9
The Gluteal Muscles and Their Relationship to the Pelvis
This book is obviously focused on the pelvic girdle and the sacroiliac joint; however, I think I ought to mention the role of the glutes in this text, as these specific muscles are a core component of the overall function and stability of the pelvic girdle.
The objectives of this chapter are to look at the specific relationship of the gluteal muscles to the area of the pelvis, and how any dysfunction that might be present within the pelvic girdle can cause a misfiring or potential weakness inhibition of the activation of the gluteal musculature.
For this chapter I will concentrate on the anatomy, function, assessment, and relationship to the pelvis of only the gluteus medius (Gmed) and gluteus maximus (Gmax) muscles.
Gluteus Medius (Gmed)
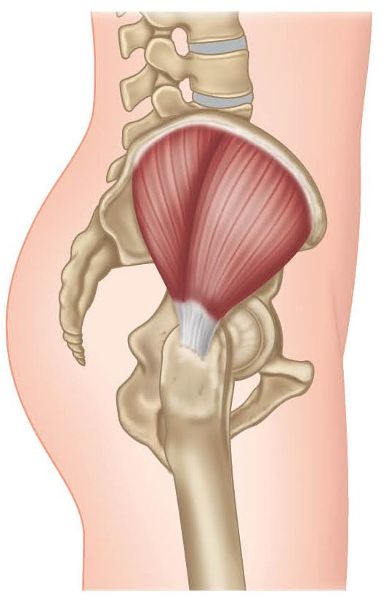
Figure 9.1. Origin, insertion, action, and nerve innervation of the Gmed.
Function of the Gmed
If you think back to Chapter 4 just for a moment, you may recall that when we initiate standing on one leg, we activate what is called the lateral sling system; as already explained, this system consists of the Gmed, Gmin, adductors on the ipsilateral side (same side), and the QL on the contralateral side (opposite side), as shown in Figure 9.2.
Potential weakness in the Gmed probably results from the overactivation of other muscles, because of the compensation process (which will be discussed below). Patients who present with weakness in their Gmed, particularly in the posterior fibers, tend to have overactive adductor muscles and ITB through the connection with the TFL; the piriformis can also play an overactive role if the Gmed posterior fibers are shown to be weak.
The Gmed is thought of as the muscle that is key to dynamic pelvic stability. For example, in my experience, patients who like to run for pleasure, or even competitively, and who have poor dynamic pelvic stability because of a possible weakness of the Gmed, will tend to shorten their stride length; they will adopt a more shuffling type of pattern, thereby reducing the ground reaction force at heel contact and decreasing the amount of muscle control required for maintaining pelvic posture.
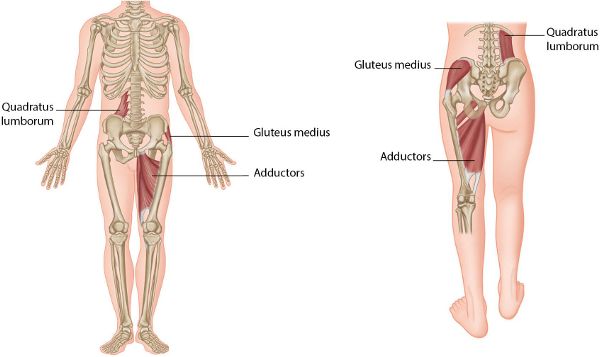
Fig 9.2. (a) Lateral sling system. (b) Lateral sling muscles activated during the gait/walking cycle.
Assessment of the Gmed
Whenever I look at patients who present with knee, lower lumbar spine, or pelvic pain, part of my assessment process includes checking the strength of the gluteal muscles and in particular the Gmed. In this chapter, as well as discussing the functional roles of this muscle and the Gmax and their relationships to the pelvis, I will also include the hip abduction and hip extension firing pattern tests, which are used for determining the correct muscle firing sequences of the hip abductors/extensors (including the Gmed/Gmax muscles).
In my opinion, the Gmed (and also the Gmax) should be assessed for every single patient and athlete who presents with pain in the areas of the lumbar spine and pelvis, and even in the lower and upper limbs. Many athletes present to my clinic with running-related overuse types of injury to the lower limb as well as to the trunk, and the majority of them also present with what I consider to be poor Gmed or Gmax (or both) function. I have come to the conclusion that the strength and control of these muscles is probably the most important overall component in achieving a biomechanically efficient pattern, especially in sports like running. This is not so surprising when you consider that during running you are always either completely in the air or dynamically balanced on one leg. All physical therapist practitioners should be able to assess and restore the function of both the Gmed and the Gmax.
Let’s take a closer look at the anatomy of the Gmed: the muscle attaches to the entire length of the iliac crest, to the external ilium between the posterior and anterior gluteal lines, to the gluteal fascia, to the posterior border of the TFL, and to the overlying ITB. The Gmed is divided into three distinct portions—anterior, middle, and posterior—which collectively form a broad conjoined tendon that wraps around, and inserts onto, the greater trochanter of the femur. The more vertical anterior and middle portions of the Gmed appear to be in a better position for abducting the hip than the more horizontal posterior portions.
As mentioned above, the Gmed contains a posterior fiber component in its structure as well as an anterior component; it is the posterior fibers that we as therapists are concerned with. The Gmed posterior fibers work in conjunction with the Gmax, and these two muscles in particular control the position of the hip into an external rotation, which helps to align the hip, knee, and lower limb as the gait cycle is initiated.
