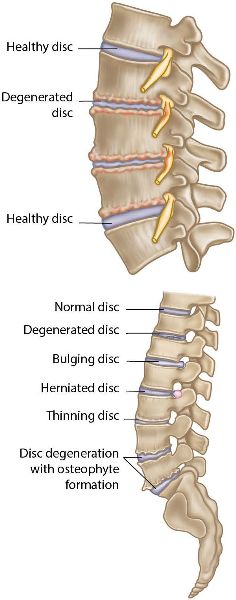
Figure 10.5. Degenerative disc disease (DDD).
DDD has been shown to cause an increase in the number of clusters of chondrocytes (cells that form the cartilaginous matrix and consist mainly of collagen) in the annulus fibrosus (consisting of fibrocartilage). Over a prolonged period of time the inner gelatinous nucleus pulposus can change to fibrocartilage, and it has been shown that the outer annulus can become damaged in areas that allow some of the nucleus material to herniate through, causing the disc to shrink and eventually leading to the formation of bony spurs called osteophytes.
Unlike the muscles in the back, the discs of the lumbar spine do not have a natural blood supply and therefore cannot heal themselves; the painful symptoms of DDD can therefore become chronic, eventually leading to further problems, such as discal herniation, facet joint pain, nerve root compression, spondylolysis (defect of the pars interarticularis), and spinal stenosis (narrowing of the spinal canal).
Facet Joints
Located within the lumbar spine are the facet joints (anatomically known as the zygapophyseal joints); these structures can be responsible for provoking a lot of pain. The facet joints lie posterior to the vertebral body, and their role is to assist the spine in performing movements such as flexion, extension, side bending, and rotation. Depending on their location and orientation, these joints will allow certain types of motion but restrict others: for example, the lumbar spine is limited in rotation, but flexion and extension are freely permitted. In the thoracic spine, rotation and flexion are freely permitted; extension, however, is limited by the facet joints (but also by the ribs).
Each individual vertebra has two facet joints: the superior articular facet, which faces upward and works similarly to a hinge, and the inferior articular facet located below it. The L4 inferior facet joint, for example, articulates with the L5 superior facet joint.
Like all other synovial joints in the body, each facet joint is surrounded by a capsule of connective tissue and produces synovial fluid to nourish and lubricate the joint. The surfaces of the joint are coated with cartilage, which helps each joint to move (articulate) smoothly. The facet joint is highly innervated with pain receptors, making it susceptible to producing back pain.
Facet Joint Syndrome/Disease
Facet joints have a tendency to slide over each other, so they are naturally in constant motion with the spine; like all types of weight-bearing joint, they can simply wear out and start to degenerate over time. When facet joints become irritated (the cartilage can even tear), this will cause the bone of the joint underneath the facet joint to start producing osteophytes, leading to facet joint hypertrophy, which is the precursor of facet joint syndrome/disease (Figure 10.6) and eventually leads to a condition called spondylosis. This type of syndrome or disease process is very common in many patients presenting with ongoing chronic back pain.

Figure 10.6. Facet joint syndrome and spondylosis.
Lumbar Spine as a Cause of Pelvis Dysfunctions
I have mentioned on numerous occasions the concept of the pelvis and possibly the hip joint being the key areas that are responsible for the presentation of pain in the lumbar spine and pelvic girdle regions. However, there have to be certain times (and, of course, there are) that some other structures (apart from those already mentioned) might need to be incorporated into the bigger picture in order to solve the problem; the structures that I am going to talk about might actually play an even greater role. Once you understand the next concept, I hope it will help you to place the jigsaw puzzle pieces in the correct sequence, so that a clearer picture will begin to appear.
It could be that the underlying issue is hidden and dormant and not showing itself as a dysfunction: the musculoskeletal problem is lying quietly in the grass and minding its own business. Let’s consider for a moment the possibility that the problem is actually within the lumbar spine, and this structure could be the key to solving the mystery, as well as being the main reason for maintaining the pelvic dysfunctions.
For example, a patient has ongoing recurrent pelvic dysfunctions that you have been correcting time and time again to no avail; you constantly feel as if you are banging your head against the wall, because what you are doing (in terms of treatment) does not seem to be the key to solving the problem, whereas it might have been with other patients you have treated in the past. The problem potentially lies within the lumbar spine, and it is this skeletal structure that is the underlying causative factor maintaining and controlling the ongoing dysfunctional pelvic pattern. If there is a rotational component at the lumbosacral junction (L5/S1), this has been recognized as one of the causes of recurrent pelvic malalignment.
Let’s look at an example where the lumbar spine is the root cause. If we have a clockwise rotation (i.e. to the right) of the 5th lumbar vertebra (L5), the right-sided TP will rotate backward (posteriorly). There are soft tissue attachments onto the L4 and L5 TPs for the iliolumbar ligament, and this ligamentous tissue attaches directly to the iliac crest. The induced rotation increases the tension within the iliolumbar ligament, and also the L5 rotation to the right will force the right innominate to rotate posteriorly; the left TP of L5 is rotating anteriorly and this creates an anterior position (anterior rotation) of the left innominate (Figure 10.7). Farfan (1973) reasoned that the shorter the TP, the longer the iliolumbar ligament and the greater the torsional force.
The L5 right inferior facet will be in a relatively open position on the superior facet of the 1st sacral vertebra (S1); the left inferior facet, however, will be in a closed position on the superior facet of S1. If the left facet joint is compressed, and the position is maintained and continued, it can now become a pivot point (fulcrum). This fixation (left) of the L5/S1 facet joint will now start to encourage the sacrum to rotate to the right axis (R-on-R), which will eventually force the whole pelvis unit into a right rotated position, as shown in Figure 10.7.
So how do we go about correcting a dysfunction of the lumbar spine? Well, the assessment of the pelvis in Chapter 12 contains snippets of valuable information that will help you ascertain if a lumbar dysfunction exists. Once you have read and understood how to determine a lumbar dysfunction in your patient, you will then need to read the appropriate text in Chapter 13, which explains in detail how to correct any possible dysfunctions that may be found within the lumbar spine complex.
Note: I would still recommend that you first treat any pelvic dysfunctions, before embarking on realigning specific dysfunctions that you find within the lumbar spine complex.

Figure 10.7. Rotational effect of L5 on the sacrum and on the innominate (via the attachment to the iliolumbar ligament).