As an example, consider a patient who is asked to walk while the therapist observes the process. When the patient puts their weight on their left leg at the initial contact phase of the gait cycle, the Gmed is responsible in part for the stability mechanism acting on the lower limb; this will also assist in the overall alignment of the lower limb. The patient continues with the gait cycle and now enters the stance phase. Contraction of the left Gmed in this phase of the gait cycle is responsible in part for allowing abduction; think of it as a hitching type of motion to the right hip, even though the left Gmed is contracting. The right side of the hip is then seen to start to lift slightly higher than the left side. This process is very important, as it allows the right leg to lift a small distance off the floor and will naturally allow the swing motion of the right leg during the swing phase of the gait cycle.
If there is any weakness in the left Gmed, the body will respond in one of two ways during the gait cycle: either the pelvis will tip down on the contralateral side to the stance leg (right in this case), giving the appearance of a Trendelenburg pattern of gait (Figure 9.3(a)); or a compensatory Trendelenburg pattern will be adopted, in which the patient will be observed to shift their whole trunk excessively to the weaker hip (Figure 9.3(b)).
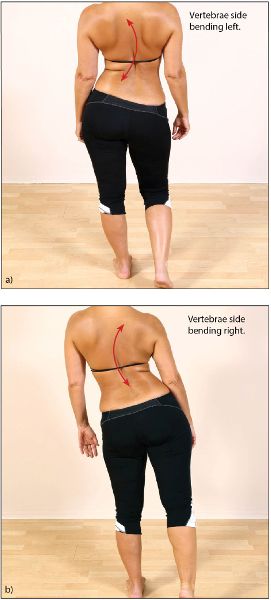
Figure 9.3. (a) Trendelenburg gait. (b) Compensatory Trendelenburg gait.
Gmed weakness will not only have implications for the overall stability of the pelvic girdle and lumbar spine, but also have an effect all the way down the kinetic chain, from heel contact to the mid-stance phase. A weakness of the Gmed can cause:
• Trendelenburg or compensatory Trendelenburg pattern of gait
• Lumbar spine pathology and sacral torsions
• Hypertonicity in the contralateral (opposite side) QL
• Hypertonicity in the ipsilateral (same side) piriformis and TFL muscles and the ITB
• Excessive adduction and internal rotation of the femur
• Drifting of the knee into a valgus or possibly varus position, causing a patella mal-tracking syndrome
• Internal rotation of the lower limb (tibia), relative to the position of the foot
• Increased weight transfer to the medial aspect of the foot
• Excessive pronation of the subtalar joint (STJ)
As you can see from the above list of consequences of a weakness in the function of the Gmed, an athlete/patient is at continual risk of any sports-related injury condition that is somehow caused by increased side bending/rotation of the lumbar spine (potentially because of Trendelenburg gait patterns), as well as by other biomechanical effects to the kinetic chain. An increased lumbar motion of side bending, coupled with rotation (normally to the opposite side), will subsequently cause the sacrum to rotate and side bend in directions opposite to the motion of the lumbar spine; as a result, a forward sacral torsion might now exist, for example a L-on-L or a R-on-R, as explained in Chapter 2.
The weakness of the Gmed can also cause prolonged over-pronation of the STJ, resulting in conditions such as patellofemoral pain syndrome, medial tibial stress syndrome (shin splints), plantar fasciitis, or Achilles tendinopathy.
Hip Abduction Firing Pattern Test
To check the firing sequence on the left side, the patient adopts a side-lying posture with both legs together and their left leg on top. In this sequence, three muscles will be tested: Gmed, TFL, and QL. The therapist palpates the QL muscle by placing their right hand lightly on the muscle. Next, to palpate the Gmed and TFL, the therapist places their finger on the TFL and their thumb on the Gmed, as shown in Figures 9.4(a) and (b).
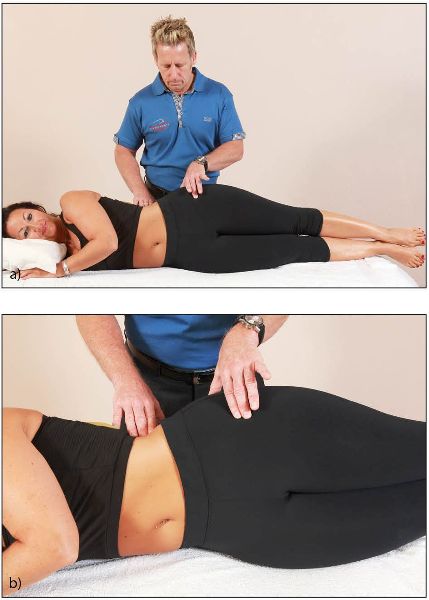
Figure 9.4. (a) Palpation of the QL, Gmed, and TFL. (b) Close-up of the hand position.
The patient is asked to lift their left leg into abduction, a few inches from their right leg, while the therapist notes the firing sequence (Figure 9.5). It is important to check for any compensatory or cheating recruitment. The idea of this test is that the patient must be able to abduct their hip without: (1) hitching the left side of their pelvis (hip hitching would mean they were activating the left QL muscle); (2) falling into an anterior pelvic tilt; or (3) allowing their pelvis to tip backward.

Figure 9.5. As the patient abducts their left hip, the therapist notes the firing sequence.
The correct firing sequence should be Gmed, followed by TFL, and finally QL at around 25 degrees of pelvis elevation. If the QL or the TFL fires first, this indicates a misfiring sequence, potentially resulting in adaptive shortness of these muscles.
Once we have ascertained the firing sequence for hip abduction, we have to decide on the next step. Most patients feel that they need to strengthen the weak Gmed muscle by going to the gym, especially if they have been told this muscle is weak, and they do lots of side-lying abduction exercises. The difficulty in strengthening the apparent weak Gmed muscle is that this particular exercise will not, I repeat not, strengthen the Gmed, especially if the TFL and QL are the dominant abductors. The piriformis will also get involved, as it is a weak abductor, which can cause a pelvic/sacroiliac dysfunction, further complicating the underlying issue.
So the answer is to initially postpone the strengthening of the Gmed and focus on the shortened/tight tissues of the adductors, TFL, and QL. In theory, by lengthening the tight tissues through METs as explained in Chapter 7, the lengthened and weakened tissue will become shorter and automatically regain its strength. If, after a period of time (two weeks has been recommended), the Gmed has not regained its strength, specific and functional strength exercises for this muscle can be added.
Gmed “Anterior Fibers” Strength Test
To test the anterior fibers of the left Gmed, the patient adopts a side-lying posture with their left leg uppermost. The therapist palpates the patient’s Gmed with their right hand, and the patient is asked to raise their left leg into abduction, a few inches away from the right leg, and hold this position isometrically to start with. Placing their left hand near the patient’s knee, the therapist applies a downward pressure to the leg. The patient is asked to resist the pressure (Figure 9.6); if they are able to do so, the anterior fibers of the Gmed are classified as normal.
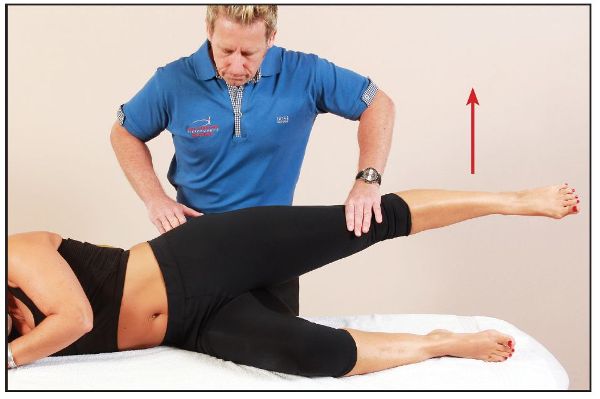
Figure 9.6. The patient abducts their left hip against resistance from the therapist.
Gmed “Posterior Fibers” Strength Test
In testing the left side, to put more emphasis on the posterior fibers of the Gmed, the therapist controls the patient’s left hip into slight extension and external rotation, as shown in Figure 9.7. The therapist applies a downward pressure as before (Figure 9.8); if the patient is able to resist this external force, the Gmed posterior fibers are classified as normal. If you want to assess muscular endurance as opposed to strength, ask the patient to hold the abducted leg and maintain the position for at least 30 seconds.
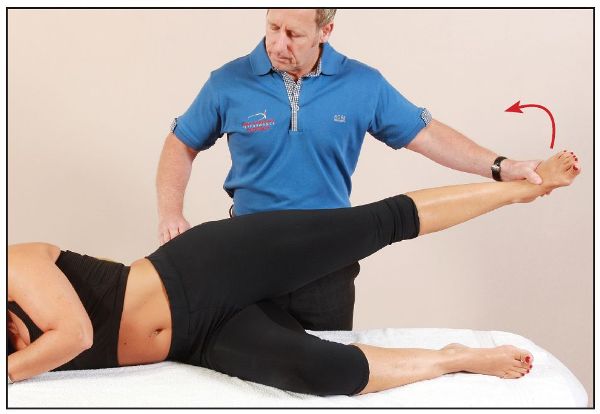
Figure 9.7. External rotation and slight extension of the hip, which emphasizes the posterior fibers of the Gmed.
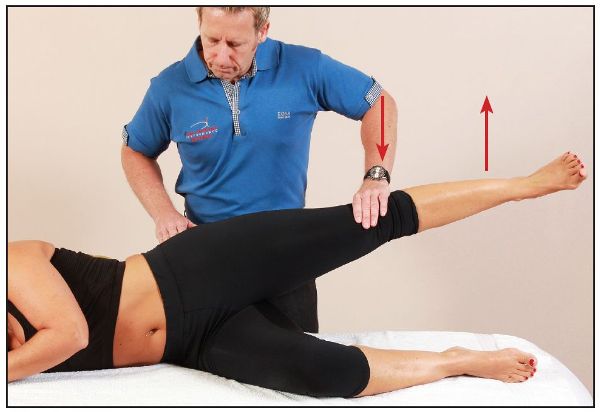
Figure 9.8. The therapist applies a downward pressure to the patient’s abducted hip.
Recall, from the earlier discussion of the role of the Gmed during the gait cycle, that a weakness of the Gmed can cause either a Trendelenburg or a compensatory Trendelenburg pattern of gait. Think about this, and the possible consequences of this weakness, for a second! As you step onto your left leg, the lateral sling has to come into play: the left Gmed is the main muscle responsible for the control of the height of the right side of the pelvis as you try to stabilize on the left leg. If the Gmed muscle on the left is weak, the pelvis will dip (to the right) as you bear weight. The dipping action will typically cause the lumbar spine to side bend (to the left) and rotate to the right (Type I spinal mechanics) and the facet joints on the left side, as well as the intervertebral disc and the exiting nerve root, to compress, resulting in pain. This side bending motion to the left can also cause the iliolumbar ligament on the right side of the spine, as well as other structures such as the joint capsule of the facet joints, to be placed in a stretched position, which can also be a source of pain (local or referred).
I also mentioned sacral torsion earlier—if the left Gmed muscle is weak, then because of the side bending of the lumbar spine to the left and rotation to the right, the effect will be to cause an opposite motion to the sacrum; thus, the sacrum will side bend to the right and rotate to the left, as in a L-on-L sacral torsion.
Let’s look at another example. If the left Gmed is weak, the opposite (right) side QL will compensate and work harder as it tries to take on the role of the weak muscle. This increased compensatory pattern will over time cause an adaptive shortening of the right QL, which can result in the formation of trigger points and subsequently lead to pain.
Case Study
Consider the following scenario: a patient presents to the clinic with pain located in the right lower side of their lumbar spine/superior ilium (QL area), which is exacerbated especially by walking/running for a certain length of time. After palpating the right side of the patient’s lower back/QL area, the physical therapist says the muscle is tight and proceeds to release the trigger points that might have developed within. A contract/relax type of technique, such as an MET, might then be used to encourage normality of the length of the QL. The patient and therapist are very happy with the treatment, as most of the presenting symptoms have now subsided. However, as the patient walks the 10-minute journey back to their car the QL pain resumes—why? Because a weak left Gmed is forcing the right QL to work a lot harder than it has been designed to do, and the therapist has only treated the presenting symptoms and not the underlying cause! Remember the wise old words of Dr. Rolf—where the pain is, the problem is not!
Please note that any pelvic dysfunction found in your patient or athlete (as outlined in Chapter 12) can also be one of the main underlying causative factors for the presentation of a weakness/inhibition of the gluteal musculature. The malalignment position of the pelvis can be the key to the problem, as this dysfunction can naturally induce an overcompensatory mechanism in other muscles of the body. This is because the altered pelvic position can now cause a misfiring sequence in the specific activation of the gluteal muscles, rather than these muscles simply being weak and misfiring because of the antagonistic muscles being held in a shortened and tightened position.
In terms of treatment, this suggests that the gluteal muscles will not resume their normal firing sequence capability, or even develop their inherent strength, until the pelvis has been realigned. One might find that the gluteal muscles resume their normal firing sequence and regain their strength simply by realigning the position of the pelvis. After the correction of the pelvic girdle, it is recommended to lengthen the antagonistic muscles (but only if you feel it is still appropriate), before promoting strength-based exercises for these muscles.
Let’s quickly recap the above. The first thing I suggest is to correct any presenting pelvic dysfunctions (Chapter 13). Next, if you still find short antagonistic muscles, I would suggest lengthening these through METs (Chapter 7). Finally, I recommend simple strength-based outer core exercises, to encourage and maintain the realigned position of the pelvis (Chapter 3).
Gluteus Maximus (Gmax)
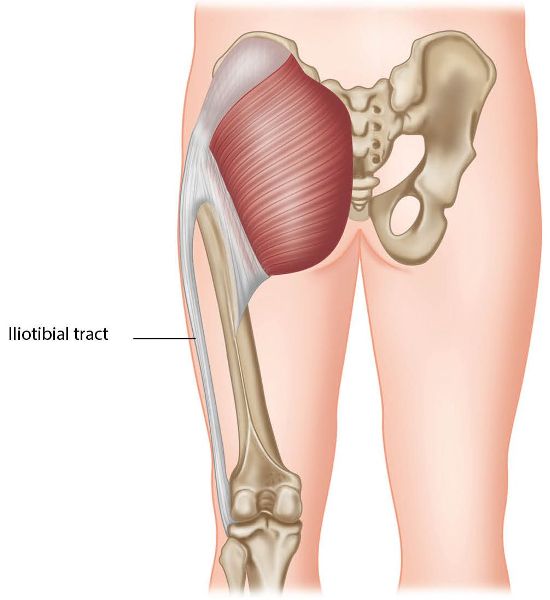
Figure 9.9. Origin, insertion, action, and nerve innervation of the Gmax.
Function of the Gmax
From a functional perspective, the Gmax performs several key roles in controlling the relationship between the pelvis, trunk, and femur. This muscle is capable of abducting and laterally rotating the hip, which helps to control the alignment of the knee with the lower limb. For example, in stair climbing, the Gmax will laterally rotate and abduct the hip to keep the lower limb in optimal alignment, while at the same time the hip extends to carry the body upward onto the next step. When the Gmax is weak or misfiring, the knee can be seen to deviate medially and the pelvis can also be observed to tip laterally.
The Gmax also has a role in stabilizing the SIJs and has been described as one of the force closure muscles. Some of the Gmax fibers directly attach to the sacrotuberous ligament and the thoracolumbar fascia, which is a very strong, non-contractile connective tissue that is tensioned by the activation of muscles connecting to it. One of the connections to this fascia is the latissimus dorsi, and the Gmax forms a partnership with the contralateral (opposite) latissimus dorsi via the thoracolumbar fascia—this partnership connection is known as the posterior oblique sling (see Figure 9.10), which was discussed in Chapter 3. This sling increases the compression force to the SIJ during the weight-bearing single-leg stance in the gait/walking cycle.
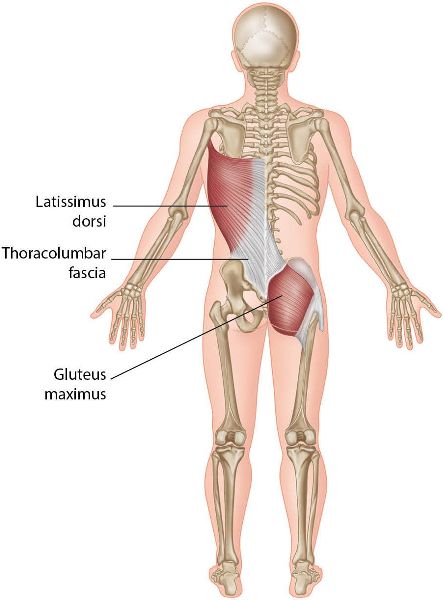
Figure 9.10. Posterior oblique sling and the connection with the latissimus dorsi.
Misfiring or weakness in the Gmax reduces the effectiveness of the posterior oblique sling; this will predispose the SIJs to subsequent injury. The body will then try to compensate for this weakness by increasing tension via the thoracolumbar fascia by in turn increasing the activation of the contralateral latissimus dorsi. As with any compensatory mechanism, “structure affects function” and “function affects structure.” This means that other areas of the body are affected: for example, the shoulder mechanics are altered, since the latissimus dorsi has attachments on the humerus and scapula. If the latissimus dorsi is particularly active because of the compensation, this can be observed as one shoulder appearing lower than the other during a step-up or a lunge type of motion.
As explained in Chapter 4, the Gmax plays a significant role in the gait cycle, working in conjunction with the hamstrings. Just before heel-strike, the hamstrings will activate, which will increase the tension to the SIJs via the attachment on the sacrotuberous ligament. This connection assists in the self-locking mechanism of the SIJs for the weight-bearing cycle. The interval of the gait cycle from heel-strike to mid-stance is where the tension in the hamstrings should decrease through the natural anterior rotation of the innominate, as well as through the slackening of the sacrotuberous ligament. The activation of the Gmax now increases while that of the hamstrings decreases in order to initiate the action of hip extension. The Gmax significantly increases the stabilization of the SIJs during the early and mid-stance phases through the attachments of the posterior oblique sling.
Weakness or misfiring in the Gmax will cause the hamstrings to remain active during the gait cycle in order to maintain stability of the SIJs and the position of the pelvis. The resultant overactivation of the hamstrings will subject them to continual and abnormal strain.
As I mentioned earlier, the focus of this chapter is to look at what happens to the function of the pelvis when the glutes become weakened through inhibition; we looked at the Gmin earlier, so in this section we will concentrate on the Gmax. This phasic muscle has a tendency to follow a trait of becoming weakened if the antagonistic muscles have become short and tight or if there are any underlying pelvic malalignments. However, the Gmax can also test weak if there is a neurological disorder, such as a herniated disc (Chapter 10), affecting the L5 and S1 nerve root (which innervates the Gmax muscle). Any type of hip joint pathology—for example an acetabular labral tear (Chapter 8) or joint capsulitis—can also cause an inhibition weakness in the Gmax.
The main muscles that can potentially cause a weakness inhibition in the Gmax are the iliopsoas, rectus femoris, and adductors, as they all are classified as hip flexors, which are the antagonistic muscles to the hip extension action of the Gmax.
The assessment of the iliopsoas and other associated shortened antagonistic muscles using the modified Thomas test has already been discussed in Chapter 7. Once that assessment has been fully understood, you will need to normalize the tight and shortened antagonistic muscles by the use of METs. After mastering and applying these advanced techniques, the physical therapist will be able to incorporate them into their own treatment modality, with the aim of encouraging the lengthening of the tight tissues. This will then promote a normal neutral position of the pelvis and lumbar spine, and in turn hopefully have the effect of “switching” the weakened Gmax back on.
Assessment of the Gmax
In this section I will discuss the hip extension firing pattern test, which is used for determining the correct firing order of the hip extensors (including the Gmax muscle). The aim of the test is to ascertain the actual firing sequence of a group of muscles, to ensure that all are firing correctly, just like the cylinders of an engine. A misfiring pattern will commonly be found in athletes and patients.
Figure 9.11 shows the correct firing pattern in hip joint extension. The normal muscle activation sequence is:
• Gmax
• Hamstrings
• Contralateral lumbar extensors
• Ipsilateral lumbar extensors
• Contralateral thoracolumbar extensors
• Ipsilateral thoracolumbar extensors
The hip extension firing pattern test is unique in its application. Think of yourself as a car with six cylinders in your engine: basically that is what your body is—an engine. The engine has a certain way of firing and so does your body. For example, the engine in a car will not fire its individual cylinders in the numerical order 1–2–3–4–5–6; it will fire in a predefined optimum sequence, say 1–3–5–6–4–2. If we have our car serviced and the mechanic mistakes two of the spark plug leads and puts them back incorrectly, the engine will still work but not very efficiently; moreover, it will eventually break down. Our bodies are no different: in our case, if we are particularly active but have a misfiring dysfunction, our bodies will also break down, ultimately causing us pain.
Hip Extension Firing Pattern Test
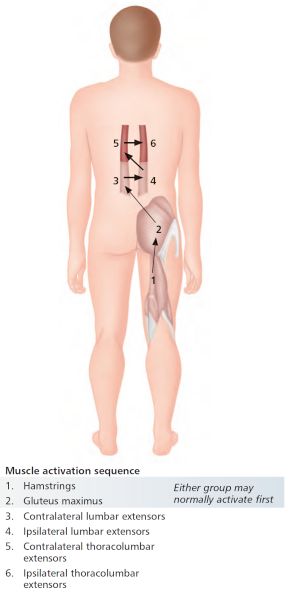
Figure 9.11. Correct firing pattern in hip joint extension.
Sequence 1
The therapist places their fingertips lightly on the patient’s left hamstrings and left Gmax (Figures 9.12(a) and (b)), and the patient is asked to lift their left leg 2” (5cm) off the couch (Figure 9.12(c)). The therapist tries to identify which muscle fires first and notes the result of this first sequence (Table A1.1 in Appendix 1 can be used for this).
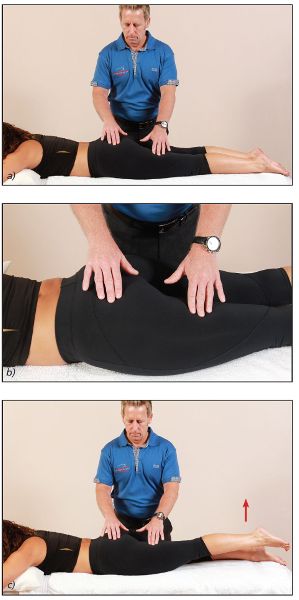
Figure 9.12. Hip extension firing pattern—sequence 1: (a) The therapist lightly palpates the patient’s left hamstrings and Gmax; (b) Close-up view of the therapist’s hand position; (c) The patient lifts their left leg off the couch.
Sequence 2
The therapist places their thumbs lightly on the patient’s erector spinae, and the patient is asked to lift their left leg 2” off the couch (Figure 9.13(a) and (b)). The therapist identifies and notes (in Table A1.1 in Appendix 1) which erector muscle fires first.
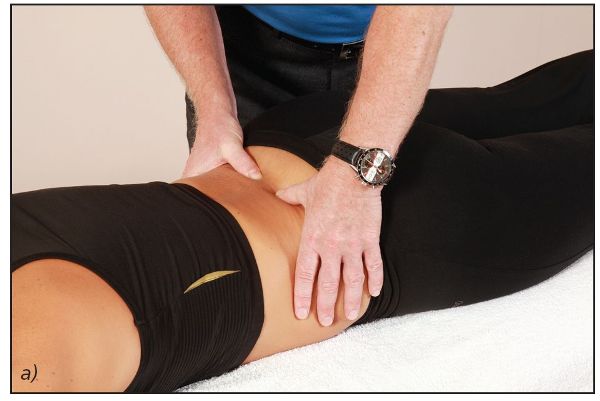
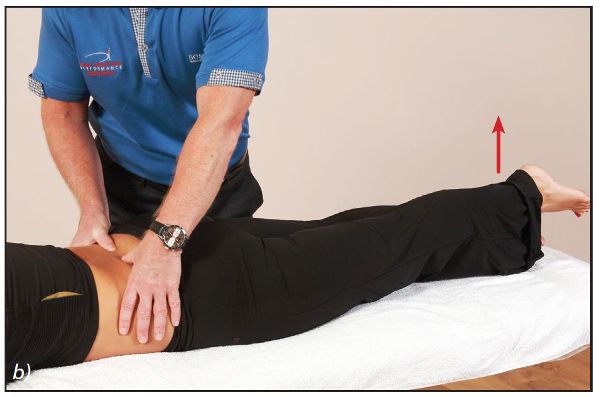
Figure 9.13. Hip extension firing pattern—sequence 2: (a) The therapist lightly palpates the patient’s erector spinae; (b) The patient lifts their left leg off the couch.
Sequences 1 and 2 are then repeated with the right leg, and the results recorded (in Table A1.2 in Appendix 1). Having done this, the therapist can determine whether or not the muscles are firing correctly. The firing pattern should be: (1) Gmax, (2) hamstrings, (3) contralateral erector spinae, and (4) ipsilateral erector spinae.
If, when palpating in sequence 1, the Gmax is found to fire first, you can safely say that this is correct. The same applies in sequence 2: if the contralateral erector spinae contracts first, this is also the correct sequence.
| 1st | 2nd | 3rd | 4th | |
|---|---|---|---|---|
|
Gluteus maximus |
○ |
○ |
○ |
○ |
|
Hamstrings |
○ |
○ |
○ |
○ |
|
Contralateral erector spinae |
○ |
○ |
○ |
○ |
|
Ipsilateral erector spinae |
○ |
○ |
○ |
○ |
Table 9.1: Hip extension firing pattern—left side.
| 1st | 2nd | 3rd | 4th | |
|---|---|---|---|---|
|
Gluteus maximus |
○ |
○ |
○ |
○ |
|
Hamstrings |
○ |
○ |
○ |
○ |
|
Contralateral erector spinae |
○ |
○ |
○ |
○ |
|
Ipsilateral erector spinae |
○ |
○ |
○ |
○ |
Table 9.2: Hip extension firing pattern—right side.
However, if you feel that the hamstrings are number 1 in the sequence, or that the ipsilateral erector spinae is number 1 and the Gmax is not felt to contract, you can deduce that this is a misfiring pattern. If the misfiring dysfunction is not corrected, the body (like the engine) will start to break down and a compensatory pattern of dysfunction will be created.
In my experience, I have found that in a lot of patients, the hamstrings and the ipsilateral erector spinae are typically first to contract and the Gmax is fourth in the sequence. In these cases the erector spinae and the hamstrings will become the dominant muscles in assisting the hip in an extension movement. This can cause excessive anterior tilting of the pelvis, with a resultant hyperlordosis, which can lead to inflammation of the lower lumbar facet joints.
Note: The firing patterns of muscles 5 and 6 have not been discussed in this chapter, because we need to make sure that the correct firing order of muscles 1–4 is established. I also find that when the muscle 1–4 firing sequence has been corrected, the firing pattern of muscles 5 and 6 is generally self-correcting and tends to follow the normal firing pattern sequence.
Another factor that can affect firing order is a previous injury. Bullock-Saxton et al. (1994) investigated the timing of the posterior trunk and leg muscles during hip extension firing, and the influence of a previous ankle sprain on the firing order. Those authors found a significant difference in the onset of Gmax activity (delayed onset) in the group with ankle sprain history compared with the control group.
Gait Cycle Continued
A weak or misfiring Gmax might lead to the creation of several compensatory patterns. First of all, let’s look at the case where a patient has a weak Gmax, potentially caused by weakness inhibition, commonly known as reciprocal inhibition (RI), through the antagonistic tightness of the iliopsoas, rectus femoris, and adductors. This soft tissue tightness of the anterior muscles will limit the amount of extension of the hip joint during the gait cycle. As compensatory reactions the innominate bone will be forced to rotate more into an anterior position, and the contralateral innominate will be forced to rotate further into a posterior position. The hamstrings, and in particular the biceps femoris, will be part of the compensation pattern by assisting the increased anterior rotation of the innominate as a result of the weakness of the Gmax. Sahrman (2002) suggested that if the hamstrings are dominant because of inhibition of the Gmax, an anterior shear of the trochanter could be palpated during the prone leg extension.
This now gets a little complex (but has already been explained in previous chapters), as the bit in between the two innominate bones, i.e. the sacrum, will now have to rotate and side bend a bit more than normal because of the increased innominate rotation. The sacrum will now have to compensate by increasing its torsion (rotate one way and side bend the other) in one direction; this will be either a L-on-L sacral torsion (left rotation on the left oblique axis), as shown in Figure 9.14(a), or a R-on-R sacral torsion (right rotation on the right oblique axis), as shown in Figure 9.14(b). The lumbar spine will also have to compensate by potentially counter-rotating a bit more in the opposite direction to the sacrum, as shown in the two Figures.
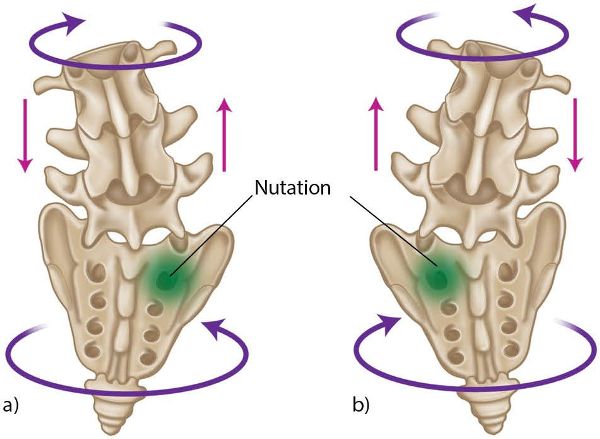
Figure 9.14. Sacral torsion: (a) L-on-L; (b) R-on-R.
There is a natural rotation of the sacral and lumbar spines during the gait cycle; however, because of the increased innominate rotation, the sacrum and lumbar spines have no choice but to compensate as well. In between the lumbar spine and the sacrum (L5 and S1) there lies an intervertebral disc (Chapter 10); imagine now this disc being “torqued” between the two spinal segments. This action will have a negative effect on the disc—it is like squeezing water out of a sponge, and discs do not like that type of increased motion!
One way of potentially correcting the misfiring sequence is as follows. Through muscle length testing (modified Thomas test), we need to first determine which muscles are actually held in a shortened position; METs (Chapter 7) and specific myofascial release techniques (see Gibbons (2014) for demonstrations of these) can then be used to treat and normalize these shortened and tight tissues.
Remember what I talked about earlier: any underlying malalignment position of the pelvic girdle can be another causative factor in the weakness inhibition of the Gmax. Bear that in mind, especially when trying to correct the misfiring sequence.
Thoracolumbar Fascia and Its Relationship to the Gmax and Pelvis
The thoracolumbar fascia is a thick, strong sheet of a ligamentous type of connective tissue, which connects with, and covers, the muscles of the trunk, hips, and shoulders. The normal function of the Gmax will be to exert a pulling action on the fascia, thereby tensing its lower end, as shown in Figure 9.15; you can see from the diagram that there is a connection between the Gmax and the contralateral latissimus dorsi muscle by means of the posterior layer of the thoracolumbar fascia. Both of these muscles conduct the forces contralaterally (i.e. to the opposite side) during the gait cycle (via the posterior oblique sling), which then causes increased tension through the thoracolumbar fascia. This function is very important for rotation of the trunk and for force closure stabilization of the lower lumbar spine and the SIJ.
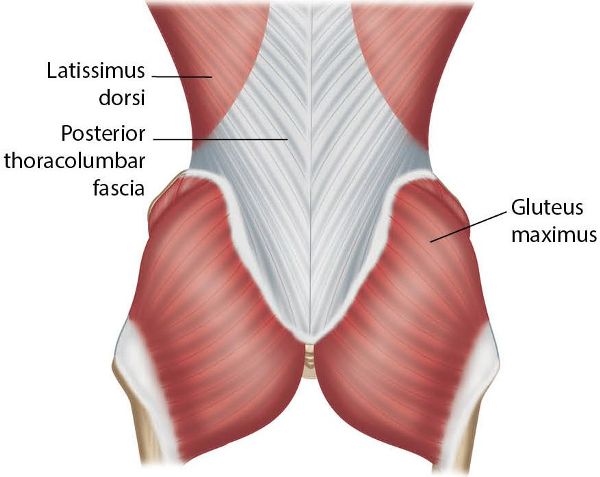
Figure 9.15. The thoracolumbar fascia and the connection to the Gmax.
There is also a co-contraction of the deeper muscles of lumbar stability—i.e. the TVA and the multifidus. These muscles co-contract when you move a limb and were discussed in Chapter 3. As far as I am aware, there has been nothing published recently about the TVA and multifidus being specifically triggered by engagement of the Gmax. However, I personally believe that the TVA muscle definitely responds to Gmax contraction, and I suspect that the multifidus does too, as they all have an association with the sacrotuberous ligament of the pelvis (either directly or indirectly), which assists in force closure of the SIJ.
Case Study
This case study, I hope, emphasizes that the relationship of the glutes to the SIJ is the key link in the patient’s presenting symptoms.
The patient was a 34-year-old woman and a physical trainer for the Royal Air Force. She presented to the clinic with pain near the superior aspect of her left scapula (Figure 9.16). The pain would come on four miles (6.5km) into a run, forcing her to stop because it was so intense. The discomfort would then subside, but quickly return if she attempted to start running again. Running was the only activity that caused the pain. Her complaint had been ongoing for eight months, had worsened over the past three, and was starting to affect her work. There was no previous history or related trauma to trigger the complaint.
After seeing different practitioners, who all focused their treatment on the upper trapezius, she visited an osteopath who treated her cervical spine and rib area. The treatments she had received were biased toward the application of soft tissue techniques to the affected area, namely the trapezius, levator scapulae, sternocleidomastoid (SCM), scalenes, and so on. The osteopath had also used manipulative techniques on the facet joints of her cervical spine—C4/5 and C5/6. METs and trigger point releases were used in a localized area, which offered relief at the time but made no difference when she attempted to run more than four miles. She had not undergone any scans (e.g. MRI or X-ray).
Taking a Holistic Approach
Let’s now assess the case study patient globally rather than locally, remembering that the pain only comes on after running four miles.
When I see a new patient for the first time, no matter what the presenting pain is, I normally assess the pelvis for position and movement, as I consider this area of the body in particular to be the “foundation” for everything that connects to it. I often find in the clinic that when I correct a dysfunctional pelvis, my client’s presenting symptoms tend to settle down. However, when I assessed this particular patient, I found her pelvis was level and moving correctly.
I then went on to test the firing patterns of the Gmax (explained earlier), which I often do with patients and athletes who participate in regular sporting activities. However, I only test the firing pattern sequence once I feel that the pelvis is in its correct position; the logic here is that you often get a positive result of the muscle misfiring when the pelvis is slightly out of position.
With the patient in question, I found a bilateral weakness/misfiring of the Gmax, but the firing on the right side seemed a bit slower than on her left side. As I had not found any dysfunction in the pelvis, I pursued this line of approach a little further.
Before we continue I would like to put a few questions to you to think about:
• How does a weakness of the Gmax on the right side cause pain in the left trapezius?
• Is there a link between the Gmax and the trapezius, and if so, how is this possible?
• What can be done to correct the issue?
• What has happened to cause it in the first place?
Gmax Function
Remember from earlier, the Gmax operates mainly as a powerful hip extensor and a lateral rotator, but it also plays a part in stabilizing the SIJ by helping it to force close while going through the gait cycle. Some of the Gmax muscular fibers attach to the sacrotuberous ligament, which runs from the sacrum to the ischial tuberosity, and this ligament has been termed the key ligament in helping to stabilize the SIJ.
Linking it All Together
So what do we know? We know that the right side of the patient’s Gmax is slightly slower in terms of its firing pattern and that this muscle plays a role in the force closure process of the SIJ. This tells us that if the Gmax cannot perform this function of stabilizing the SIJ, then something else will assist in stabilizing the joint. The left latissimus dorsi is the synergist that helps stabilize the right Gmax (Figure 9.10) and, more importantly, the SIJ. As the patient participates in running, every time her right leg contacts the ground and goes through the gait cycle, the left latissimus dorsi is over-contracting. This causes the left scapula to depress, and the muscles that resist the downward depressive pull will be the upper trapezius and the levator scapulae. Subsequently, these muscles start to fatigue; for the patient in question, this occurs at approximately four miles, at which point she feels pain in her left superior scapula.
Treatment
You might think the easy way to treat the weakness in the Gmax is to simply prescribe strength-based exercises. However, in practice this is not always the correct solution, as sometimes the tighter antagonistic muscle is responsible for the apparent weakness. The muscle in this case is the iliopsoas (hip flexor), and its shortening can result in a weakness inhibition of the Gmax. My answer to this puzzle was to lengthen the patient’s right iliopsoas muscle (Chapter 7) to see if it promoted the firing activation of the Gmax, while at the same time introducing simple strength exercises for the Gmax.
Prognosis
I advised the patient to abstain from running and to get her partner to assist in lengthening the iliopsoas, rectus femoris, and adductors using METs (Chapter 7) twice a day. Strength and stability exercises for the outer core muscles (Chapter 3) were also advised once daily until the follow-on treatment. I reassessed her 10 days later and found the firing sequence of the Gmax to be normal in the hip extension firing pattern test, and a reduction in the tightness of the associated iliopsoas, rectus femoris, and adductors. Because of these encouraging results, I advised her to run as far as felt comfortable. I was not sure if my treatment was going to correct the problem, but she reported that she had no pain during or after a six-mile (10km) run. The patient is still pain free and continues to regularly use the strengthening exercises for the Gmax and the lengthening techniques for the short/tight muscles.
Conclusion
This case study demonstrates that very often the underlying cause of a condition or problem may not be local to where the symptoms/pain presents, which means that all avenues need to be fully considered.
I hope that the information from this case study has intrigued you enough to continue reading. I would like to think that when you next assess and treat one of your patients, you will look at them in a slightly different way to what you normally would.
___________
I think of this book (and all the books I have written) as taking you on what I call a jigsaw puzzle journey—if you stick with it, the picture will eventually become a lot clearer.
After reading this chapter and the above case study, you should have a better understanding of the situation that if the glutes are weak or misfiring, their function (the Gmax’s in particular) of tensing the thoracolumbar fascia is reduced, which will cause a natural overactivation of the contralateral latissimus and the ipsilateral multifidus. A weakness inhibition of the Gmax and Gmed will over-stimulate other compensatory mechanisms throughout the whole of the kinetic chain, all of which will naturally in some way or other have an effect on the functionality and stability of the pelvis.
